Exploring the realm of GLP-1, we delve into the burgeoning interest in GLP-1 receptor agonist weight loss drugs like Ozempic and Wegovy.
While these drugs offer a promising avenue for weight loss, the story doesn’t end here. Uncover how natural GLP-1 agonists present a holistic approach to weight management.
Discover how to increase GLP-1 naturally, understand the potential of GLP-1 supplements, and unlock the secrets of natural GLP-1 agonists.
As you traverse through this elucidative guide, you’ll find answers to “How can I increase my GLP-1 naturally?” unveiling a path to satiety without the needle.
Background
Interest in GLP-1 receptor agonist weight loss drugs like Ozempic, Wegovy, Mounjora, and Trulicity is exploding!
It’s easy to get excited about these satiety-inducing drugs, especially if your scale has done nothing but climb with no hope in sight.
When we look at the big picture, it looks like the deck is stacked against us.
- First, food corporations create a hyper-palatable, ultra-profitable food system that makes you feel ‘addicted to’ the only nutrient-poor, hyper-palatable foods that are affordable.
- Then, we create high-priced drugs that mimic our satiety response to nutritious food.
- But if we keep eating the same food, we get fewer nutrients and become dependent on these drugs.
These new drugs could be life-changing for the many who desperately need to lose weight for their health, especially if they are able to build new habits and optimise their nutrition.
In this article, we’ll look at:
- How these new drugs work,
- Why they are prescribed for people with Type 2 Diabetes,
- The risks and the cost,
- How much weight can you lose, and what are the chances of gaining it back when you stop?
- How GLP-1 works in your body, and
- How you can increase GLP-1 naturally.
How Do Injectable Weight Loss Drugs Work?
The main active ingredient is Semaglutide, a glucagon-like peptide-1 (GLP-1) receptor agonist.
Your gut and brainstem naturally produce the signalling hormone GLP-1 after you consume food. GLP-1 signals satiety and lowers your hunger after eating.
GLP-1 is also an incretin hormone and hence enhances insulin and suppresses glucagon secretion in your pancreas, thus lowering blood glucose.
An agonist is “a drug that binds to a receptor inside a cell or on its surface and causes the same action as the substance that normally binds to the receptor”. So, the GLP-1 receptor agonist works because the drug binds to a receptor and acts like your endogenously produced GLP-1.
So, with the support of these drugs, someone is less consumed by thoughts of food, eats less, and can lose weight from the energy deficit they create and maintain their lowered calorie intake over the long term with the help of these drugs.
In addition to Semaglutide, there are a few other variants on the market or in the pipeline:
- Mounjaro is a GLP-1/GIP agonist, which means it also mimics glucose-dependent insulinotropic polypeptide (GIP).
- Carinlintide mimics amylin, another pancreatic hormone that influences satiety.
- Retatrutide is a GLP-1/GIP/glucagon agonist that will also encourage your liver to release more energy in addition to increasing satiety.
These medications are injectable satiety; they’re as close as we’ve come to the “magic pill” for weight loss. So, there is a lot of reason to be excited about them.
Why Is Semulglutide Used for People with Diabetes?
Rather than injecting more insulin, GLP-1 receptor agonists increase your body’s endogenous insulin and increase satiety, which helps you eat less. So, instead of just managing the symptom of T2D—erratic blood sugars—with injected insulin, these new drugs help to address the root cause—energy toxicity.
However, thanks to TikTok influencers and celebrity use, many people without diabetes are now asking their doctors to prescribe these drugs to help them lose weight. There is currently such a shortage of these drugs worldwide that doctors have been asked to stop writing new prescriptions until suppliers can produce more.
How Much Weight Can You Lose?
