Are you among the many who believe that maintaining stable blood sugars by consuming fewer carbs is the key to fat loss?
It’s a common belief in keto circles, driven by the fear of insulin’s purported fat-storage effects. However, this article unravels the misconception and sheds light on why a high-fat diet aimed at stabilizing blood sugar might not lead you to the weight loss results you desire.
Discover the real relationship between fat, insulin, and your metabolic health, along with data-driven insights that could redefine your approach to achieving your weight loss and health goals.
- Background
- What We Know From People With Type 1 Diabetes
- How Insulin Really Works
- The Difference Between People with Type 1 Diabetes and Everyone Else!
- But What if I’m ‘Insulin Resistant’?
- Show Me the Science!
- Flatline Blood Sugar Envy… We’re Still Chasing the Wrong Numbers
- How Much Should My Blood Sugars Rise After a Meal?
- Stable Blood Glucose Does Not Equal Fat Loss!
- Blood Glucose Variability
- Pre-Meal Trigger
- Doesn’t WHAT I Eat Matter Too?
- Avoiding Blood Sugar Spikes is Only the First Step
- The Bottom Line
- More
Background
If there was anything I thought I knew for sure when I was an insulin-fearing keto zealot, it was that:
- the blood sugar rollercoaster is bad and
- stable blood sugars were good.
According to the keto gurus that I was following, if you want to lose fat and optimise your metabolic health, the most important thing you could do was to eat fewer carbs to achieve flatline blood sugars and ‘turn off your insulin’.
Even today, there is still plenty of confusion about the role of stable blood sugars and insulin levels in weight loss.
Many people incorrectly assume that super-stable blood sugars will lead to lower insulin levels, automatically leading to fat loss.
Since we started Data-Driven Fasting, I have had a barrage of questions as people try to make sense of their blood sugars. Now that thousands of people have completed their baselining phase of Data-Driven Fasting, we have data demonstrating that eating a high-fat diet to stabilise your blood sugar is unlikely to help you lose weight.
Rather than worrying about your blood glucose after meals, your blood glucose before meals is a more powerful way to optimise your metabolic health. By actively managing your blood glucose levels before you eat (through meal timing and nutrient-focused foods and meals), you can optimise the numbers that matter when managing your metabolic health (i.e. BMI, waist-to-height ratio and waking blood sugars).
What We Know From People With Type 1 Diabetes
For someone with Type 1 Diabetes, injecting large doses of insulin to treat elevated blood sugars from modern processed food leaves them on a blood sugar rollercoaster. When their blood sugars are high, they inject more insulin to bring their blood sugars down.
A few hours later, when they find they have overshot their blood sugar target, they are ravenously hungry and will eat anything and everything in sight until they can raise their blood sugars again. A day in the life of most people living with Type 1 Diabetes looks like this. In this scenario, injected insulin is driving their appetite and causing them to eat more.
If their insulin doses are not precisely matched with the food they eat (which is nearly impossible with synthetic, injected insulin combined with synthetic, processed food), they end up overeating because of the insulin they are injecting.
Living with rollercoaster blood sugars sucks – appetite, mood or energy levels are in the toilet!
How Insulin Really Works
While we often think of insulin as the hormone that jams energy into our cells, it’s not the whole story.
We all have about 5 grams of glucose (about a teaspoon or 20 calories worth) buzzing around in our bloodstream at any one time. It doesn’t take long to use this up once we turn off the flow of energy into our bloodstream.
If you could turn off the release of energy from your liver completely, you would run out of glucose in about 15 minutes.
Insulin is secreted by the pancreas that turns off the flow of stored energy into your bloodstream (from your liver and adipose tissue) until you burn up the energy in your blood from that last meal.
So, rather than thinking of insulin as an anabolic hormone (i.e. it helps things to grow), it’s much more helpful to focus on its function as an anti-catabolic hormone (i.e. it stops us from breaking down and disintegrating).
As per Dr Bernstein’s Law of Small Numbers, once people with Type 1 Diabetes reduce the significant inputs of processed carbohydrates that require large doses of insulin, they can stabilise their blood sugars and insulin requirements.
Smaller inputs of carbs and insulin lead to smaller errors that are easier to correct throughout the day. When they are no longer injecting massive amounts of insulin to treat the blood sugar rollercoaster, their appetite stabilises, and they tend to achieve healthy body fat levels.
If you are part of the one in 8000 people with Type 1 Diabetes whose pancreas doesn’t work, stabilising your blood sugars and insulin by manipulating your diet should be your highest priority.
The Difference Between People with Type 1 Diabetes and Everyone Else!
If you are part of the 99.5% of the population that is fortunate enough to have a functioning pancreas, EVERYTHING is different.
