Many people still believe the primary role of insulin is to push energy into fat cells when you eat carbs. This flawed logic goes a bit like this:
eat carbs -> boost insulin –> get fat
But the reality is:
- in the fullness of time, all food elicits an insulin response to varying degrees,
- the insulin released after you eat is only a fraction of the insulin produced by your pancreas each day,
- your cells are always using glucose regardless of insulin,
- insulin’s primary role is to stop your body from disintegrating, and
- the bigger you are, the more insulin your pancreas needs to produce.
The most effective way to reduce your daily insulin requirements is to eat in a way that will increase satiety and will allow you to achieve (and maintain) healthy body fat levels.
To help you move beyond the over-simplified carbohydrate-insulin belief, this article will:
- give you a deeper understanding of how insulin works in your body, and
- show you how to reduce your insulin, blood glucose, and weight to healthy levels through improved food choices and optimised meal timing.
Eager to learn more about the actual role of this critical hormone in your body and how you can manipulate it to your advantage?
Then, let’s go!
- Does Insulin Make You Fat?
- What Would Happen If You Injected Too Much Insulin?
- Does Insulin ‘Push Glucose Into Cells’?
- The Primary Role of Insulin: To Hold Your Fat and Glucose in Storage
- What would happen if you had no insulin?
- The problem with short-acting insulin
- Learning To Think Like a Pancreas
- Basal > Bolus Insulin
- Insulin Toxicity vs Energy Toxicity
- Energy flux and Your Fat and Glucose Fuel Tanks
- What Happens To Insulin Between Meals?
- What Happens to Insulin When You Eat Carbohydrates?
- What Happens to Insulin When You Eat Fat?
- It’s The Area Under the Curve That Matters!
- How Can You Reduce Your Insulin Levels?
- So, What’s Left to Eat?
- More
Does Insulin Make You Fat?
Jason Fung says, ‘I can make you fat by giving you insulin‘.
This is true, but only if he followed you around and jabbed you all day with a needle full of insulin.
But this would be illegal, and anyone who did that would be locked up.
Fortunately, it wouldn’t happen for long.
What Would Happen If You Injected Too Much Insulin?
If you did happen to accidentally inject too much insulin:
- your blood sugars will plummet,
- you will feel super hungry, and
- you would eat anything and everything you could get your hands on NOW to bring your blood sugars back to normal levels!
No amount of conscious willpower would stand in the way of your raging survival instincts.
And yes, if you continue to inject more insulin than you need and continue to due to the hunger it creates, you will eventually get fat. However, this fact is 100% irrelevant for the 98.5% of us that have a functioning pancreas and can produce the insulin we need.
- Endogenous (produced from inside the body) and exogenous (supplied from outside the body) are different animals.
- Like everything in nature, your body is highly efficient – your pancreas only makes just enough insulin to respond precisely to the food you eat and your body fat levels.
- Insulin alone can’t magically store energy from food you don’t eat.
As you will see in this article, insulin due to the carbs (or even protein) you eat is not the primary driver of obesity.
Instead, the reverse is true: unless you are injecting insulin, obesity is the driver of high insulin levels.
Does Insulin ‘Push Glucose Into Cells’?
When my wife Monica was diagnosed with Type-1 Diabetes 35 years ago, she was taught that insulin is like a key that unlocks insulin receptors that work as cell doors to allow glucose into the cell. It can then be transformed and utilised as energy.
Our understanding of the role of insulin has come a long way since then. We now know that we can use energy in food via non-insulin-mediated glucose uptake (i.e., without insulin).
If your cells run low on fuel, the energy from your blood floats into the cells to be used. Glucose is translocated across the gradient from high glucose in your blood to lower glucose in your cells. So, if your cells are using energy, they essentially suck it in from the bloodstream.
GLUT1 is the insulin-independent glucose transporter that allows cells to use glucose without insulin. A little bit of exercise goes a long way to increasing GLUT1 activity! Meanwhile, GLUT4 is the insulin-dependent glucose transporter that helps glucose enter cells.