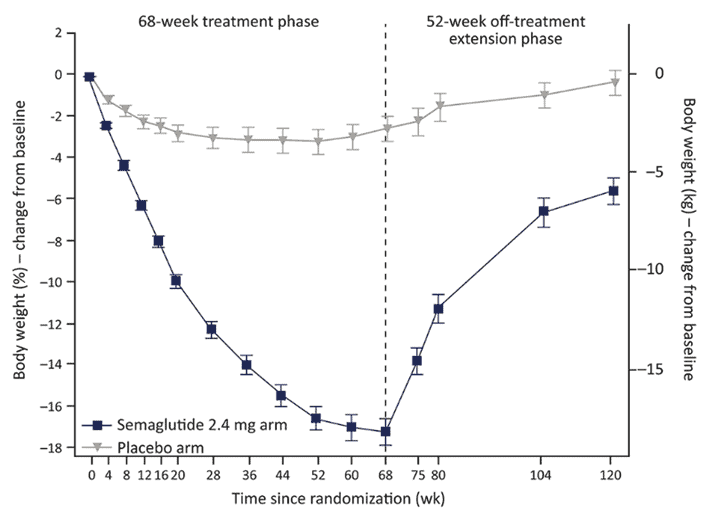
With the increased satiety from GLP-1 analogues, weight loss is quite promising. With a mean weight loss of 14.8%, the progress decimates the 2.4% weight loss in the placebo group (Garvey et al., January 2023). However, it’s interesting to note that the weight loss effect plateaus at around 60 weeks.
There has also been a lot of discussion on whether the benefits last after stopping taking these drugs, especially if no diet or lifestyle changes are made while on them. While some report that these drugs give them the control to develop new habits, many others have found have gained back the weight once they stopped.
The chart below from Weight regain and cardiometabolic effects after withdrawal of semaglutide also shows a rapid regain after stopping taking the drugs. In addition, researchers also found that participants’ cardiometabolic improvements reverted once their weight returned to their baseline and they regained what they had just lost.
How Much Do They Cost?
While the weight regain is concerning, the cost is the real sticking point; Wegovy’s monthly list price in the US is $1350!
That’s $16,200 per year or 30% of the average American’s annual salary!!!
Fortunately, health insurance often covers this cost if prescribed by a doctor. However, many insurance companies are starting to push back to manage their expenses.
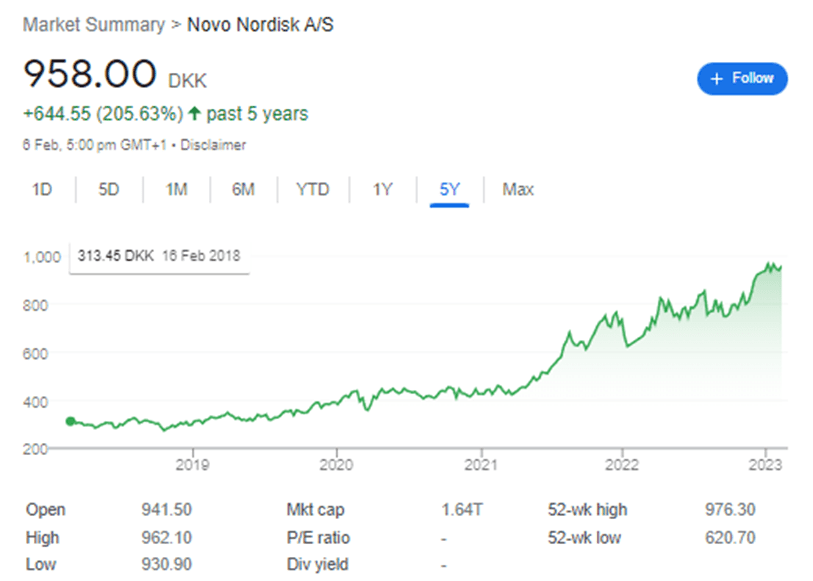
But the cat is out of the bag for these new GLP-1 drugs. Everyone is talking about them! This definitely hasn’t hurt Novo Nordisks’ share price.
But if we do some quick calculations, if everyone who was obese in the US went on Wegovy, someone would have to foot a bill of $3 trillion per year.
That’s 10% of the United States’ massive $31 trillion national debt every year!
I wonder how long this can continue before health insurance rates become more expensive for everyone.
These drugs are certainly helpful for people to avoid the many complications that stem from metabolic syndrome, T2D, and obesity. However, the financial equation becomes very challenging if everyone who wants to be a bit leaner starts using these drugs.
How Can I Increase My GLP-1 Naturally (for Free)?
If you can’t afford GLP-1, cannot get a prescription, or want to do things without medication, you may be interested in how to increase your GLP-1 naturally.
