Embark on an illustrative expedition to unravel the mysteries of metabolism, the intricate system that powers every movement, thought, and heartbeat.
Through a pair of enlightening infographics, discover the complex dance between food, digestion, and energy conversion. Witness firsthand how a healthy metabolic system stands in stark contrast to one beleaguered by energy toxicity.
Delve deeper into the subtle nuances and vital components of metabolism, offering a visual narrative that’s both enlightening and captivating. With each section, move closer to understanding the core of metabolic flexibility versus energy toxicity, setting the stage for an informed quest toward nutritional and metabolic nirvana.
Background
With 82,000 followers on Twitter, I know there’s a long line… but I think I must be Dr Ted Naiman’s #1 fan!
Many of my articles, like this one on the Personal Fat Threshold Model of Insulin Resistance, Diabetes, and Obesity vs. the Carbohydrate Insulin Model, are just extended captions to his pithy memes about nutrition and metabolism.
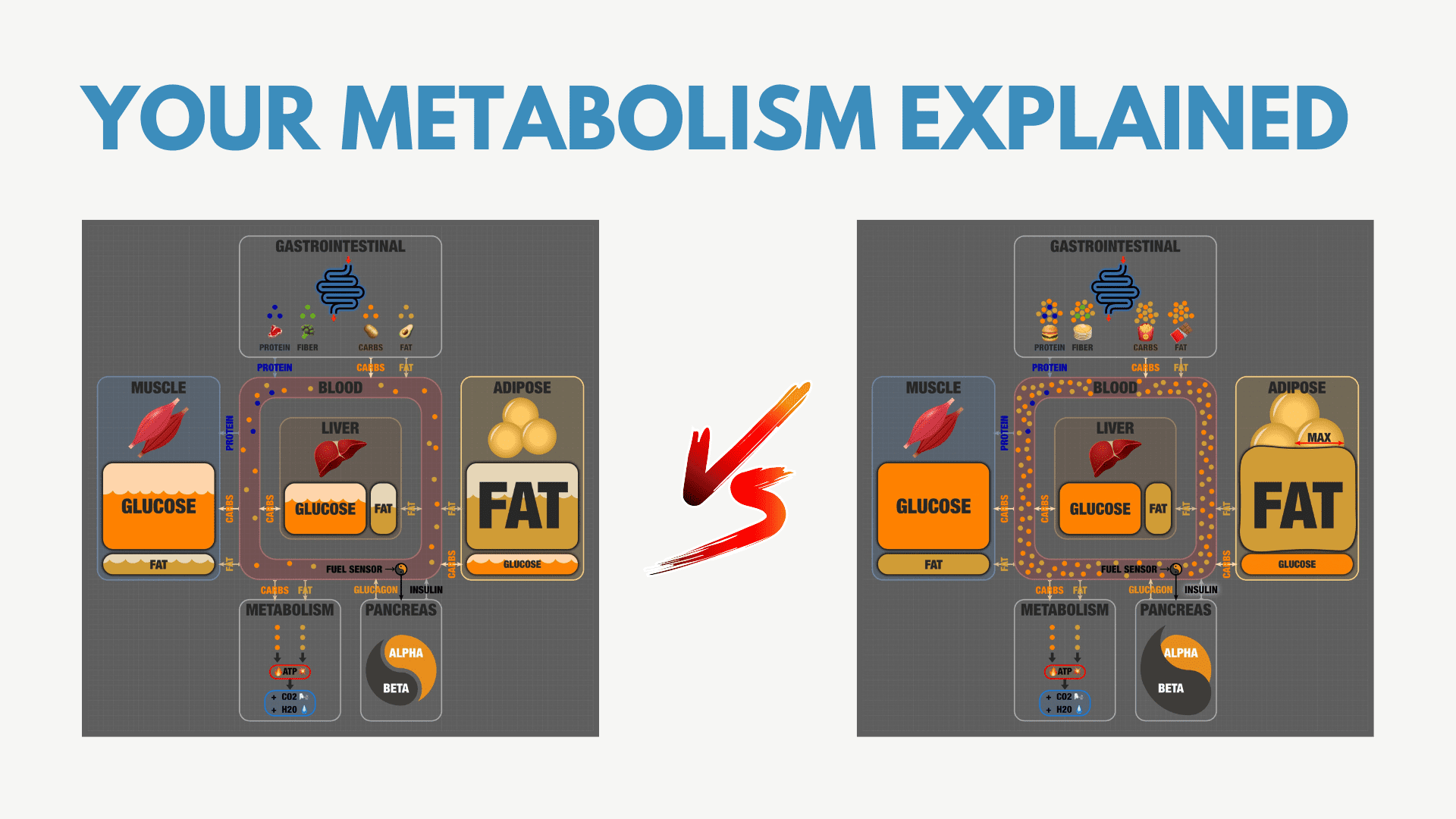
Ted recently shared a set of super cool infographics that show what components of human metabolism differ between someone who is metabolically healthy and someone who is suffering from energy toxicity.
You can see the animated gif version here.
There are many important concepts to unpack here, and I had a few queries from some of our Optimisers wanting to understand more.
So, I thought it would be worth putting an article together to unpack and compare metabolic flexibility vs. energy toxicity.
The following sections explain how each crucial component of human metabolism functions with the others.
In the end, I’ll share some of the most valuable strategies you can use to achieve nutritional and metabolic nirvana.
Food and Digestion
It all starts in the gut—or at least with what we put in our mouths!
