Unlock the secret to supercharging your weight loss journey by understanding the ideal blood sugar levels for weight loss and fat burning! But hold onto your seats because it’s not what you might expect.
Imagine having a personal compass that directs you towards the right food and meal timing, custom-fit for your body. Well, it turns out that your pre-meal blood sugars are the hidden heroes in your quest for weight loss and improved metabolic health, not the usual suspects like waking glucose or post-meal sugar spikes.
Now, you might be wondering, what’s the optimal blood sugar level for fat burning and weight loss? Brace yourself because it’s not a one-size-fits-all answer. It’s all about being a little lower than your personal normal range.
Here’s the scoop: when your glucose dips below your own regular levels, you’re unleashing the power to tap into your stored energy, and yes, that includes that stubborn body fat you’ve been wanting to shed!
In the thrilling journey that follows, we’re going to reveal how you can wield the incredible potential of your blood glucose to dictate not just what’s on your plate but also when you should indulge, all in the name of a consistent and successful weight loss adventure.
So, are you ready to dive into this glucose-guided odyssey?
- What Are the Ideal Blood Sugar Levels for Weight Loss and Overall Health?
- How Do Ideal Blood Sugar Levels for Weight Loss Affect Your Weight Management Journey?
- How Can I Stabilise My Blood Sugar to Lose Weight?
- Will Ketosis Help Me Lose Weight, and What Should Your Glucose Level Be for Ketosis?
- Does Your Body Burn Fat When Your Blood Sugar Is Low?
- What Should Your Glucose Level Be for Weight Loss?
- Will Lowering My Blood Sugar Help Me Lose Weight?
- How Can I Stabilise Blood Sugars and Lose Weight?
What Are the Ideal Blood Sugar Levels for Weight Loss and Overall Health?
Waking and post-meal glucose tend to get most of the attention, so we’ll start by mentioning how they can be helpful and levels considered normal.
Waking Glucose
Understanding the ideal blood sugar levels for weight loss can also guide individuals on how waking glucose levels relate to weight management. Generally speaking, the ideal blood sugar level for a (fasted) healthy person in the morning after you wake is between 70-100 mg/dL (4.4-5.6 mmol/L).
A fasting blood sugar within this range is considered normal, indicating that your body is using the energy you’re getting from food without it backing up into your bloodstream overnight.
For reference, the chart below shows the range of waking glucose values in people in our Data-Driven Fasting Challenges. The average waking glucose in this group of people who are generally metabolically healthy is 103 mg/dL (5.7 mmol/L).
If your waking glucose is on the higher end of this range, you would likely benefit from some weight loss to drain the excess energy your body has stored.
As shown in the image below from our Data-Driven Fasting app, waking glucose decreases as people lose weight. However, it can bounce around from day to day for reasons like poor sleep, where you’re at in your menstrual cycle, or your stress levels.
However, you should be aware of several things that can affect your waking glucose. For example:
- Your waking glucose can be higher if you finish eating later.
- Waking glucose can be higher if you’re on a lower-carb diet, and your blood glucose is lower later in the day. In converse, your waking sugars may be lower early in the day and higher later on if you eat a low-fat diet.
- Some athletes with excellent body composition and low insulin levels also find their glucose is slightly higher than what is considered ‘healthy’ in the morning. This is likely because their body is primed with energy and ready for action.
- Additionally, your waking glucose can rise while you lose weight. As insulin drops, your liver releases stored energy into your bloodstream throughout the night.
So, while your waking glucose can be a valuable marker of your metabolic health over the long term, it’s not useful to guide your progress in the short term.
Post-Meal Blood Glucose
As a general rule of thumb, you don’t want to see your glucose exceed 140 mg/dL (7.8 mmol/L) in the two hours (or more) after you eat. If your glucose rises more than this, it can indicate pre-diabetes or Type-2 Diabetes.
The table below shows the generally accepted cut-offs for pre-diabetes and T2D in mg/dL and mmol/L.
For more on healthy blood glucose levels, check out What Are Normal, Healthy, Non-Diabetic Blood Sugars?
How Do Ideal Blood Sugar Levels for Weight Loss Affect Your Weight Management Journey?
Blood glucose and weight loss have a fascinating relationship. Lean people who are metabolically healthy tend to have lower and more stable blood sugars, which supports fat burning. However, the converse is not true; simply eating to stabilise your blood glucose will not necessarily make you lean and metabolically healthy or empower you to use your stored body fat.
People who are lean and metabolically healthy have plenty of capacity in their liver, muscles, and adipose tissue to store the energy from their food, so the glucose and fat in their blood stay low.