As we mentioned earlier, GLP-1 is a satiety-inducing peptide hormone that your body naturally produces in response to food, but not just any food!
A 2016 paper, Nutritional modulation of endogenous glucagon-like peptide-1 secretion: a review (Girous et al., 2016), found that GLP-1 is stimulated more by foods rich in nutrients.
In another study, High-protein intake stimulates postprandial GLP1 and PYY release (Faroqui et al., 2012), protein was shown to stimulate GLP-1 more than fat and carbohydrates. Additionally, it showed that GLP-1 tends to align with our insulin response. So, it’s likely that GLP-1 follows a similar pattern as your blood glucose and insulin. Incorporating foods that increase GLP-1, like those rich in protein, can be beneficial.
In our Data-Driven Fasting Challenges, we guide participants to use their blood glucose as a fuel gauge and eat when their glucose is lower than normal. They also learn to prioritise protein when they are hungry, and their glucose is higher than normal.
Unfortunately, most of the interest in GLP-1 has been around patentable drug treatments rather than nutritional interventions, so we don’t know much about how our GLP-1 production responds to various nutrients in your food.
However, we know from our satiety analysis that the protein % of our diet impacts how much we eat throughout the day more than any other parameter. Protein, fibre, and other nutrients like potassium, calcium, sodium, and particular vitamins also tend to align with eating less, but not quite as much.
In converse, food containing more energy from carbs and fat and less from protein and fibre tend to align with eating more, especially when combined in ultra-processed foods.
While the new messaging seems to be that obesity is a genetic disease that we can manage with drugs, there’s undoubtedly more to why conditions stemming from metabolic syndrome weren’t so common half a century ago. Although genetic factors are certainly at play, nature (genes) vs nurture (environment) still holds true, and our food system has changed.
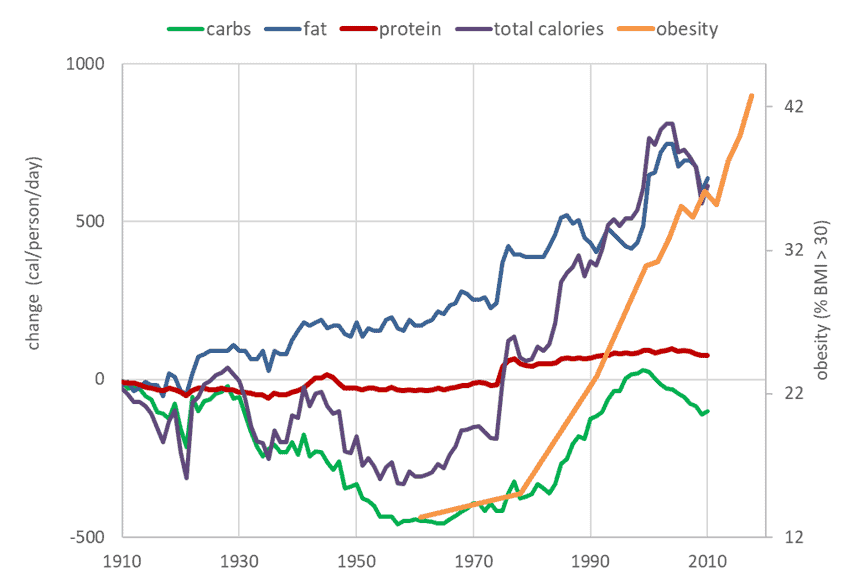
As the image below shows, fat consumption has been steadily rising over the last century since we discovered how to extract oil from crops at scale, fuelled by synthetic fertilisers. Meanwhile, our carb intake has risen since the agricultural revolution.
Together, these add up to a lot of extra cheap and tasty extra calories from ultra-processed foods that we love to overeat. Because our carb and fat intake has increased so much relative to carbohydrates, our overall per cent of total calories from protein (i.e., protein %) has decreased. It’s no wonder obesity is rising at such an alarming rate!
To learn more, check out How to Maximise Satiety Per Calorie. You can also join our Optimising Nutrition Community to access our food lists and meal plans that will help you increase your satiety naturally.
What About Nutrients?
Q: Why do we want to eat?