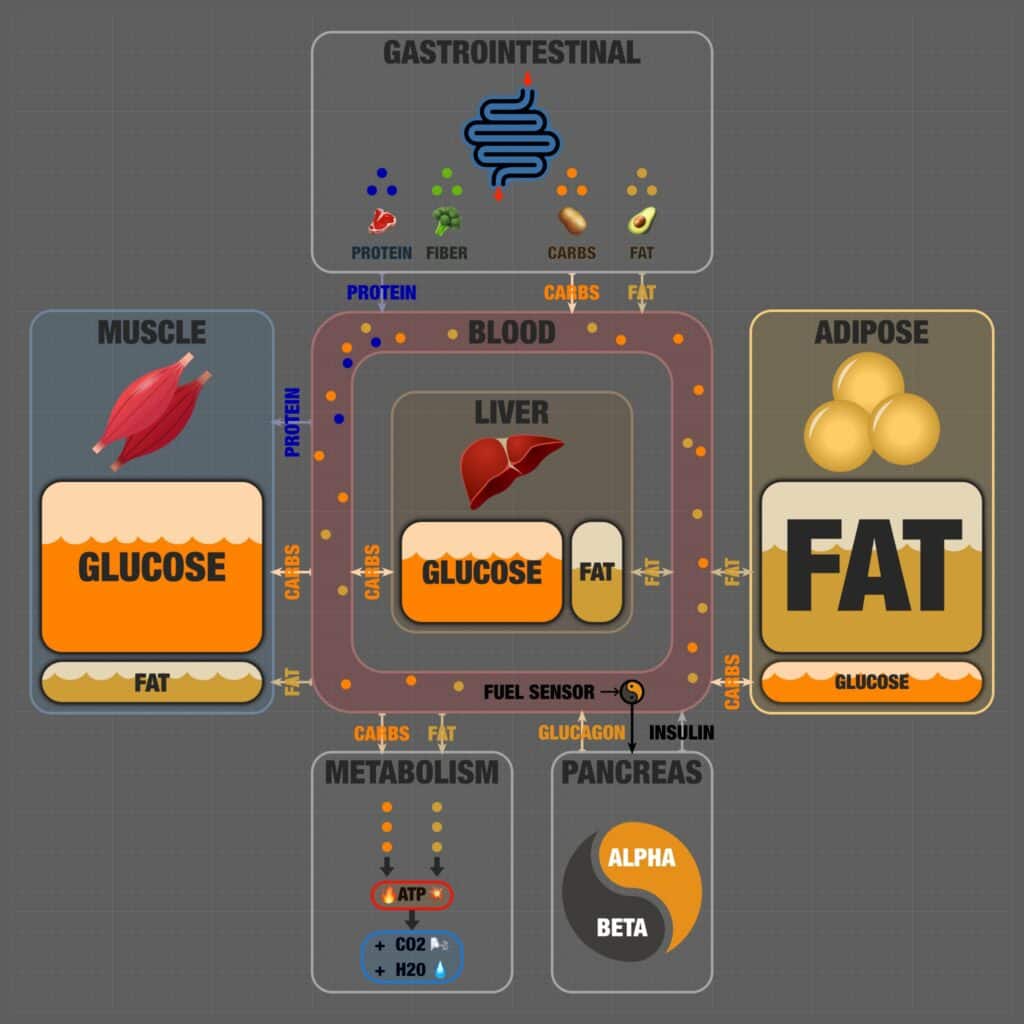
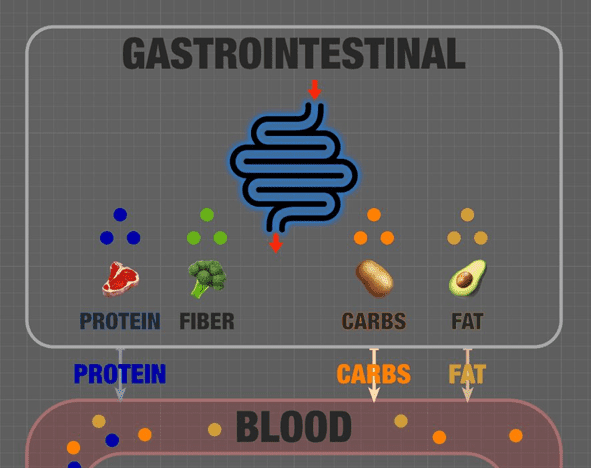
As the snip below shows, protein, fibre, carbs and fat are the main components that make up the food you eat.
First off, we have fibre, which is represented as green dots. We lack the enzyme that allows us to break down fibre (cellulase) into energy your body can use. Instead, fibre feeds your gut bacteria, binds to toxins in the GI tract, and bulks up your stools.
Although it’s helpful to ‘keep things moving’, fibre is not essential, so we don’t have a target intake. However, more fibrous foods can be beneficial as they’re harder to overeat. It’s ideal if your carbs are more fibrous. Fibrous foods also contain more essential nutrients like manganese, copper, iron, potassium, calcium, and vitamin C.
Next, we have protein shown as blue dots. During digestion, the amino acids in protein are extracted from your food and flow directly to your muscles by blood. This is shown in the top left corner of the infographic’s ‘blood’ section.
A little labile protein floats around your blood to refresh your muscles and organs. Aside from muscle and organ repair, we need protein to make enzymes and DNA, detoxify, and synthesise nearly every substance in our body. Higher-protein foods contain other essential micronutrients like niacin, zinc, selenium, calcium, sodium, and potassium.
As Ted and I have discussed before, foods and meals with a higher percentage of total energy from protein (a higher protein percentage, or protein %) tend to be more satiating and harder to overeat. We have strong cravings for protein.
But our appetite settles once we get enough to satisfy our bodies’ needs. Thus, prioritising protein ensures we don’t overconsume energy from carbs and fat while your body searches to get the protein it requires.
Finally, we have carbs (orange dots) and fat (brown dots), our body’s primary fuel sources. Carbs and fat flow into the bloodstream as glucose and fatty acids.