You cannot turn off your insulin pump or stop injecting insulin. No matter what we’d like to believe, it just doesn’t work like that.
Your pancreas will always produce just enough insulin (no more, no less) to hold your body fat in storage until you have used up the extra energy from the food coming in from your mouth. Then, when you stop eating, insulin levels lower and your stored energy is allowed to be released for use.
If you have Type 2 Diabetes and eat a diet of heavily processed carbs and fat (e.g. modern processed junk food), your blood sugars will shoot up after eating and take a long time to come back down.
But What if I’m ‘Insulin Resistant’?
‘Insulin resistance’ is a term that is used a lot in low-carb and keto circles. But why we become insulin resistant and how to reverse it is not yet commonly understood. Many people think they are obese because they are insulin-resistant. But the reverse is true. They are insulin-resistant because they are obese.
When your fat cells (which make up your adipose tissue) fill up (like a sponge or a balloon), it becomes harder to force more energy into them. As a result, your pancreas must raise insulin levels more and more to enable your body to continue to store excess energy. Because we need more and more insulin to do the job, the fat cells appear to have become resistant to the effects of insulin, and thus, we say we have become insulin resistant.
Many people develop a victim mentality (I was one of them), believing that they are insulin-resistant. They blame their obesity on their insulin resistance (not the other way around). They think being insulin-resistant makes it harder for them to lose weight, but the reverse is true.
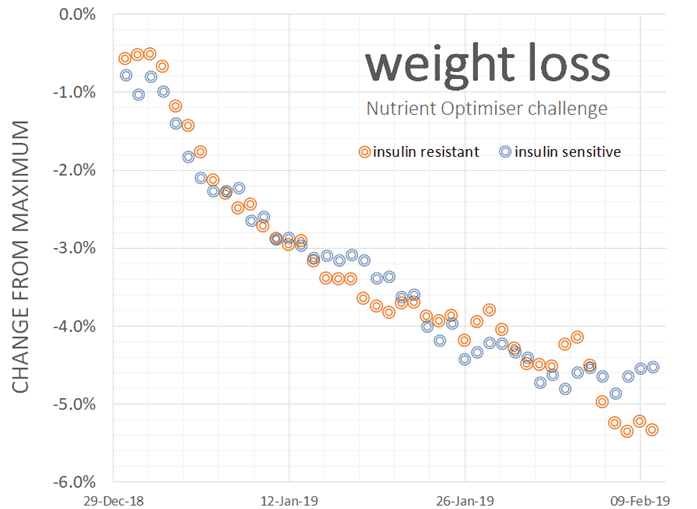
This chart shows the weight loss in our first Macros Masterclass for people who identified themselves as insulin resistant vs insulin sensitive. It was interesting to see that people who identified themselves as insulin-resistant lost weight at a similar rate as everybody else. In the end, it was actually the people who believed they were insulin-resistant who lost slightly more weight.
When you are lean and insulin-sensitive, your body is eager to store energy and grow. However, once you become insulin resistant, your body is only too willing to offload the excess energy as soon as you stop jamming in low-satiety, nutrient-poor processed foods.
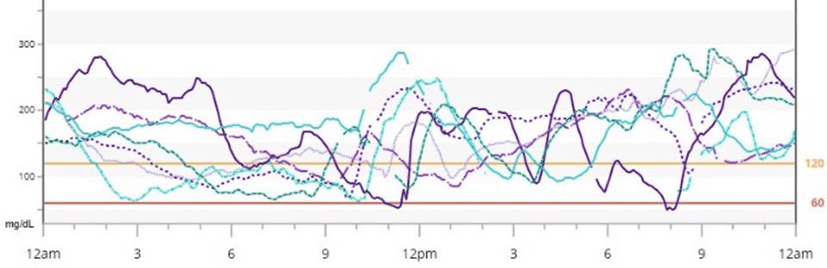
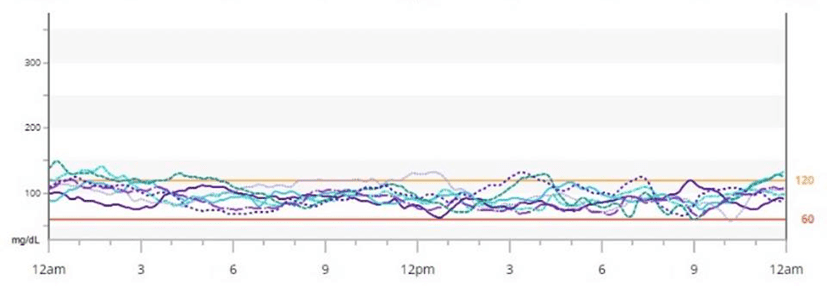
The chart below shows the difference between diabetic and healthy blood sugar levels (i.e. higher and with bigger swings). Foods that are a combination of fat+carb together enable your body to fill both fuel tanks at the same time. Because your fat stores are already full, the extra energy is not easily absorbed by your liver and body fat, so it overflows into your bloodstream.