The 2011 study by Krakoff et al. titled Assessment of Non-insulin Mediated Glucose Uptake: Association with Body Fat and Glycemic Status showed that 83% of glucose uptake occurs through non-insulin mediated mechanisms like GLUT1 glucose transport. On average, your body clears 1.6 mg/kg of glucose per minute from your bloodstream without using any insulin. That’s more than 160 g of glucose (or carbs) per day for the ‘average’ 70 kg man. So, if you’re on a lower-carb diet, all the glucose you eat could be used without insulin!
The bottom line is that insulin isn’t required to “push” glucose into the cells in the same manner as Japanese subway workers pushing more people onto the train. This only happens when you inject way more insulin than you need or build up excessive energy in your blood that your cells can’t use.
Although exogenous injected insulin is often used to manage dangerously high blood glucose levels as in the management of Type-2 Diabetes, insulin’s anabolic role of ‘pushing’ energy into cells should still be seen as an emergency function when glucose levels are elevated above optimal levels.
The Primary Role of Insulin: To Hold Your Fat and Glucose in Storage
Rather than seeing insulin as a pusher, it’s much more helpful to see insulin as an anti-catabolic hormone that stops your body from breaking itself down (or falling apart).
Without insulin, the fat and glycogen in your liver and muscles would flow freely into your bloodstream. Once your stored glucose was used up, your body would then resort to using other more valuable tissues for fuel, like your muscles and organs!
Insulin is the signal sent from your pancreas to your liver to regulate the flow of just enough energy into your bloodstream to meet your current energy needs.
You can think of the stored fuel in your body like a water tank: the more fat and glucose you have in storage, the higher the pressure is to push the stored energy out of the liver. You can think of insulin as the signal that regulates the tap. With no insulin to turn off the tap, all your stored energy would gush out. Conversely, if you have a lot of energy in storage, you need to go to greater lengths to turn off the tap to ensure it doesn’t leak.
What would happen if you had no insulin?
The photo below shows an extreme example of what happens when people with Type-1 Diabetes can’t produce enough insulin – they lose weight quickly and waste away (as shown in the photo on the left). However, they can quickly regain weight once they get enough insulin. The photo on the right is the same child after taking insulin.
In another example, a bit closer to home, my fifteen-year-old son was recently diagnosed with Type 1 Diabetes. The photo on the left shows him in hospital with a blood sugar of 23 mmol/L (or 420 mg/dL) and an HbA1c of 14.5%. The photo on the right shows him five weeks later doing some father-son axe throwing.
Fortunately, we caught it early and knew what to do when we randomly tested his blood sugars and found them sky-high. At the time, he was eating a LOT (like 4000 – 5000 calories per day) of food but still very lean. We thought it was because he was doing a lot of sport and spending a ton of time in the gym.
However, after five weeks on about 50 units of long-acting insulin per day, he has gained about 5 kg and increased his deadlift by 40 kg, pulling 195kg or 430 lbs in his first powerlifting competition! The extra exogenous insulin helped him stop wasting all the energy and stopped his muscles from breaking down. Thankfully for our food budget, he’s also eating a lot less!
The problem with short-acting insulin
If you’re injecting insulin, it’s crucial to get just enough — but not too much—short-acting insulin. As highlighted by the image below (that’s been shared 295k times on Facebook!), injecting insulin can be dangerous.
Type 1 Diabetes guru Dr Richard Bernstein talks about the Law of Small Numbers whereby large inputs of fast-acting carbohydrates and large doses of short-acting insulin lead to large errors that are hard to manage.
The graphic below shows the calculations that someone dosing for insulin relies on to calculate their blood sugars. While this is the best available, there will always be errors in these insulin dosing calculations. The simplest way to reduce the magnitude of the errors is to reduce the blood starting blood sugar and the amount of fast-acting carbohydrates.
These errors put someone taking exogenous insulin on the blood sugar rollercoaster, which makes them feel awful as their blood sugars swing wildly.
This really becomes problematic when their blood sugars drop below what feels normal for them, and they become super hungry. The injected insulin causes their blood sugars to drop below normal, they become hungry, and they end up overeating.
But, as you’ll learn in the next section if you’re not injecting insulin, it’s not the insulin produced by the pancreas that is causing you to gain weight.
Learning To Think Like a Pancreas
People often believe they struggle to lose weight because they are ‘insulin resistant’. However, the reverse is true – their fat stores are packed full and ready to burst as soon as they learn to eat in a way that provides greater satiety!