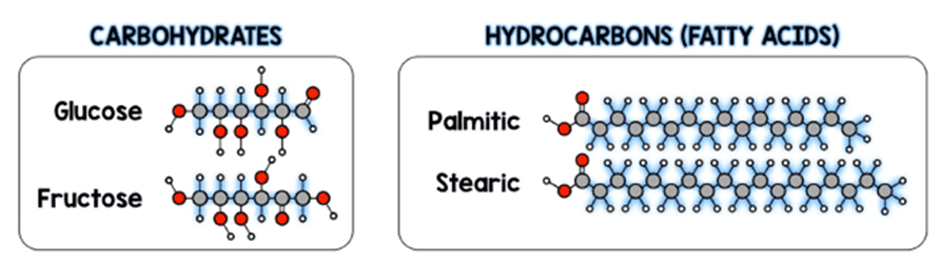
Carbohydrates and fat contain energy as carbon-carbon bonds. During fatty acid oxidation and glycolysis, they are broken down and used to produce energy as ATP.
Carbs are an explosive, volatile fuel source. From what we know about oxidative priority, your body must use carbs up first because it can’t store much of them. This makes them great for explosive activity. Carbohydrates are stored in your body as glycogen, which is one molecule of glucose and three molecules of water.
At nine calories per gram, fat is the most energy-dense macronutrient. Fat is a much more stable fuel source and great for storage and everyday use. But it’s easy to store because the body doesn’t have to produce much insulin or exert much energy to turn fat into usable fuel.
Fat is also last in line to be burned for energy per the oxidative hierarchy. So, if you’re drinking and eating a lot of alcohol, carbs, and protein on top of your fat, you’ll likely store the dietary fat you don’t use.
Our digestive system and appetite work optimally when we only consume one thing at a time. Consuming foods in their natural, whole form also makes it difficult to overeat. Over time, we humans have ingeniously figured out that combining fats and carbs makes food much tastier, and we can eat a lot more of it—especially when we don’t add much protein.
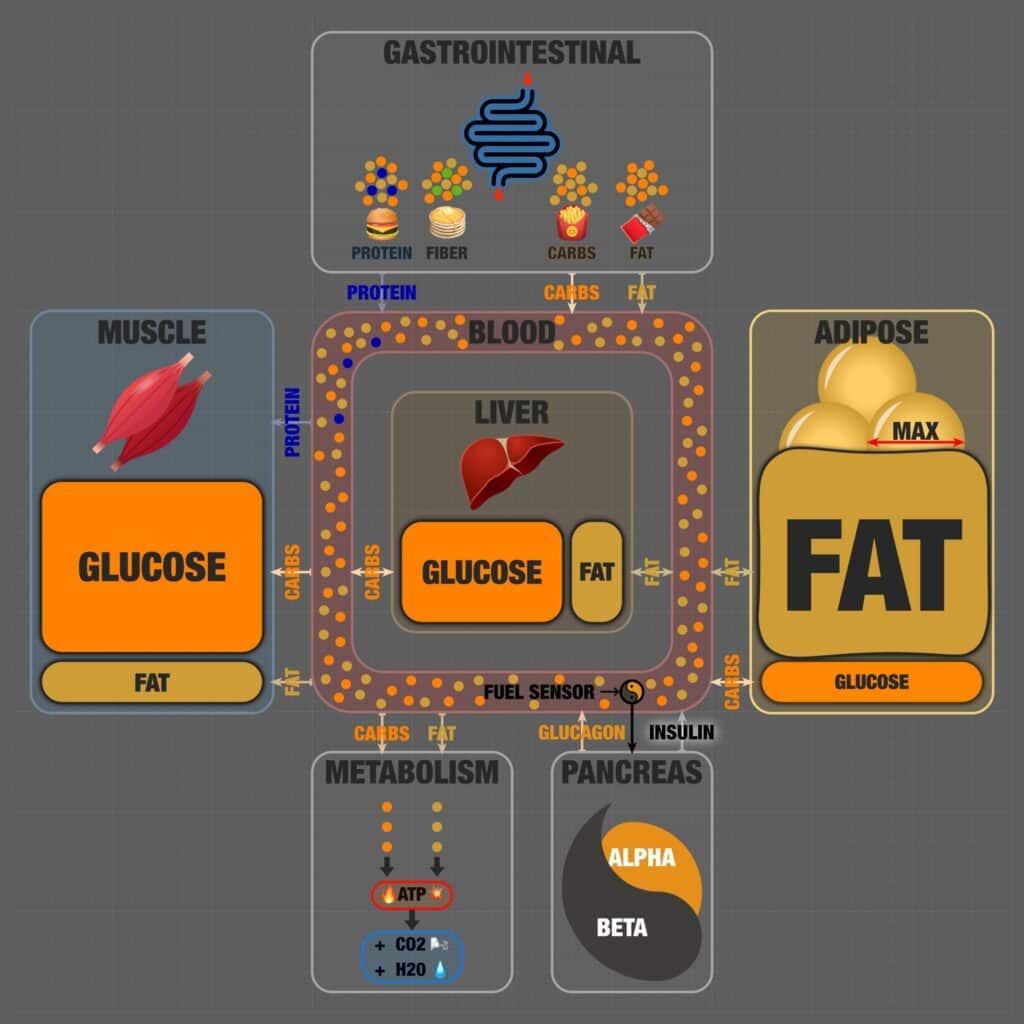
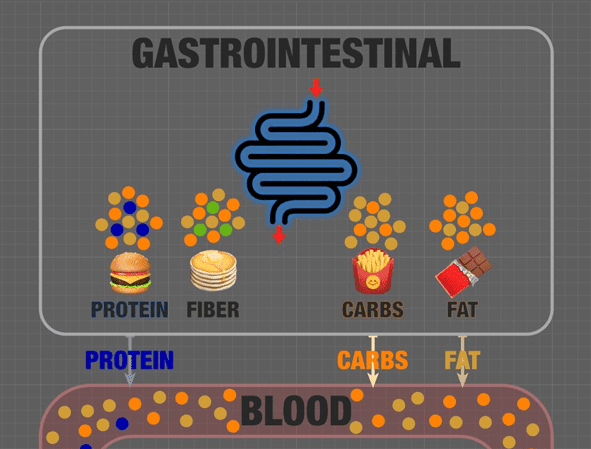
In the second ‘processed’ version of the infographic, we see the macronutrients represented as hyper-palatable industrialised ‘pseudo’ foods. Here, milk chocolate is a combination of fat and carbs (sugar added to the chocolate).