You can’t blame getting fat on insulin. It’s the nutrient-poor foods with carbs and fat (together with low protein) that cause you to overeat and gain fat. The increase in insulin is simply the consequence of storing more energy on your body.
Once you’re carrying extra body fat, you require lots of extra insulin to hold it in. Understanding the cause-and-effect relationship is critical to designing the correct dietary solution.
It’s not that stable blood sugars are a bad thing. But simply switching carbs for fat to achieve stable blood sugars is nothing more than symptom management. It won’t make you lean and metabolically healthy and may even make things worse!
Show Me the Science!
Since launching the Data-Driven Fasting, we have been bombarded with questions about blood sugars and insulin as people test their blood sugars and try to make sense of the data they see.
- Why do my blood sugars rise when I don’t eat?
- How much should my blood sugars rise after I eat?
- My blood sugars are flatline? Why am I not losing fat?
With data from hundreds of people, I have been able to understand if there is really a relationship between more stable blood sugars and fat loss.
Flatline Blood Sugar Envy… We’re Still Chasing the Wrong Numbers
Many people believe that maintaining stable blood glucose levels is the highest priority and will lead to weight loss.
I’m seeing more and more people (who don’t have Type 1 Diabetes) walking around with (expensive and sometimes painful) continuous glucose monitors (CGMs) eating more fat and less protein and carbs to make sure they maintain flatline blood sugars. They proudly post their flatline blood sugars on Facebook and Instagram.
How Much Should My Blood Sugars Rise After a Meal?
To help us understand how much our blood sugar should rise after a meal, the table below shows the generally accepted limits for blood glucose.
If your blood sugars after meals are elevated above 7.8 mmol/L (140 mg/dL), then you have prediabetes or diabetes and need to work to reduce your post-meal blood glucose by reducing refined carbohydrates and/or medications to reduce blood sugars. This maximum peak usually occurs within an hour or two after you eat, depending on the type of food.
A rise in glucose from 5.6 mmol/L to 7.8 mmol/L (100 mg/dL to 140 mg/dL) would be accepted as normal and healthy. If your blood sugars rise by less than 2.6 mmol/L or 40 mg/dL, then it’s highly likely you have a fully functioning pancreas, and you would benefit by focusing on your blood sugars before you eat (not after) if you have more weight to lose.
In the Macros Masterclass and Data-Driven Fasting, we set even tighter limits than this. We recommend that people reduce the amount of processed carbs in their diet if their blood sugars rise by more than 1.6 mmol/L or 30 mg/dL.
Once your blood sugars are stable, you should move on and focus on nutrient density, satiety and your blood sugars before meals rather than continuing to micromanage the fluctuations in your blood sugars after you eat in the mistaken belief that this will help.
Interestingly, the average rise for people following Data-Driven Fasting is only 10 mg/dL or 0.5 mmol/L, which is not much. It seems people who are fans of fasting (and typically following a low-carb or keto-style diet) already have extremely stable blood sugars! However, many of them still have a lot of fat to lose.
Stable Blood Glucose Does Not Equal Fat Loss!
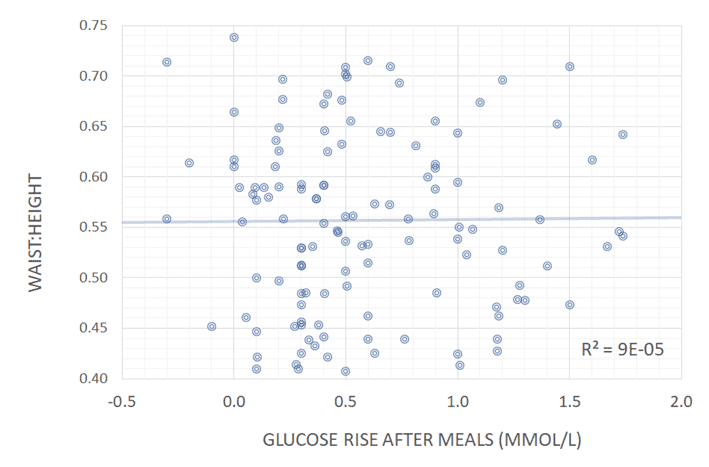
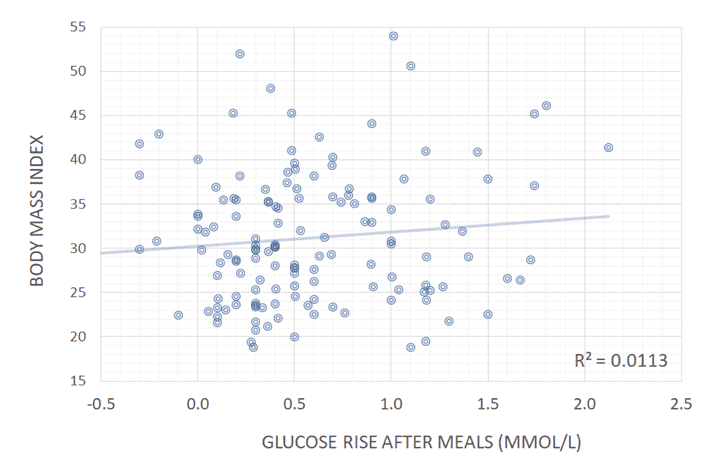
The charts from the data from people using Data-Driven Fasting below show there is no correlation between someone’s waist:height ratio or BMI and their blood sugar after they eat.