A: For pleasure.
EH! Wrong answer.
A: To get the nutrients and energy we require.
Bingo!
In recent years, studies looking at factors influencing eating disorders like binge eating, bulimia, and even anorexia have shown many probable causes, including mental and emotional stress as well as nutrient deficiencies.
Feel-good ‘happy’ neurotransmitters like dopamine and serotonin are synthesised from amino acids like tyrosine and tryptophan. Additionally, various vitamins and minerals like vitamins B1, B6, B9 and C and minerals like magnesium, zinc, and copper serve as catalysts for these reactions. Gut health also becomes essential, especially for serotonin synthesis.
So, if you suffer from one of these conditions and you’re not consuming adequate nutrients, you’re more likely to return to your old habits once the effect of the weight loss drugs wear off.
Much research—including our own—points to nutrients as the most critical factors for satiety. In other words, if you’re not getting enough of them, your body will send you in search of the vitamins, minerals, essential fatty acids, and amino acids you’re lacking by making you eat more.
Unfortunately, our modern food environment has replaced essential nutrients like protein, minerals, and vitamins with lots of cheap energy. Whether by accident or design, it has lowered the satiety value of our food and forced us to eat more of these cheap but profitable foods. As a result, we now have to consume more energy to get the nutrients we require to thrive.
Our work on satiety and nutrient density enables us to reverse engineer hunger and satiety to get the nutrients we require without excess energy. But, when it comes to weight loss in a pill—or, in this case, an injection—people will no longer be hungry for the nutrients they need.
As a worst-case example, a person may have eaten two or three chocolate muffins before they started the weight-loss drug, but they are only hungry for one. While these muffins likely provided little in the way of real nutrients, they contain some synthetic (fortified) ones. Thus, they consume fewer nutrients than they require to thrive long-term.
While these people may achieve weight loss, their body composition may deteriorate unless they consume adequate protein. Additionally, their overall health might decrease unless they incorporate nutrient-dense whole foods that provide other vitamins, minerals, and essential fatty acids, all of which increase GLP-1 naturally.
Satiety-inducing drugs don’t change your requirements for nutrients from your food. In fact, when you’re eating less, nutrient density becomes even more important! If you’re eating less, it’s critical to find a way to pack more of the nutrients you need into fewer calories!
In an ideal scenario, someone could initially use Semaglutide to lose weight while they develop new lifestyle habits that allow them to make better food choices. Essentially, the drug becomes a bridge to get them to a healthier lifestyle.
As the results below show, craving control tends to improve initially. But interestingly, the studies show that cravings seem to come back after two years, especially for sweets. This may be why the weight loss results start to slow after a year or so.
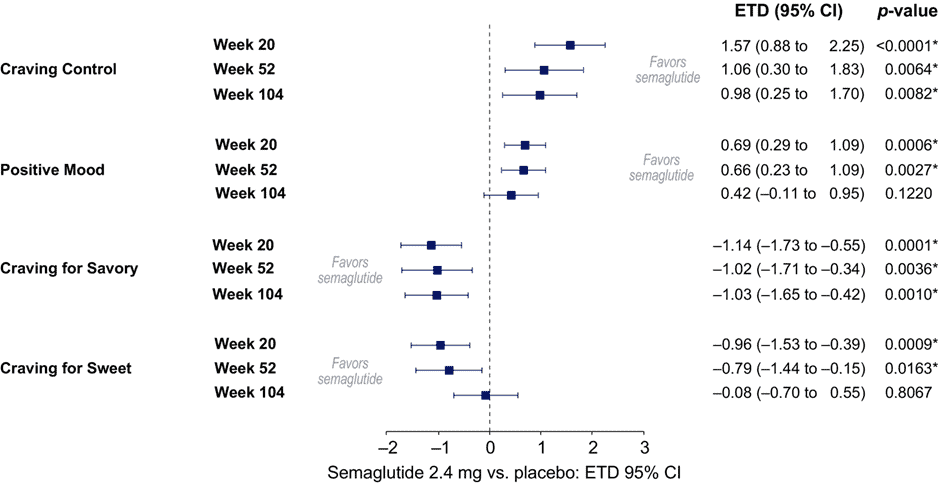
What happens if someone is undernourished after years of eating a poor diet on these appetite-suppressing drugs and then gets to the point they can no longer obtain them?