French fries are a similar mixture, with the potatoes providing carbs and industrial seed oils accounting for the fat. There is a little fibre and protein, but refined starches dilute it in the pancakes, hamburger bun, and French fries.
In nature, fat-and-carb combo foods were rare except in autumn, when we needed to fatten up for winter. Our satiety analysis shows that fat and carbs are minimally satiating without protein. However, each elicits a sizable dopamine response, which stimulates our reward system and tells us to eat MORE of them.
But modern low-protein, fat-and-carb combo foods drive a supra-additive dopamine response that leads us to overeat and feel ‘addicted’ to these foods beyond what we can control. This unique combination tells our bodies that winter is coming and that we need to get fat to survive NOW!
But in our modern world, winter never comes. Overconsuming low-protein, low-fibre, fat-and-carb combo bombs have us stuck in perpetual autumn. Ultimately, we overeat and inherently overfill our fat and carb fuel tanks. Over time, our bloodstream becomes overloaded with energy from fat and glucose, which you see as high blood sugars, cholesterol, and triglycerides.
Storage and Circulation
As shown in this following snippet, your body has several places to store easily accessible energy from fat and glucose.
Your liver holds a little bit of fat and some glucose in the form of glycogen. You can think of the energy your liver stores as your body’s primary go-to fuel tank that drip-feeds energy directly into your bloodstream as your body demands.
As we will learn later, your pancreas regulates the release of both glucose and fat into your bloodstream. The beta cells of your pancreas produce insulin to hold energy in storage while it uses up what’s floating around your bloodstream from the food you just ate.
To balance this, the alpha cells of your pancreas produce glucagon to promote the release of stored energy into circulation when you’re not eating.
Your liver and muscles also hold onto glucose in its storage form, glycogen. So, when you engage in activity between meals, you’re stressed, or doing a lot of vigorous exercises, your body breaks down this glycogen to fuel it.
Some of the protein stored in your muscles can flow back into the bloodstream to provide you with glucose (via gluconeogenesis). However, the glycogen in your muscles is locked away until you’ve used up the recently consumed glucose.
On the right-hand side, we can see the fat you’ve stored in the adipose tissue on your bum, belly, face and other parts of your body. Because you can store a LOT more energy as fat than glucose, your body uses fat stores as its primary fuel reservoir for when food isn’t so abundant.
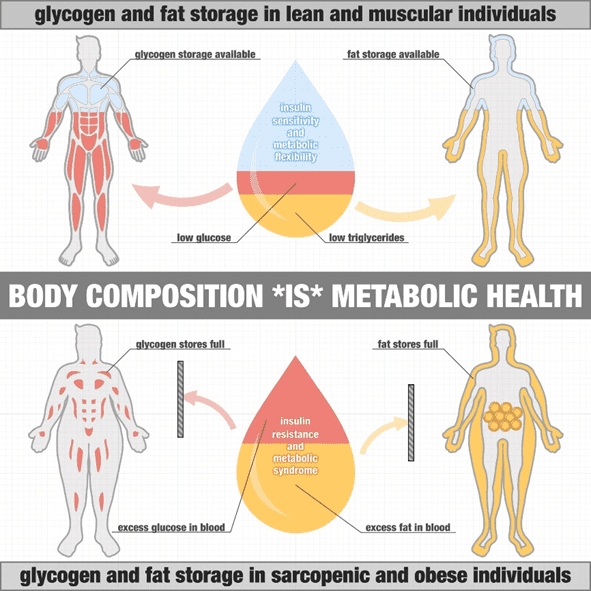
It’s important to note that the various fuel reservoirs in the version of the diagram above are NOT full! If you ate more fat and carbs, you’d easily absorb it and store it for later.
However, in the second version (below), everything is packed! The muscles and liver are full, and your fat cells have expanded to their maximum capacity.
This is where things get scary!
Your Metabolism
Finally, we come to the control system of your metabolism: your pancreas.