I’m fascinated by my wife Monica’s continuous glucose meter, which includes a closed-loop insulin pump system (Android APS). I see a live version of Monica’s blood sugar dashboard like the screenshot below on my phone and computer most of the day.
Because it’s a matter of life and death, I like to see that she’s doing OK. So, I review the data twice a week and fine-tune her basal insulin profile to keep her blood sugars as close as possible to optimal levels.
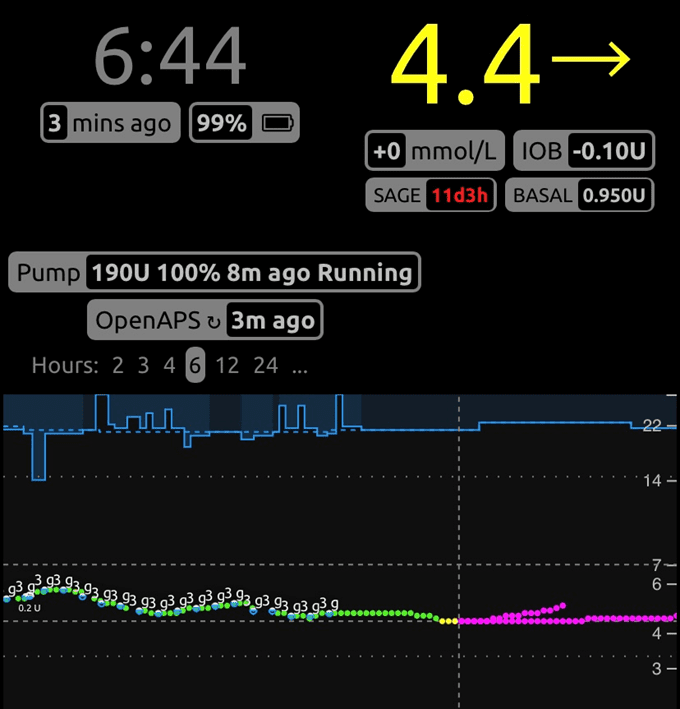
In this image from NighScout, the “4.4” number is her current blood sugar (in mmol/L). The little numbers on the line to the left shows an extended bolus insulin dose for lunch – the algorithm drips insulin slowly over 5 hours to maintain glucose in a healthy range for low-carb meals.
The coolest thing is the basal insulin chart in the middle that resembles a blue “icicle”. This displays the action of the pump, which is slowly dripping between 0.75 and 0.9 units of insulin per hour whether she eats or not. The algorithm reassesses her current blood sugar and how much active insulin she has in her bloodstream every five minutes. It then adjusts her basal insulin rate to ensure her blood sugar will be in the target range five to six hours from now.
The pink lines on the right are the projected blood sugars for the next five hours. The algorithm always ensures that her blood sugars won’t go too low, even if the system fails. If her blood sugars are projected to go below 4.0 mmol/L, it will temporarily dial the basal insulin back. If it forecasts that it will rise above 6.0 mmol/L, it will add more basal insulin.
Using this closed-loop insulin pump system has been incredibly helpful for Monica to dial in her insulin management and control her Type-1 Diabetes. When Monica started using an insulin pump, she used more than 60 units a day and had an HbA1c of 11%. Now, she’s using less than 30 units per day and has a non-diabetic HbA1c in the low 5s despite not producing any insulin herself.
This experience has also helped me understand how the rest of us with fully functioning pancreas can reduce our insulin requirements, achieve better blood glucose control and lower body fat levels. It has also helped me cut through the confusion and conflicting advice in the nutrition space.
I have tried to learn to think like a pancreas by continually watching the algorithm to understand the various factors that affect blood sugars and insulin.
In the rest of this article, I’ll share some of my insights for those of you who have fully functioning pancreases.
Basal > Bolus Insulin
One of the main takeaways I want to highlight from this little ‘show and tell’ is the amount of basal insulin required to stop Monica’s stored glucose, fat, and muscles from being broken down and dumped into her bloodstream vs the amount related to the food she eats.