Meanwhile, people who are not so metabolically healthy have overfilled their fat and glucose fuel tanks. Subsequently, they often find that the energy from the food they eat overflows into their bloodstream. This shows up on their glucometer as a considerable rise in glucose after they eat.
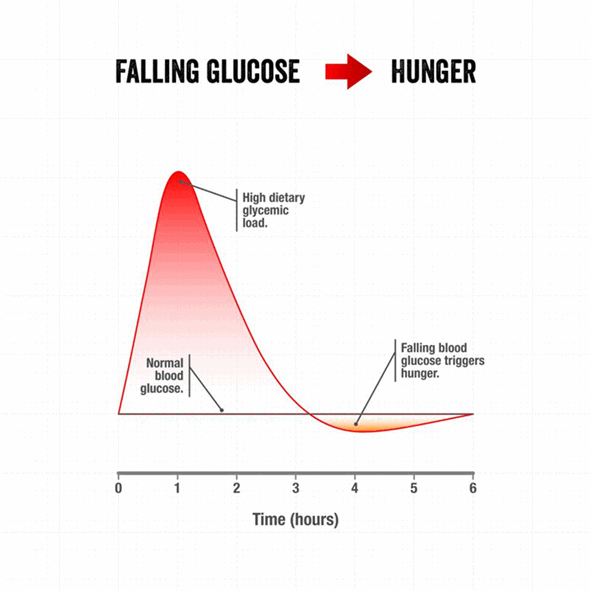
Tracking your glucose the hour or two after you eat can help you understand if you consume more carbohydrates than your body needs. If your glucose rises by more than 30 mg/dL (1.6 mmol/L) after you eat, there’s also a greater risk that it will come crashing down soon after. This significant rise in glucose, followed by a rapid crash, is known as reactive hypoglycemia.
When your glucose falls rapidly, you are more likely to feel hungry and compelled to eat again soon and likely eat more than you otherwise would. This situation can be avoided by dialling back your carbohydrate intake or avoiding foods and meals that spike the most. That said, although lowering your carbs can be helpful to stabilise your glucose into the healthy range, simply swapping energy from carbs for fat is unlikely to lose weight or achieve the glucose levels necessary to burn your body fat. In fact, it might prompt you to gain it.
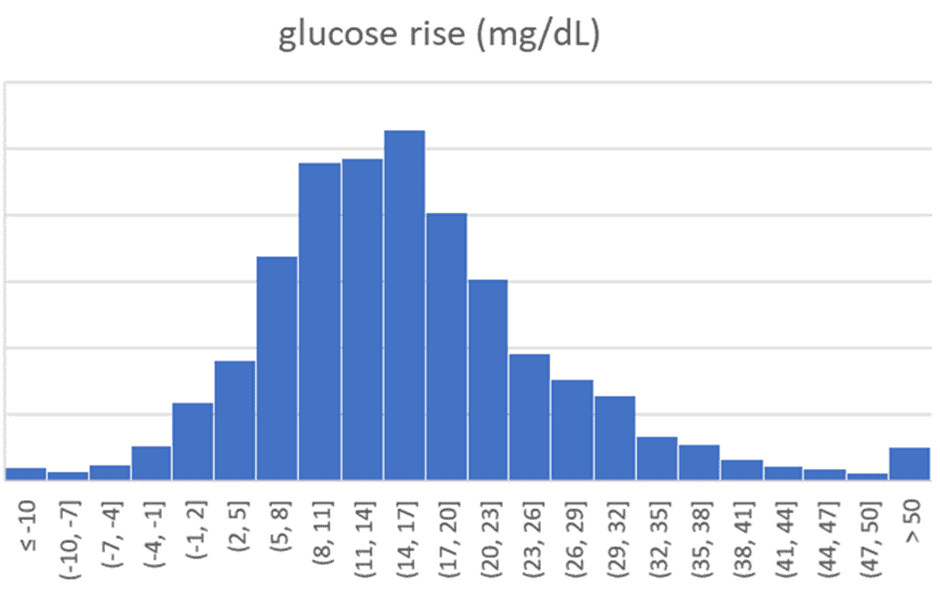
The chart below shows the distribution of the rise in glucose after people eat from 4,402 participants in our Data-Driven Fasting Challenges. Here, we can see an average increase of 16 mg/dL (0.9 mmol/L).