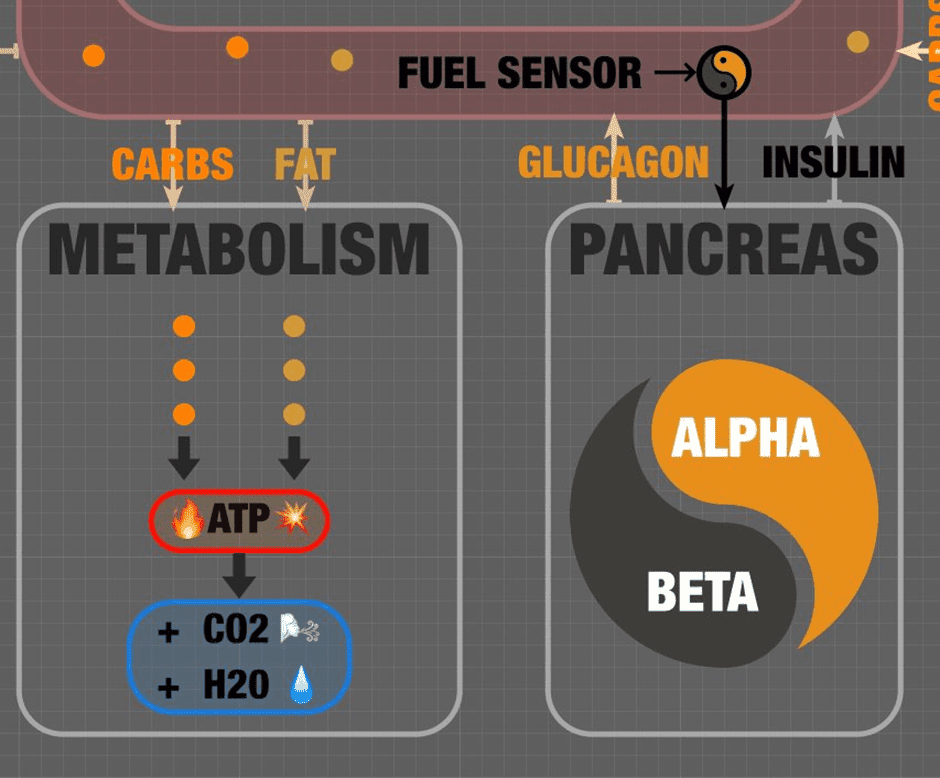
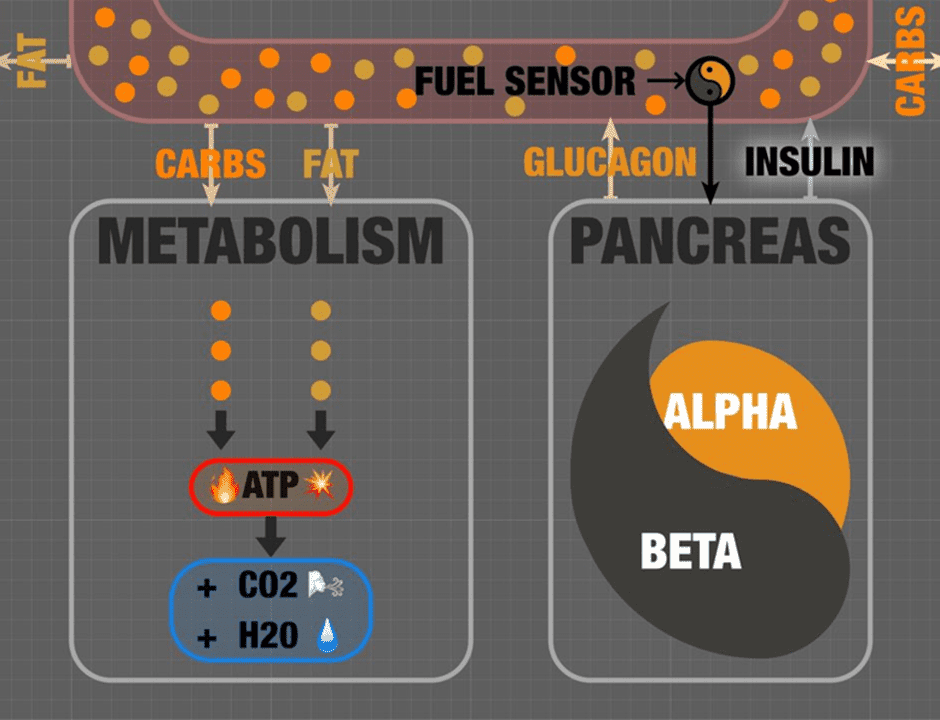
When your body needs energy—especially your muscles—it pulls glucose and fat from your bloodstream to your cells’ mitochondria to be oxidised. Your mitochondria are your cells’ little power plants that help convert glucose and fat to ATP.
Fatty oxidation, glycolysis, the citric acid cycle, and the Krebs cycle cumulatively take the energy from fat and glucose, producing ATP (energy), CO2 (which we exhale), and water. This process requires some help from the amino acids, vitamins, and minerals you consume from all the nutrient-dense food you eat.
Your pancreas controls this process, acting acts as a fuel sensor. The glucagon-producing alpha cells and insulin-producing beta cells work in tandem to balance the ebb and flow of energy as you cycle between fed and fasted.
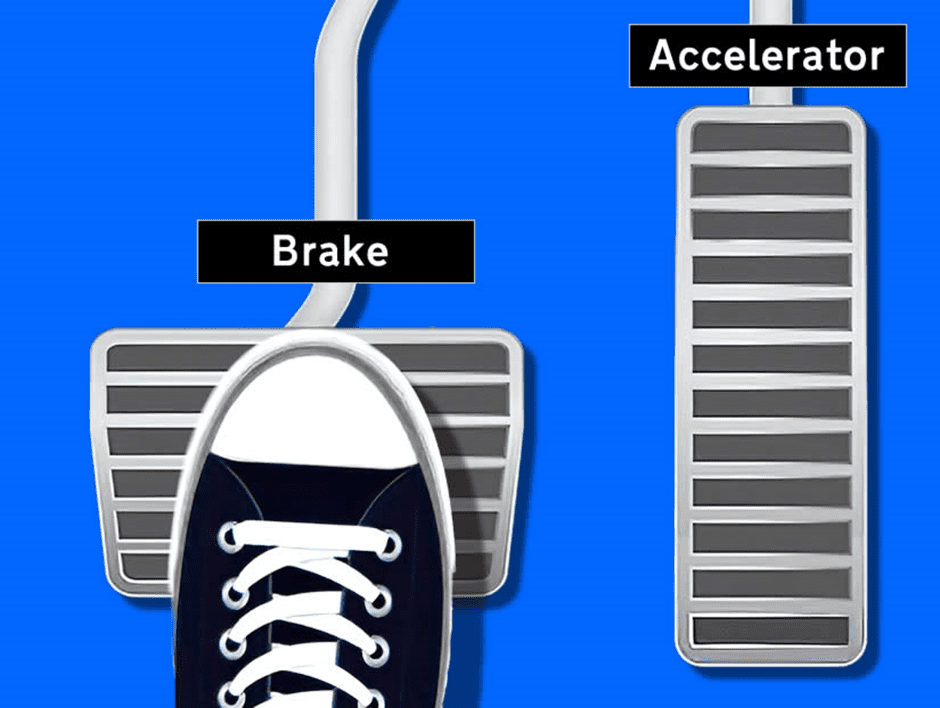
You can think of insulin as the brake pedal to your metabolism and glucagon as the accelerator. Like if in your car, you need enough—but not too much—fuel in your system at all times. If you don’t have enough energy, you will die.