The snip below is Monica’s average daily dose over the past month, showing that 90% of her daily insulin is basal insulin. Remember: basal insulin is the insulin that is required to keep her body from disintegrating. Only 10% of her daily insulin is related to her food!
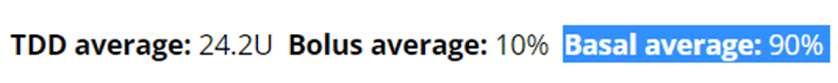
We see a similar pattern in the insulin pump data from other people with Type-1 Diabetes. While their bolus insulin may be higher if they eat more carbohydrates, most of their requirement is still basal insulin to hold their fat in storage.
Her basal insulin was higher when Monica was heavier than she is now. Monica’s body weight is the main constant influencing her daily insulin demand! She always has the lowest total demand when she is losing weight.
The photo on the right is at the end of our first Masterclass when we both prioritised higher satiety meals. As a result, we both lost a ton of weight, and her insulin was the lowest it had EVER been.
The chart below shows Moni’s daily insulin dose over the past 13 years. On the left, you can see where we started getting into paleo and lower-carb – her daily insulin dropped from 50 to 30 units per day. But then, during the Masterclass in February 2019, her insulin requirements dropped as low as 12 units per day, focusing on nutrient-dense high, satiety meals.
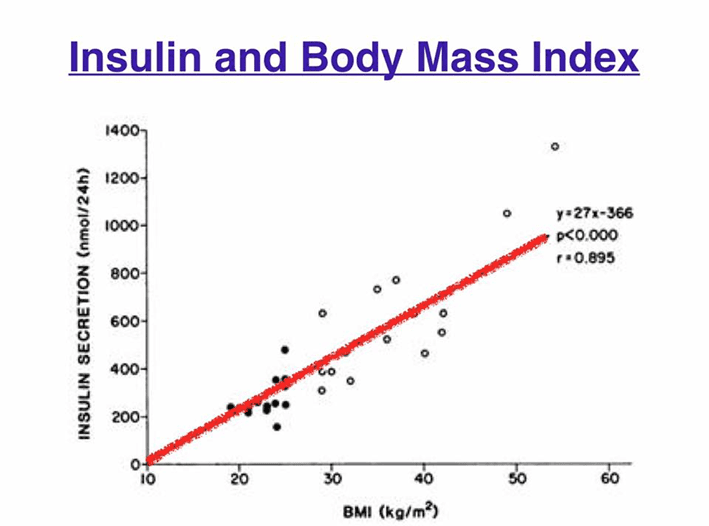
This is precisely the same for you, regardless of whether you have diabetes or are injecting insulin! The chart below shows the relationship between BMI vs daily insulin showing your pancreas needs to produce more basal insulin to hold all that stored energy in storage as you become bigger.
It’s not the muffin that you just ate that is primarily causing your elevated insulin levels, but rather the muffin top of fat around your belly from the food you ate a year ago that is raising your insulin levels.
While it’s helpful to maintain your blood sugars in a healthy range to prevent blood sugar crashes that drive your appetite, the most important thing you can do to lower your insulin is to find a way of eating that allows you to achieve and maintain a healthy body weight.
To achieve this, your goal should not be flat-line blood sugars achieved by avoiding carbs and even protein and eating ‘fat to satiety’. Instead, you must find the right balance of protein-rich, nutrient-dense foods and energy supplied from fat and carbs that maintain satiety and enable you to use stored energy.
Insulin Toxicity vs Energy Toxicity
Many people lately have been talking a lot about ‘insulin toxicity’ as if it is what we should fear the most. However, the reality is that high insulin is simply another symptom of being overweight. The root cause of insulin toxicity is energy toxicity. The only way to meaningfully manage it is to lose fat and build more muscle.
So rather than:
eat more carbohydrates -> make more insulin -> get fatter
what appears to be driving obesity is:
low satiety, nutrient-poor foods -> increased cravings and appetite -> increased energy intake -> fat storage -> increased daily insulin
The real solution to managing Type-2 Diabetes, blood sugar, insulin levels and avoiding the myriad complications of metabolic syndrome is:
Consuming high-satiety nutrient-dense foods and meals -> decreased cravings and appetite -> decreased energy intake -> fat loss -> optimised insulin levels
In the final part of this article, I’ll share some insights to help you from my research on learning to think like a pancreas and watching Monica’s closed-loop pump system.