There is also no correlation between the amount your blood glucose rises after you eat and your waking blood glucose (another critical marker of metabolic health). Although it’s good to have stable blood sugars in the healthy range, flatline is not better, especially if you have to consume a low satiety, high-fat, nutrient-poor diet to get it!
Although stable and lower blood glucose levels are a positive marker of good metabolic health, merely treating the symptom (i.e. elevated blood sugar) rather than addressing the cause (i.e. energy toxicity and excess body fat) doesn’t help.
Unfortunately, many people who believe fat is a ‘free food’ because it does not raise insulin significantly in the short term after eating end up overeating fat in a misguided effort to maintain stable blood sugar levels. Before long, this can quickly lead to fat gain. Excessive levels of stored energy on the body lead to high insulin levels across the day to hold the fat in storage.
Blood Glucose Variability
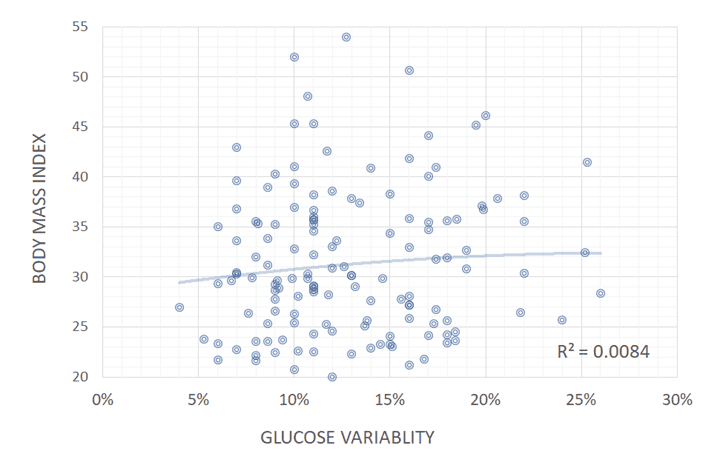
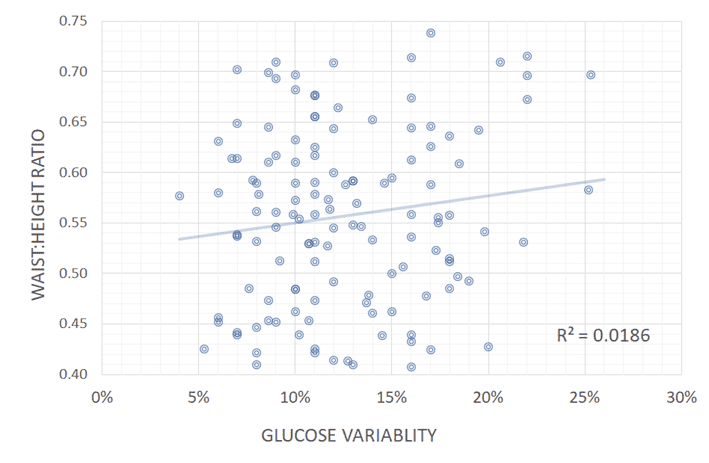
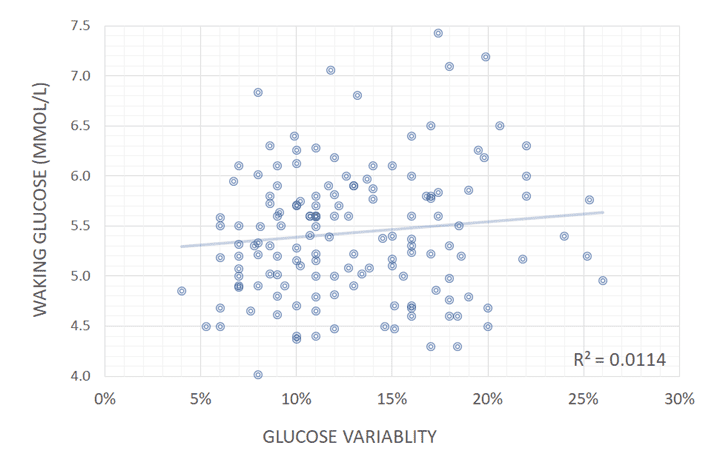
When we look at blood glucose variability (i.e. standard deviation/average glucose), we see there is also a negligible correlation between stable blood sugars and a better waist:height ratio, BMI or waking blood sugars.