But if too much energy circulates throughout your bloodstream, your metabolism will also choke. Hence, you need to find the ‘goldilocks’ dose of energy and the correct fuel ratio (i.e. macronutrient ratios) for YOU!
Remember how we mentioned that fat+carb combo foods signal that winter is coming and we need to eat more to get fat? Your body also has another mechanism to reduce energy expenditure to ensure you store more energy!
Check out this video if you want the biochemistry detail on the Randle Cycle or the process by which your body conserves energy when you have both fat and glucose in your bloodstream.
Insulin vs Glucagon
When the energy in your bloodstream is low, your pancreas secretes glucagon. This signals to the body to release more of your stored energy.
But when you have too much energy in the bloodstream, your pancreas will secrete insulin to hold energy back in storage.
People like my wife and son with Type-1 Diabetes have malfunctioning beta cells, so they don’t produce enough insulin. Hence, glucagon is unopposed, and energy as glucose, fat, and ketones is constantly released into their bloodstream.
When this goes on uncontrolled, it quickly turns into a dangerous state of excess energy in the blood. Blood sugars and ketones are through the roof, and someone may experience diabetic ketoacidosis. While this situation could end in death, it’s quickly remediated with injectable (exogenous) insulin. This allows the body to hold energy back in storage.
Insulin often gets a bad rep in some circles. But the reality is that insulin is critical to keep your body from disintegrating! If you’re part of the 99.5% of the population that has a functioning pancreas—and yes, this includes people with prediabetes, Type-2 Diabetes, or any form of metabolic syndrome—you can’t turn off your pancreas to stop producing insulin, regardless of how you mix up your macros. matter what you eat!
Insulin Response to Carbs vs. Fat
Our insulin response to carbohydrates vs. fat mainly differs because our bodies have such a limited capacity to store excess glucose. Your pancreas ramps up insulin aggressively if you eat a high-carb meal and your blood glucose rises; it must hold back ALL your stored energy until you’ve used up any excess glucose floating around your bloodstream.
Conversely, your body’s adipose tissue will happily absorb all the dietary fat you eat if you eat a high-fat meal and have plenty of spare storage capacity. As a result, you may see insulin rise slightly over the longer term, but this is mainly to hold extra energy in storage.
A healthy metabolism doesn’t rely heavily on insulin, especially if you’re active. While insulin is often thought of as the hormone that pushes energy into cells (i.e. via the GLUT1 transporter), this really only happens in an emergency when glucose and (or) fat in the bloodstream exceeds the body’s capacity.
Normally, energy floats across the gradient from an area of higher glucose concentration to a lower one (via GLUT4 transporter), replenishing the energy as it is used. The 2011 study by Krakoff et al. titled Assessment of Non-insulin Mediated Glucose Uptake: Association with Body Fat and Glycemic Status showed that 83% of glucose uptake occurs through non-insulin mediated mechanisms like GLUT1 glucose transport.
On average, your body clears 1.6 mg/kg of glucose per minute from your bloodstream without using any insulin. That’s more than 160 g of carbs per day for the ‘average’ 70 kg man. So, if you’re on a lower-carb diet, all of the glucose you eat could be used without insulin!
Insulin Resistance and Energy Toxicity
But things get funky when our liver, muscles, and adipose tissue reach their limits and become overfull with energy. In this instance, our pancreas senses high levels of fuel in the blood. This forces the beta cells to ramp up their production of insulin in an attempt to keep the ever-growing pool of energy stored in our liver and adipose tissues tucked away.
In the diagram below, notice how Ted made the beta cells much larger than the alpha cells. That’s because they’re working overtime to stop all your excess energy from flowing into your blood!
Once our adipose tissue is overfull, it becomes harder and harder to keep fat in storage. Like balloons ready to burst or saturated sponges that can no longer hold more energy, insulin can no longer do its job effectively to resist the pressure of our now-full fat cells.
Before long, we become ‘insulin resistant’, and energy overflows into our bloodstream as high ketones, blood glucose, cholesterol, and triglycerides.
Over time, our poor little beta cells get tired and burn out once they can no longer match the body’s insulin demands. At this point, you can develop double diabetes, which entails high levels of insulin resistance and a worn-out pancreas that can’t make as much insulin as before.
What’s the Root Cause?
Sadly, many people with diabetes are told it’s an irreversible and progressive disease that requires more and more medications until the day they die so they can fend off the numerous complications that accompany the condition. However, this thinking is far from the truth… at least if you’re willing to put in a little effort!
To understand the solution, we must first comprehend the fundamental problem.
- Insulin is not the problem; high insulin is simply a response to the problem. We need enough insulin to survive and regulate the flow of fuel into our blood.
- Carbohydrates are also not the problem. Humans now and thousands of years ago consume carbohydrates regularly and never develop diabetes.
So, if it’s not insulin resistance or insulin toxicity, what is it then?
The fundamental problem is energy toxicity. Our nutrient-poor, low-satiety diet has driven us to eat more than we need or that our bodies can handle, and we exceed our body’s capacity to store energy, or our Your Personal Fat Threshold.
What’s the Solution?
To address and reverse energy toxicity, we need to change WHAT and WHEN we eat. It’s not simply a matter of limiting calories; we always eat when we’re hungry until we feel full or satiated.
How much we eat matters, but unless we change the quality of the food we eat and begin giving our bodies what they need, we will only be able to consciously control the quantity of these foods we’ve been consuming for so long. We can do this by packing more micronutrients into each calorie we consume or by improving the nutrient density of our food.