People towards the right of this chart whose blood glucose rises the most after meals will benefit from dialling back their carbs to achieve more stable glucose. However, we find that most people already see an acceptable rise in glucose after eating but often need to dial back their dietary fat. If people only focus on their blood glucose, this is not outwardly evident.
Our analysis of post-meal glucose values from 4,402 people in our Data-Driven Fasting Challenges shows no relationship between post-meal blood glucose and weight loss or healthier waking glucose!
How Can I Stabilise My Blood Sugar to Lose Weight?
A considerable amount of people have hopped on the ‘flat-line blood sugars = weight loss’ trend.
Many invest in expensive continuous glucose monitors (CGMs) to watch their glucose levels’ every turn and twist to see what throws them off their targeted flat-line trajectory. But sadly, many find that this method does not help them lose weight; instead, some actually gain!
Trying to understand every blip on your CGM and achieving flat-line blood glucose levels can quickly become overwhelming and hard to maintain. Many just end up swapping carbs for low-satiety, high-fat foods.
High blood sugar can contribute to many harmful conditions like cataracts, nerve damage, poor immunity, decreased wound healing, and systemic inflammation.
But stabilising your blood sugars and improving metabolic health is not simply about swapping carbs for fat. In our programs, people get much better results when prioritising foods and meals that contain more protein and fibre, which are positively correlated with increased satiety. Additionally, progressively dialling back energy from carbs and fat while prioritising protein and other nutrients allows them to burn body fat for fuel, lower their blood glucose, and improve their metabolic health.
Foods and meals with more fibre and protein tend to keep your glucose lower and stable. In contrast, hyper-palatable fat-and-carb combo foods keep our glucose and insulin elevated for longer and lead to fat gain.
Focusing on protein and fibre will help to increase your satiety and keep you full. It will also supply you with amino acids so you can maintain your precious metabolically active lean body mass, which fuels your metabolism and regulates glucose control.
For more on fibre, protein, and other nutrients that contribute to feelings of satiety, check out:
- How Much Protein Should I Eat to Lose Weight?
- Dietary Fibre: How Much Do You Need?
- The Cheat Codes for Optimal Nutrition, Satiety, and Health
Protein can also help lower blood glucose by stimulating a slight insulin response. Insulin, after all, helps clear glucose from the blood. Protein does not (often) elicit a glycemic response, so you are not adding to the problem.
Fat and carbs are energy sources; if you have adequate energy on your bum, thighs, and belly, you don’t need more of it in your diet! In contrast, a higher protein % is the most critical parameter for satiety. It also ensures you get the nutrients needed to preserve your lean mass while losing weight.
So, preserving your metabolically active lean muscle mass with protein will not only keep your metabolism fuelled, but it will also provide you with the nutrients you require to feel satiated, so you don’t overeat.’
Consuming more energy than your body needs will result in weight gain, regardless of how stable your blood glucose is.
By focusing on protein, fibre, and nutrients with less energy from carbs and fat, you will feel full and be able to manage your cravings while successfully eating at a calorie deficit. As you begin to lose weight, you will have less energy stored in your body. Thus, your blood glucose and insulin levels will decrease steadily over time!
Will Ketosis Help Me Lose Weight, and What Should Your Glucose Level Be for Ketosis?
Many people believe that a ‘ketogenic diet’ and simply cutting out all carbs will help them stabilise their blood glucose levels and lose weight automatically.
While minimising your carbs can help get you off the blood sugar rollercoaster, the ketones you measure in your blood must be coming from your body fat if you want to lose weight and not the extra fat from your diet.
Ketones are molecules produced by the liver from the metabolism of fatty acids. In the absence of carbs and excess protein, they can be used by the body for energy to fuel organs like the brain. When your glucose levels are low, your body will start breaking down body or dietary fat when glucose levels get too low, thus producing ketones.
While keto has been popular in recent years, we’ve found that your blood glucose before you eat is more helpful to guide your progress. As you lower your pre-meal glucose, you’ll have plenty of ketones in your blood from using stored body fat.
It’s important to note that ketosis is not a one-size-fits-all state, and the degree of ketosis you get into can vary from person to person depending on factors such as diet, exercise, and overall health. Additionally, greater ketone production does not necessarily equate to more fat-burning, especially if the ketones are coming from the extra fat in your diet.
Hence, higher ketone levels do not necessarily guarantee weight loss. Ketosis occurs when the body is forced to break down fat for energy vs carbs, and it can happen when someone is in a caloric deficit and burning body fat for fuel or when they’re eating a ton of dietary fat and not much carbs or protein.