Energy flux and Your Fat and Glucose Fuel Tanks
Your body is a dynamic system similar to a dual-fuelled engine that runs predominantly on glucose and fat.
In an emergency, you can use alcohol, ketones, and protein. However, your body uses the fat and glucose from your food most of the time.
Most of the time, your body is extremely capable of regulating just enough fuel in your bloodstream. Your body also likes to maintain a healthy reserve of energy in its two fuel tanks:
- your adipose tissue (fat stores), and
- liver for reserving glycogen (the stored form of glucose).
These fuel tanks are depicted diagrammatically in the image below.
Energy in the form of glucose and fat is constantly flowing into your bloodstream and being utilised as energy by your body.
You only have about five grams of glucose in your bloodstream at any time, equating to roughly 20 calories. This would only last you about 15 minutes if your liver didn’t manage the constant flow of fuel into your bloodstream so precisely!
But, your body only wants to have just enough glucose and fat in your blood at any one time to fuel your immediate activities like thinking, breathing, walking, running or exercise. Too much glucose in your bloodstream leads to a range of complications, so it’s tightly regulated.
What Happens To Insulin Between Meals?
When you don’t eat, your pancreas produces a little less insulin to let more energy flow into your blood. Just like Monica’s closed-loop insulin pump, your basal insulin is slightly decreased for more energy to flow out of storage.
The reduction in insulin signals your liver to ‘open the tap’ a little more and release energy from stored liver glycogen and adipose tissue into your bloodstream.
Later, as your liver starts to get depleted of glycogen and your blood sugars drop, ghrelin increases to prompt feelings of hunger so that you seek out food. When you eat, energy from fat and carbs gets stored in your liver and adipose tissue. The process then starts all over again!
What Happens to Insulin When You Eat Carbohydrates?
Now, let’s look at what happens when you eat some carbs. Your body has limited space to store carbohydrates in your liver and muscles, and your body wants to keep a tightly regulated glucose level in the bloodstream. In other words, not too little or too much.
When you dump an excessive load of carbs into your body from that bread, apple, or potato you just ate, your pancreas abruptly raises insulin to slow the stored glucose from your liver until the glucose in your blood is used up. So, the more carbs you eat, the more insulin is required to hold back your stored energy.
Rather than thinking your body is pushing glucose into your cells, it’s more helpful to think of it as holding back stored energy until the carbs you just ate are used up.
While the insulin response to carbs is sharp and fast, it usually clears quickly, and your glucose and insulin return to baseline in two to three hours. Once glucose is cleared from your bloodstream, insulin starts to drop, and you return to releasing stored energy.
The chart below shows the data from food insulin index testing.
- Pure glucose (black line) has a significant insulin response, but it returns to baseline quickly.
- In contrast, foods like milk (aqua line) that combine fat and carbs have a flatter but more extended insulin response.
What Happens to Insulin When You Eat Fat?
The reason we don’t see such an abrupt insulin response to fat is two-fold.
- On the one hand, fat takes longer to digest and metabolise. You will still see an insulin response to pure fat, although it will be over a much more extended period.
- On the other hand, your body doesn’t respond heavy-handedly with insulin to fat because, unlike glucose, there is simply plenty of room to store it! Your body doesn’t need to halt the release of stored energy to burn it off. Dietary fat simply gets welcomed aboard with open arms and added to your fat stores to be used later.