Rather than eating all day, some form of structured time-restricted eating can also help. This allows us to offload the extra energy we have on board when we aren’t eating.
Reducing carbohydrates can help to reduce one of the symptoms of diabetes: elevated blood sugars. This can help get us off the blood sugar rollercoaster so we can stop falling victim to caving into cravings when our blood sugar comes crashing down. Reducing our carb intake also moves us out of autumn and into winter.
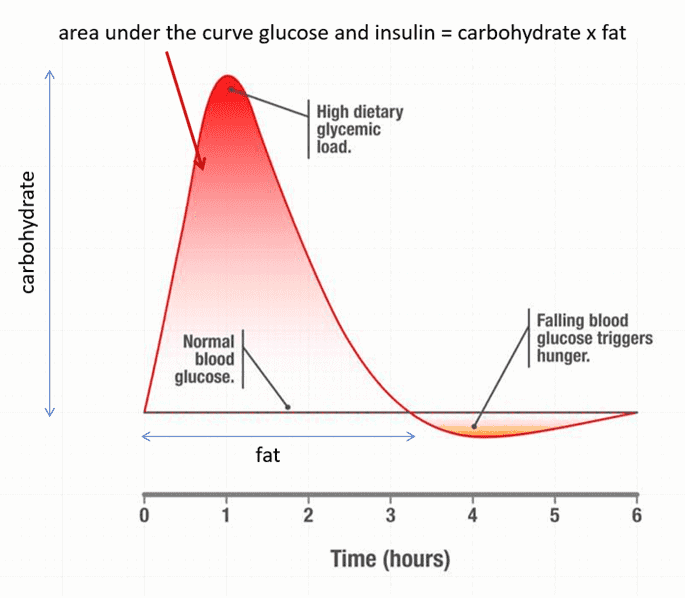
While going lower-carb can be a helpful band-aid to support our bodies until they’ve offloaded some extra energy, swapping carbs for dietary fat does not always help us reduce our body fat unless we lower our overall energy intake.
We can do this by moving from winter into spring and embracing the high-protein, fibrous carbs available to us. In time, we will be able to lose our winter blubber and regain our metabolic health.
What Can We Measure?
Before falling into the world of nutrition and human metabolism, Ted and I were engineers. Our backgrounds helped us understand a little bit of measurement goes a long way to achieving your desired outcome (quality control, too). With that being said, we’ve included a few things you can measure to improve your metabolism and reverse energy toxicity.
Premeal Blood Glucose
The simplest and most effective thing we’ve found to determine WHEN and WHAT you feed yourself is to measure your glucose before (not after) eating.
You can use a simple glucometer as your energy sensor or fuel gauge. We’ve found that this is the most effective way to stay in tune with your true hunger signals and understand your body’s true need for food.
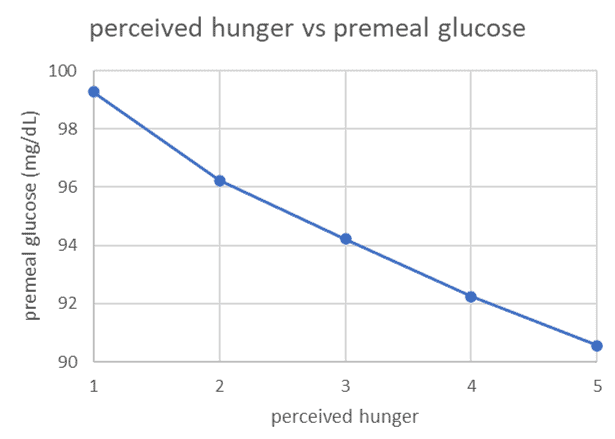
Using over two years of data from our Data-Driven Fasting Challenges, we’ve found that lower premeal glucose correlates strongly with your hunger levels and actual need for food.
Aside from telling you when to eat, your blood glucose also indicates what to eat at any point in time. In our Data-Driven Fasting Challenges, participants use the DDF App to identify their personalised glucose trigger. From there, they receive guidance on WHAT to eat when they are hungry based on their meter readings.
| Glucose | Guidance |
| Above the upper limit after a meal. | You’ve overfilled your glucose fuel tank. Next time, eat less of whatever you ate or eliminate it from your repertoire. |
| Significantly above trigger. | Wait! You don’t need to eat yet. You’ve got plenty of fuel on board! |
| Just above trigger. | Ideally, wait to eat. If you’re particularly hungry, prioritise nutrients and protein and consume less energy from carbs and fat. |
| Just below trigger. | Eat ‘normally’. |
| Significantly below trigger. | Consume enough whole-food carbs to bring glucose back to your normal range to quickly alleviate extreme hunger from low glucose. |
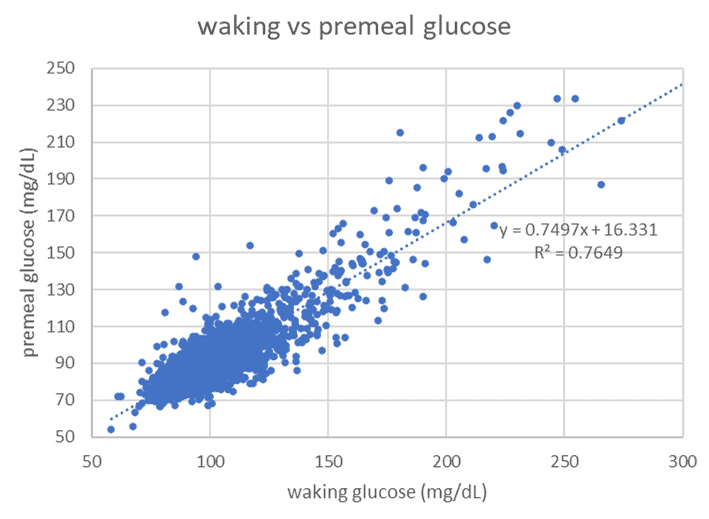
The DDF app also calculates a progressively lower trigger. Throughout our DDF challenges, participants continue to ‘chase’ this lower trigger to keep unloading the extra energy they have on board. A lower premeal glucose aligns with lower waking glucose, reduced waist measurement, and fat loss.