For more on ketosis and how to get into it, check out:
- Keto Lie #1: ‘Optimal Ketosis’ Is a Goal, and More Ketones Are Better. The Lie that Started the Keto Movement, and
- Keto Lie #2: You Have to Be ‘in Ketosis’ to Burn Fat.
Does Your Body Burn Fat When Your Blood Sugar Is Low?
When your blood glucose is low, indicative of reaching the optimal blood sugar level for fat burning, the amount of energy flowing through your system is depleted. Thus, you will begin to tap into your body fat stores for fuel once your glucose lowers. However, there is no single glucose value that aligns with fat burning for everyone. The key is to reduce your glucose before you eat and continue to chase a lower average pre-meal value.
In our Data-Driven Fasting Challenges, we guide people to identify their initial pre-meal blood glucose ‘trigger’ (i.e., Your Personalised Trigger) based on the average pre-meal glucose over three days of baselining training. From there, your goal is to wait until their glucose returns below their personalised trigger before eating.
When your blood glucose reaches Your Personal Trigger, you have used up the excess energy buzzing throughout your system. However, when your glucose gets below your trigger, you start to tap into your stored energy, including your unwanted body fat.
You don’t have to wait a ridiculous amount of time to eat again, as many do with extended fasting, alternate-day fasting, OMAD, or other popular fasting trends. Unfortunately, these approaches can lead to very low blood glucose levels that align with extreme hunger and rebound bingeing on less-optimal food choices when they allow themselves to eat again.
Instead, with Data-Driven Fasting, you eat when you are hungry, and your blood glucose is just below Your Personalised Trigger.
The chart below shows the distribution of a quarter of a million premeal blood glucose from people in our Data-Driven Fasting Challenges. The average premeal glucose value is 82 mg/dL (4.6 mmol/L). However, as you can see, there is a wide range.
If you have pre-diabetes or Type-2 Diabetes, your premeal glucose will be much higher than that of someone who is metabolically healthy. So, hopefully, you can see why it’s critical to have a personalised target and why there is no one-size-fits-all number.
What Should Your Glucose Level Be for Weight Loss?
To begin using your blood glucose levels to lose weight, you can use a regular old run-of-the-mill blood glucose meter as a fuel gauge to determine Your Personalised Trigger to find your optimal blood sugar level for fat burning.
Your personalised trigger is the average of your premeal glucose over three days when you’re eating normally. You can use the Data-Driven Fasting app to calculate your trigger now.
From there, you must wait until you are hungry and your blood glucose levels fall below your trigger to eat again. As you are successful, the DDF app progressively lowers your premeal trigger, so you continue to lose weight without pushing it so hard you end up in a rebound binge.
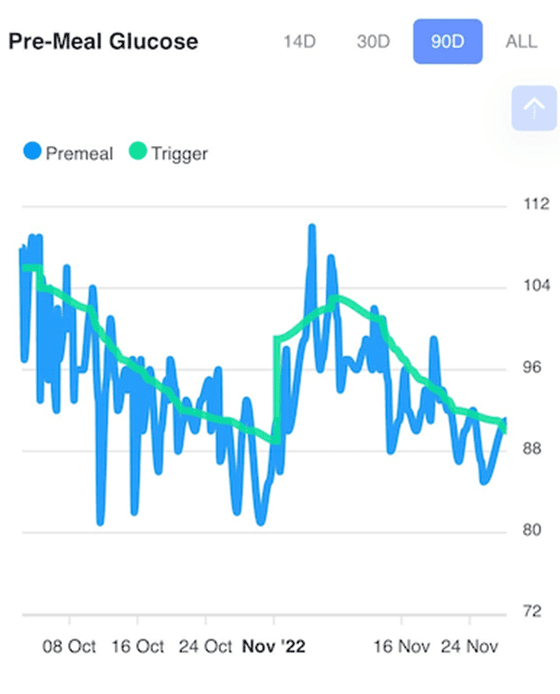
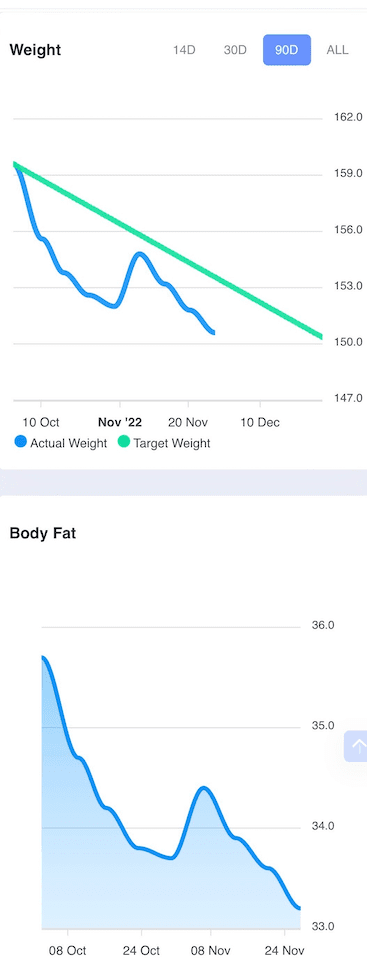
The images below show how this has worked for one of our participants, June. You can see her premeal glucose trigger progressively lowered through her first round of the DDF challenge. After that, she took a break and restarted baselining again to chase a lower trigger.