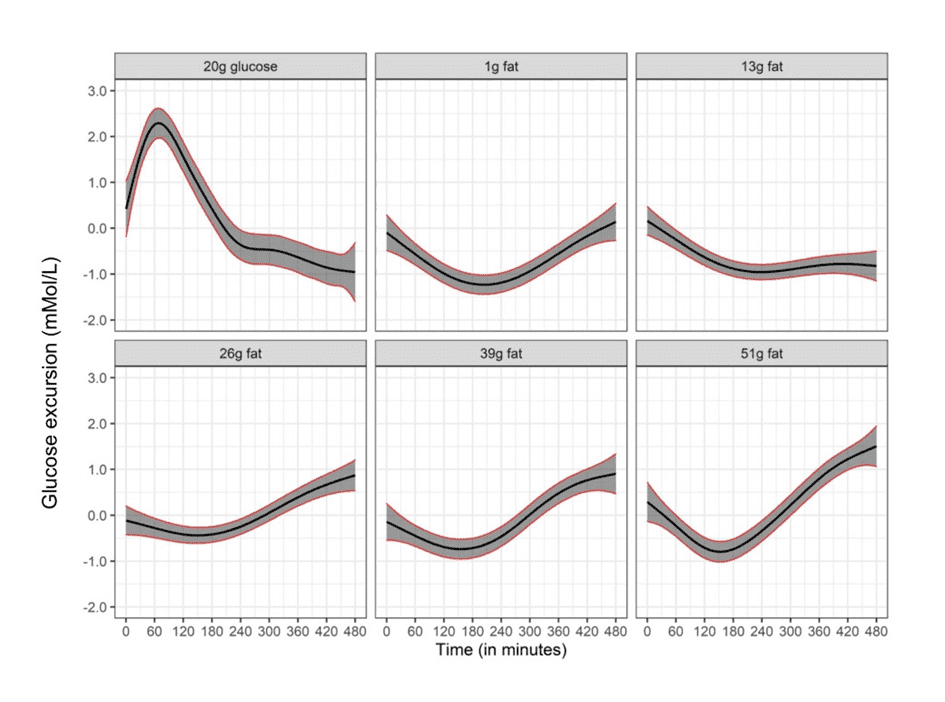
A recent study in people with Type 1 Diabetes who didn’t take insulin showed that, while dietary glucose raises blood sugar in the first three hours or so, dietary fat causes a significant rise after three hours.
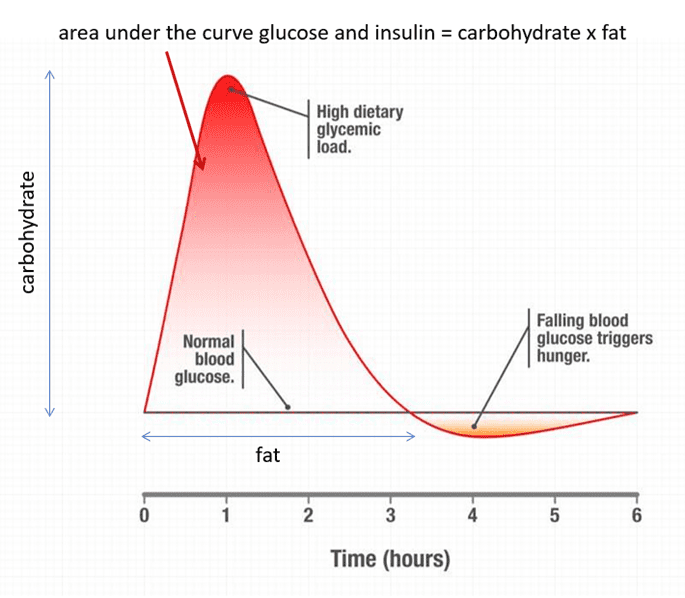
It’s The Area Under the Curve That Matters!
Now I want to show you how to stabilise your blood sugars and reduce insulin levels across the day.
The diagram below shows how your blood glucose responds to the food you eat.
The amount your glucose rises is proportional to how many carbohydrates you eat. So, if your blood sugar rises more than 30 mg/dL (1.6 mmol/L) after eating, you have probably overfilled your glucose fuel tanks in your liver and muscles. So next time, you may want to consider eating less of the food you just ate.
What goes up must come down! When your blood sugar comes crashing below what is normal for you, you’ll feel hungry. If your glucose goes way below average for you, you’re more likely to make less than optimal food choices.
In contrast, the length of time your blood sugars will remain elevated after eating fatty meals is much longer, although they don’t cause a significant spike. As a result, your blood sugars will stay above baseline for much longer.
The worst combination of foods you can eat is fat and carbs together. This fattening combination is the basic formula for most processed foods, like croissants, pizza, or creamy pasta. These foods will raise your blood glucose and keep them elevated for longer. You can also eat a lot more of these foods because you can fill both fuel tanks simultaneously. The overall area under the curve is, therefore, much larger. Because glucose must be used first before fat due to oxidative priority, you’ll have to wait a long time before using the dietary fat and even longer to burn your excess stored body fat.