Macronutrients
Our satiety analysis of 125,000 days of data from 35,000 people shows that fat and carbs affect satiety similarly.
So, if you want to reduce your glucose and lose body fat, you must decrease dietary fat AND carbohydrates to move out of autumn and away from a modern processed diet towards a Protein-Sparing Modified Fast-style-like diet with the type of foods that would be available in spring (i.e. more protein and fibre).
Over the past sixty years or so, our intake of both carbs and fat has increased within our food system.
In percentage terms, we now consume an ominously similar blend of fat and carbs. However, our intake of satiation-dependent protein has fallen. With satiety low and our calorie intake on the rise, it’s no surprise that our obesity rates have only continued to climb.
To reverse this trend, turn back time, and rescue your metabolic health, you can progressively dial back energy from fat and (or) carbs and prioritise protein and nutrients. This will allow you to stay full, reduce your calories, and keep your hunger at bay so you can begin burning stored fat for fuel.
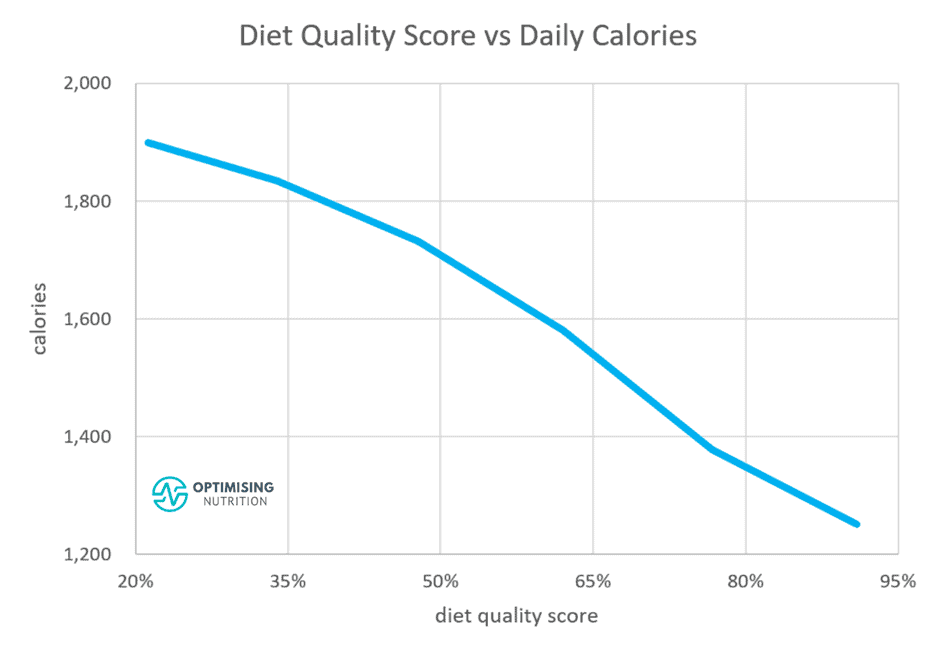
As the chart below shows, increasing protein % aligns with a marginally higher protein intake (in grams) but a significant reduction in calories.
While this knowledge might have you running out to buy all the egg whites, lean steak, and chicken breasts you can, the key is to not jump from one extreme to the other overnight. That is never sustainable, and you’ll be overwhelmed with cravings for easy energy from fat or carbs before long!
Instead, you need to determine where you currently sit on the macronutrient spectrum and gently tweak your macros over time, as we do in the Macros Masterclass. There are no overnight solutions to long-term problems, but this is a sure way to lose weight—and maintain it sustainably!
Micronutrients
Finally, if you’re looking to get even closer to Nutritional Nirvana, you can dial in your micronutrients as we do in the Micros Masterclass. Getting enough amino acids is only the first step!
Aside from protein, your body also craves all the vitamins, minerals, and essential fatty acids it’s currently lacking. Once you get everything your body needs from the food you eat, it’s ‘satisfied at a cellular level’ (as one of our Optimisers described it) and happy to use your stored energy to fuel itself. Before long, you’ll be well on your way to reversing energy toxicity.
I hope these insights from Ted’s infographic and our tools and tips help you reverse your energy toxicity and move towards more optimal metabolic health!
Best of luck on your journey, and we hope to see you again soon!












Hi, excellent stuff. I was quietly thinking how to visualize the metabolic process around bloodstream etc, I have to dig no more. Maybe add something from my favourite incretin hormones GIP and GLP on the gut section…
I guess it was made in the name of simplicity, but direct arrows from bowel to blood vessel re. carbs and prots bypasses the filtering of the liver. I never stop wondering how the long-chain fatty acids can go directly to the bloodstream, just in front of the heart…
One question: the “rabbit starvation” i.e. 100% protein diet and above 200g per day does not hit you if there is some fat added to the mix? otherwise 50% protein share would not be possible? Please expand.
rgds JR
RE rabbit starvation… it’s hard to make a sustainable diet that is 100% protein – protein tends to come with some fat. But if you did manage to live on egg whites, protein powder, cod and collage (which are not 100% protein), you would get severe cravings for energy. It’s hard to make ATP from protein. See https://optimisingnutrition.com/psmf/
In our Macros Masterclass, we guide people to find the balance between protein and energy the achieve their goals at a sustainable rate. Between 0.5 and 1.0% weight loss per week tends to be sustainable without leading to rebound binging. https://optimisingnutrition.com/macros-masterclass/