But over two rounds of the Data-Driven Fasting Challenge, her weight and body fat continued to fall at a healthy rate.
It’s a simple approach that gamifies the process of learning when and what to eat and has helped thousands lose weight, lower their blood glucose and improve their metabolic health.
Will Lowering My Blood Sugar Help Me Lose Weight?
As we mentioned earlier, healthy people naturally have lower blood glucose readings; manipulating blood glucose readings into the healthy, normal range will not necessarily make you metabolically healthy.
Eating a lower-carb diet if you have some form of metabolic imbalance will likely help you stabilise your sugars and get off the blood glucose rollercoaster. As a result, you are less likely to succumb to excess hunger when your blood glucose bottoms out not long after eating.
Simply shooting for a low blood glucose level by abstaining from food will not necessarily yield weight loss. In fact, letting your blood glucose levels drop too low could prompt you to gain weight, as hypoglycemia often triggers uncontrollable hunger.
Additionally, eating a nutrient-dense diet low in added sugars and refined carbohydrates can help keep blood sugar levels in check, as can eating more nutrient-dense foods.
We walk our Optimisers through these adjustments in our Macros Masterclasses and Micros Masterclasses. Finally, regular exercise, adequate sleep, and stress management techniques can also help regulate blood sugar levels.
How Can I Stabilise Blood Sugars and Lose Weight?
As we have described, lowering blood sugars does not necessarily equate to weight loss.
However, you can use your blood glucose levels to validate your hunger and understand if it’s time for you to refuel. This threshold to refuel is known as Your Personal Trigger, and it’s an essential foundation of our four-week Data-Driven Fasting Challenges.
In each four-week challenge, you will spend time establishing your blood sugar baseline and learning how to wait to eat until your blood glucose falls below it. You will also learn how to determine which foods will allow you to eat again sooner and which keep your blood glucose elevated for too long.
Summary
- Healthy blood glucose levels are between 70-100 mg/dL after a fast or <140 mg/dL after a meal. While healthy people have blood glucose levels in this range, manipulating your blood glucose levels to these values does not ensure stellar metabolic health.
- A higher body weight coincides with higher blood glucose and insulin. Thus, decreasing body fat aligns with improved metabolic health and ensures healthier insulin and blood glucose levels over time.
- Although a lower-carb diet can be an excellent way to stabilise your sugars, it does not always guarantee weight loss. Simply swapping carbs for fat might not be a successful solution!
- Using your blood glucose as a fuel gauge, as we teach in our Data-Driven Fasting Challenges, is a helpful way to begin unloading extra energy that your system has stored on board and get back in touch with your healthy hunger skills. In just four weeks, you can lose a substantial amount of weight and learn when to refuel and what to refuel with.
More
- How To Use a Continuous Glucose monitor for weight loss (and why your CGM Could Be Making You Fat)
- Blood Glucose and Hunger: Decoding the Intimate Relationship
- Keto Lie #10: Stable Blood Sugars Will Lead to Fat Loss
- Data-Driven Fasting: How to Use Your Blood Glucose as a Fuel Gauge
- What are Normal, Healthy, Non-Diabetic Blood Sugar Levels?
- Stress and Cortisol: The Missing Piece to Your Weight Loss and Blood Sugar Puzzle
- Hunger Training… How to Use Your Glucometer as a Fuel Gauge to Train Your Appetite For Sustainable Weight Loss















Your posts are always so chockful with good information; I’m sure glad I got the unlimited membership, because I seem to find something new (and usually lots of somethings new!) in even the posts and materials I have read before. I hope I can move it from short-term to longterm memory during the next challenge. For now I’m just trying to get through all the resources! Thank you.
Thanks so much. Glad to hear you’re loving it all.