Many people combine fasting with a high-fat keto diet to achieve stable blood sugars in the hope of weight loss and/or improved health. But sadly, despite their herculean feats of self-deprivation, they just continue to gain weight due to a low-satiety, nutrient-poor diet that leaves them craving and eating more when they break their fast.
Actively avoiding insulin and rises in blood sugar levels using a high-fat diet tends to lead to poorer satiety, greater energy intake and obesity. In time, these people end up with higher insulin levels across the day because they are carrying more body fat, which requires more insulin to hold in storage.
At this point, you may be thinking that measuring blood sugar is completely useless. This is not what I’m saying. Wild swings in blood sugar outside the normal healthy range are not ideal. But rather than simply being intolerant to carbohydrates, the reality is a large rise in blood glucose after you eat is likely due to fuel (from both fat and glucose) backing up in your system.
A low-carb or keto diet does help to stabilise the swings in blood glucose. However, managing the symptoms of diabetes by trying to achieve minimal blood sugar variation by avoiding all carbs and even protein does not address the root cause and may even make things worse.
Pre-Meal Trigger
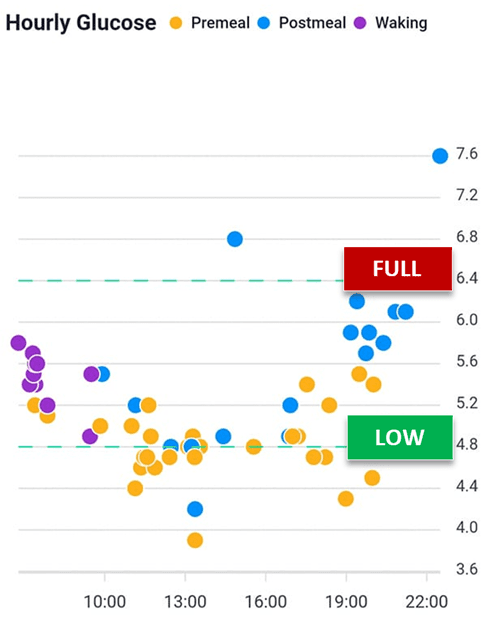
Because glucose is such a volatile fuel and effectively floats on top of all the fat in your body, measuring your blood sugar when you wake or BEFORE YOU EAT is an excellent way to ensure you are not chronically over-fuelling (from either fat or carbs).
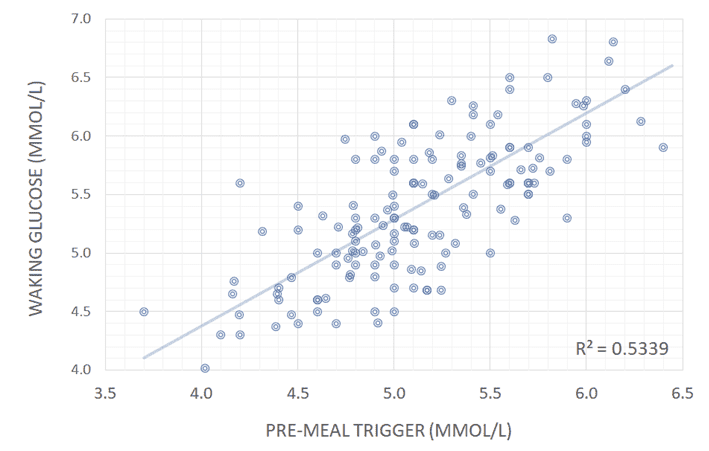
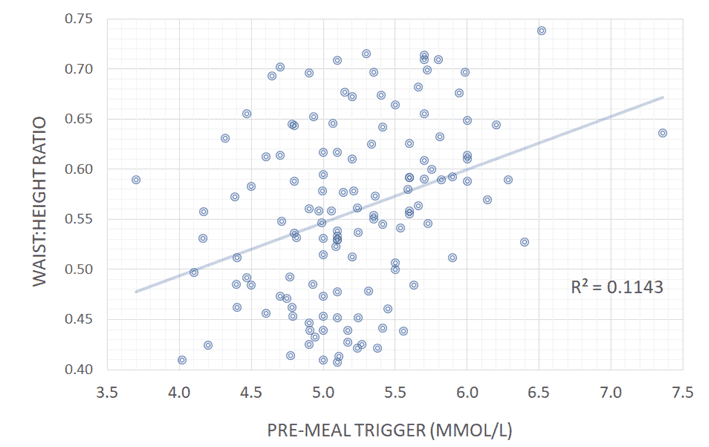
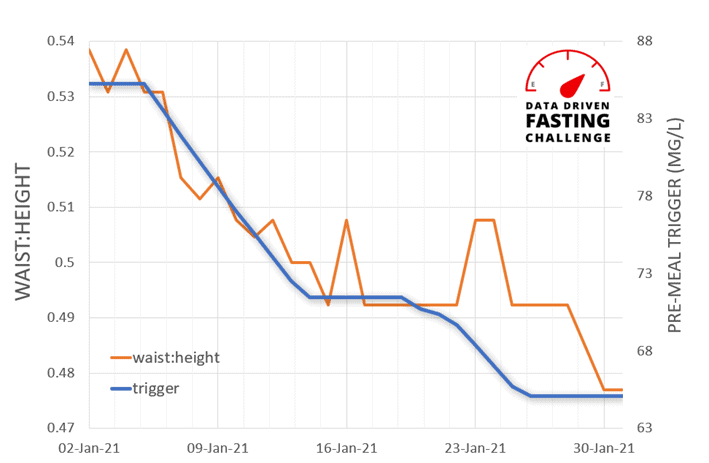
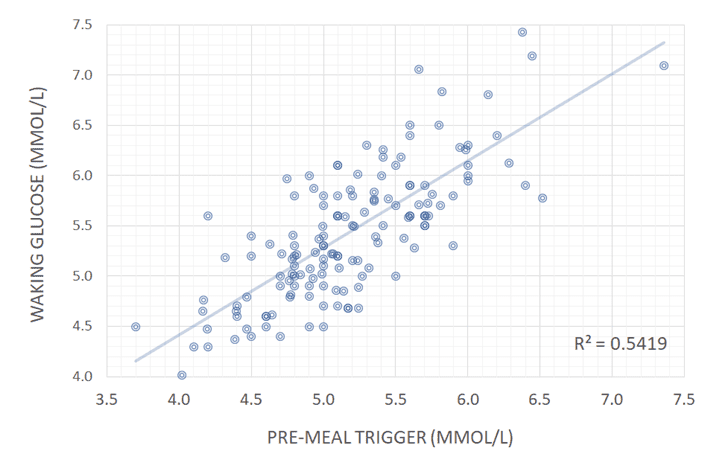
As shown in the charts below, we see a much better correlation between a pre-meal blood glucose trigger and waist:height ratio and waking glucose. Rather than worrying so much about your blood sugars after you eat, it seems that people who have lower blood glucose before they eat tend to have much better metabolic health.
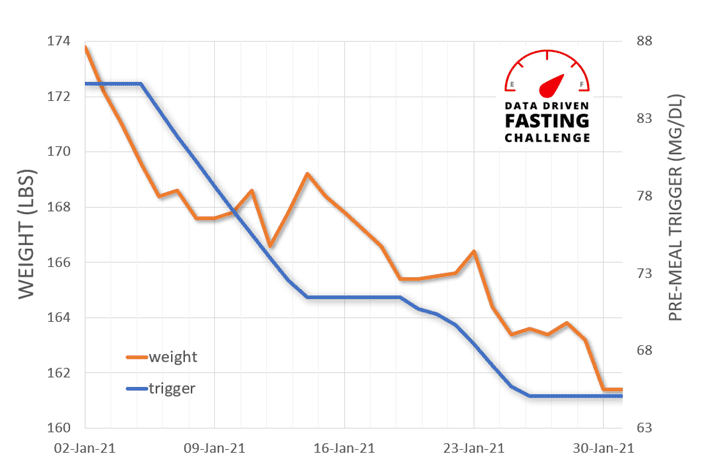
There is some variability across individuals due to different Personal Fat Thresholds. However, when we look at this on a person-by-person basis as they progressively lower their premeal blood sugars (e.g. Jane’s data below), we see that a lower pre-meal blood glucose trigger before you eat aligns nicely with weight and body fat levels.