How Can You Reduce Your Insulin Levels?
So, what’s the solution?
How do you tame your insulin and blood glucose?
Now that you understand the problem, the solution is relatively simple: you do the reverse.
- A little less carbohydrate will reduce the magnitude of your glucose spike.
- Likewise, a little less fat will help your blood sugars return to your baseline more quickly.
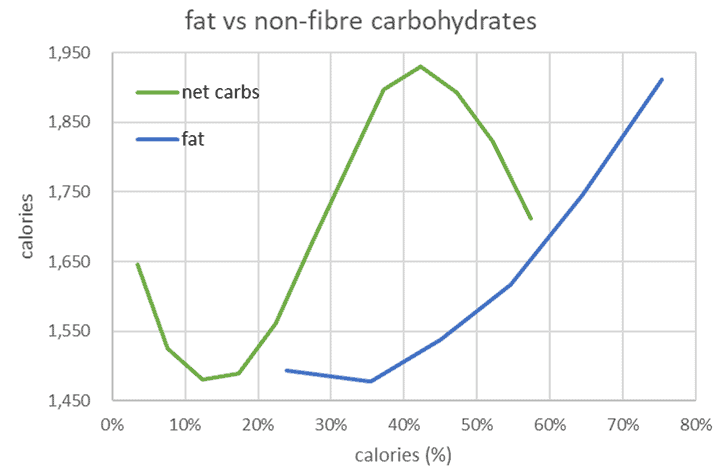
As shown in the chart below from our satiety analysis, eating less energy from carbohydrates and fat corresponds to eating less.
While some people benefit from lower-carb and others benefit from lower-fat diets, the reality is that reducing either carbs or fat will help you eat less.
You can dial back either fat or carbs or even both to lose weight. But the key here is to do it progressively to ensure it’s sustainable. Unfortunately, we found many people tend to swing from one extreme to the other and end up ‘falling off the wagon’ in a rebound binge because their body needs some energy.
That’s why we designed the Macros Masterclass – to guide people to understand their current diet and progressively tweak their macros just enough to ensure sustained progress (i.e., between 05 and 1% weight loss per week).
If you want to lose body fat, you must wait a little longer to permit your blood glucose to drop below your average premeal glucose. For those who don’t like tracking their food, we use blood glucose to guide when people need to refuel in our Data-Driven Fasting Challenges.
So, What’s Left to Eat?
So, what’s left to eat if you dial back both glucose and fat?
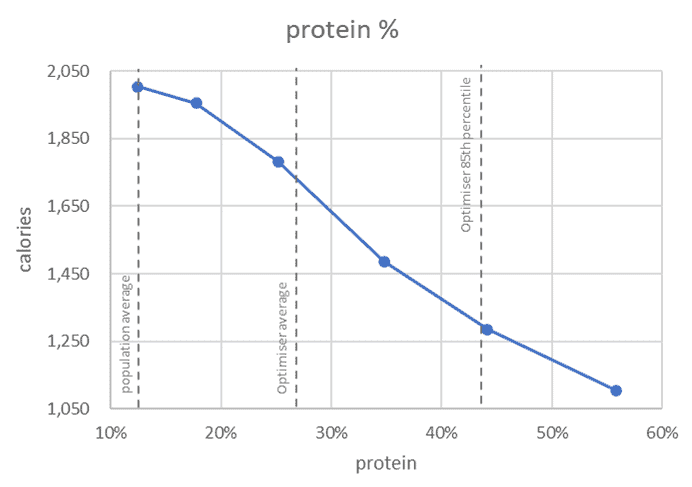
The secret is to prioritise foods and meals that contain protein, fibre, minerals, and vitamins with less energy from fat and non-fibre carbohydrate.
Of all the micronutrients and macronutrients, protein % has the biggest impact on satiety. These will give your body what it needs with less excess energy to smash your appetite. As a result, you will be more satisfied while taking in fewer calories.
However, if you’re willing to do a little bit of work to dial in all of the micronutrients, we find in our Micros Masterclass that people get even better results when they improve their Diet Quality Score.