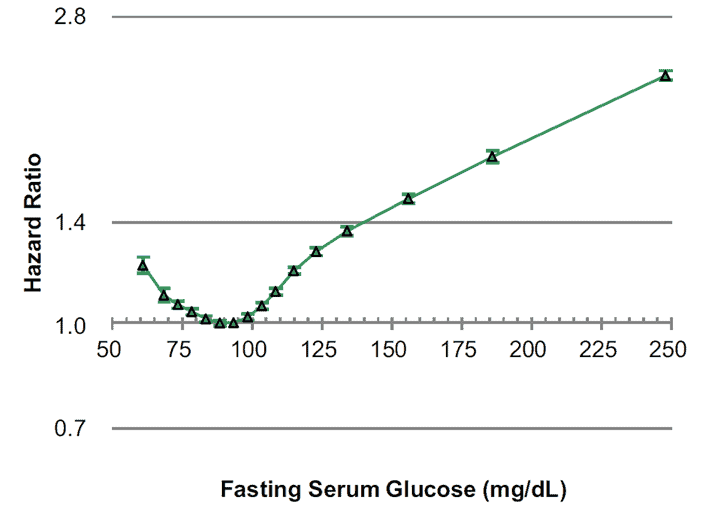
As shown in the chart below (from the Association between fasting glucose and all-cause mortality study), your waking glucose is one of the most powerful indicators of metabolic health and your risk of dying from any cause.
Pre-meal blood glucose trigger strongly correlates with your waking blood glucose. Rather than worrying about the rise in blood glucose after you eat, managing your blood glucose before you eat is much more useful if you want to lose fat and gain health!
To optimise body composition, you need to measure and manage the things that matter. Your blood sugar before meals is an extremely useful thing to measure, and you can manage it by simply optimising your meal timing/intermittent fasting routine to ensure it continues to decrease.
Doesn’t WHAT I Eat Matter Too?
WHAT you eat is arguably more important than WHEN you eat. Data-Driven Fasting simply empowers you to optimise your food timing to ensure a negative energy balance.
- While high-fat foods and meals will keep your blood sugars stable, they also provide a lot of energy, along with lower satiety. Although your blood sugars and insulin levels may be stable, your body won’t need to draw down on your body fat until it burns up all the energy from that fat bomb or buttered coffee.
- Meals with more fast-digesting, non-fibre carbohydrates will raise your blood sugars quickly, but they will likely return to below baseline more quickly as well.
- Foods that contain both fat and carbs together (which are typically also low in protein) will fill your fat and glucose fuel tanks at the same time and allow you to eat more, and keep your blood sugars elevated for longer.
- Foods with a higher percentage of protein and a greater nutrient density are harder to overeat and won’t raise your blood sugars significantly (in fact, they may reduce them). Your blood glucose will return to below target more quickly.
Avoiding Blood Sugar Spikes is Only the First Step
In our Macros Masterclass, we guide people to reduce their carbohydrates if their blood sugars rise more than 30 mg/dL or 1.6 mmol/L after meals. But once they achieve this, there is no benefit in avoiding nutrient-dense foods that may contain some carbohydrates.
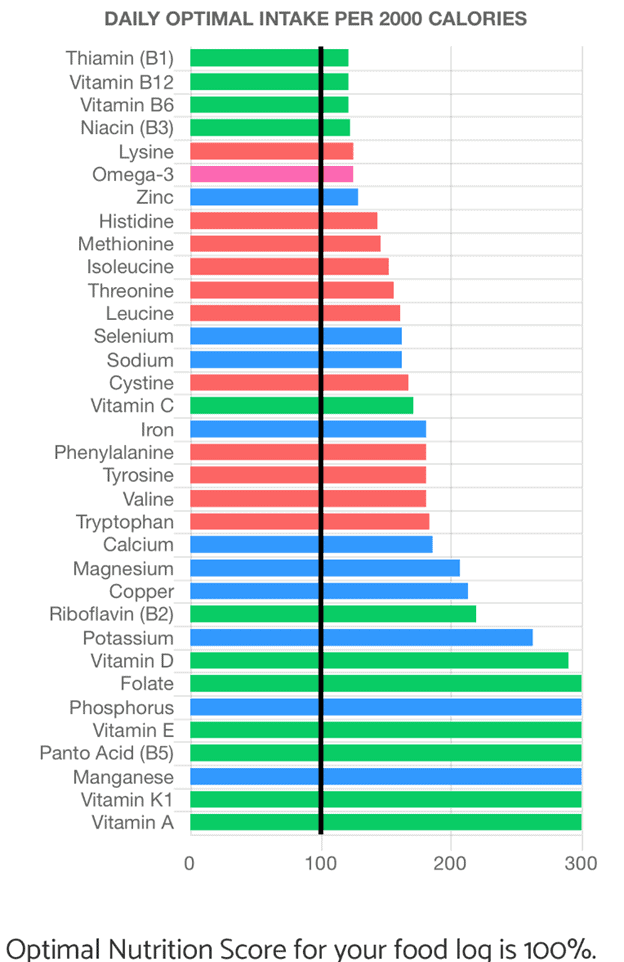
As they fill in their nutrient gaps (by chasing the nutrients they are currently struggling to get enough of, as demonstrated in the nutrient fingerprint chart below) with more nutrient-dense foods, they eliminate all the problematic nutrient-poor processed carbs anyway.
In our Data-Driven Fasting Challenge, we guide people to reduce or eliminate foods and meals that are causing their blood glucose to rise more than 30 mg/dL or 1.6 mmol/L above their current blood sugar trigger. Foods that raise your blood sugar a lot AND keep it elevated for a long time (i.e. fat+carb combo foods) are bad news.
Significantly elevated blood sugars after meals outside the healthy range is a sign that you are overfilling your carb fuel tank AND that your body fat stores are full. We do not recommend people aim for flatline blood sugars as it can lead to simply swapping carbohydrates for low-satiety nutrient-poor added fats.
So, once your blood sugars are in the healthy range, the next step is to simply delay or skip meals to allow your premeal blood sugar to drop below Your Personalised Trigger. Combined with protein/nutrient-focused meals, this allows both your fat and glucose stores to be depleted.
The Bottom Line
- Lower and stable blood sugar and insulin levels are a sign of good metabolic health, but managing the symptoms with a high-fat diet does not lead to greater metabolic health.
- Rather than focusing on avoiding short-term blood sugar and insulin spikes, you should focus on higher-satiety, nutrient-dense foods that will reduce your cravings and allow you to lose body fat.
Get Big Fat Keto Lies!
Get your copy of Big Fat Keto Lies here.
More
- Big Fat Keto Lies: Now On Kindle
- Big Fat Keto Lies: Introduction
- A Brief History of the Low Carb and Keto Movement.
- Keto Lie #1: ‘Optimal ketosis’ is a Goal. More Ketones are Better. The Lie that Started the Keto Movement.
- Keto Lie #2: You Have to be ‘in Ketosis’ to Burn Fat.
- Keto Lie #3: You Should Eat More Fat to Burn More Body Fat.
- Keto Lie #4: Protein Should Be Avoided Due to Gluconeogenesis.
- Keto Lie #5: Fat is a ‘Free Food’ Because it Doesn’t Elicit an Insulin Response.
- Keto Lie #6: Food quality is Not Important. It’s All About Reducing Insulin and Avoiding Carbs.
- Keto Lie #7: Fasting for Longer is Better.
- Keto Lie #8: Insulin Toxicity is Enemy #1.
- Keto Lie #9: Calories Don’t Count.
- Keto Lie #10: Stable Blood Sugars Will Lead to Fat Loss.
- Keto Lie #11: You Should ‘Eat Fat to Satiety’ to Lose Body Fat.
- Keto Lie #12: If in Doubt, Keep Calm and Keto On.
- Resources







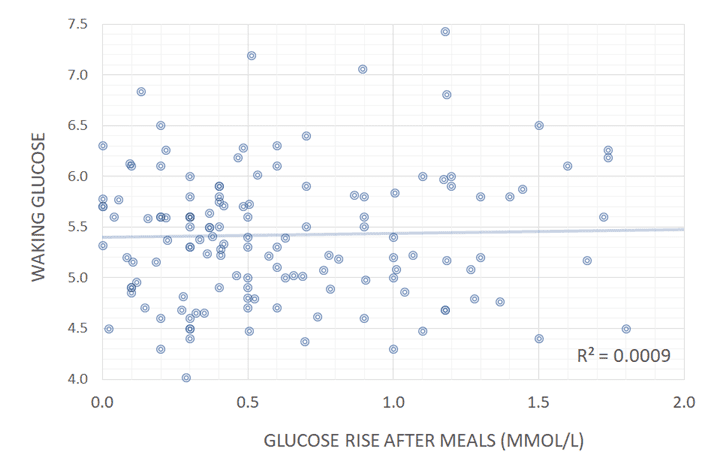

This all info is very interesting, but do you make up all of this by yourself, I mean, on what scientific research and peer-reviewed articles are all this based on? I want to believe in you because everything you write sounds so nice 🙂 but I cannot find any references on what science all your information is based on?
we are fortunate to have our own data to analyse from thousands of people doing our programs. here’s another article covering the concepts. https://optimisingnutrition.com/want-to-lose-fat-dont-aim-for-stable-blood-sugars-your-cgm-is-making-you-fat/