Without building new habits around food, will all their cravings instantly return as their body seeks out the nutrients they have been missing?
Or if they stay on them long term without improving food quality, will their bodies be forced to trudge through nutrient deficiency into new diseases?
I suppose time will tell.
Happy Ending
I had hoped to be more positive in this article. But I think there are some nutritional issues worth highlighting.
I hope you can use this information to consider whether or not these drugs are right for you.
To finish, I wanted to share some positive stories from people who have used these weight loss drugs in our groups.
My hormone doc suggested giving semaglutide a try (Ozempic, Wegovy). And it has worked wonders for me! I am still fasting, tracking blood glucose, and prioritising protein and nutrients, but it was a game-changer. It has been a challenge going through perimenopause and fluctuating hormones. This gave me more freedom, or a bridge, if you will, to balance hormones. I am now on Mounjaro, which has worked well at a low dose. It has helped with other areas in my body that have surprised me. I am down 25 lbs and now maintaining. — Joanne
I’ve been on the drug for Type-2 Diabetes for two years now and lost 25 kg of mostly (92% by my calculation) body fat… Independent of Optimising Nutrition, I discovered I could use my blood glucose levels to optimise fat loss whilst on this medication. I noticed that I consistently lost weight when I only ate below my blood glucose trigger of 4.8 mmol/L. Then I found Data-Driven Fasting, and your evidence backed up my experience. My GP said none of her other diabetes patients on Ozempic had had as good a result as mine… so what I was doing was the critical difference.
I was on Januvia, Metformin and Gliclazide and exercising *hard* at the gym, but not losing body fat very quickly, up at 36% body fat. I’m now on Metformin and Ozempic, down under 22% body fat and down 25kg, 23kg or so of which is fat.
But primarily because I noticed that I lost weight when I stopped eating until my glucose was low. I also started using my blood glucose to avoid the hypos I started getting when Ozempic was added to my three other meds.
My biggest concern with weight loss in a pill (or, in this case, an injection) is that people will no longer be hungry for the nutrients they need. It’s already an issue with weight loss surgery, where it’s a permanent state of affairs afterwards. At least with a pill, you can come off it. Last week I was diagnosed with low iron levels after 2+ years on semaglutide, even though I prioritise protein.
I am an admin of 30,000+ folks in the Ozempic Facebook group. I often feel they would benefit from Data-Driven Fasting. I like DDF because it addresses this single most challenging aspect of dieting: when should I eat, and can I train myself to eat less? — Paul Antoine
This is definitely a complex topic, so feel free to share your thoughts and experience below to add to the discussion!
Summary
- GLP-1 receptor antagonist drugs are an exciting new frontier in weight loss. However, they are expensive, meaning everyone living with obesity may not have the chance to use them.
- Studies show a dramatic initial weight loss that slows after 60 weeks as the appetite-suppressive effects appear to diminish.
- Once people stop taking these drugs, most seem to regain their lost weight.
- Maintaining a healthy weight is undoubtedly more challenging in today’s modern food environment. However, we do have a solid understanding of the properties of food that leads us to eat more or less. Therefore, changing what you eat directly impacts how much you will eat.
- Simply eating less of the same nutrient-poor foods with artificially lowered hunger is not ideal. Hence, it’s wise to do everything you can to dial in your food choices, eating habits, and appetite to ensure long-lasting results whether or not you’re using these weight loss drugs.









The one thing they never tell you when you start these drugs…when to stop. The trick is YOU DON’T STOP! When you do–instant rebound, just like with normal dieting. This is the thing the doctors and shareholders don’t want you to find out, because it’ll cut into their revenue stream.
When you mention “becoming dependent”, you aren’t kidding in the least! The keto diet taught this to me. Whatever you do (or did) to lose the weight becomes a LIFESTYLE , not a one-shot deal.
For me, full-boar keto was no longer the answer, so rather than focus on the weight loss, I now make adjustments within the keto framework, and focus on OVERALL HEALTH. The injected GLP-1 crowd is paying out big bucks and yet still missing the ball, because they’re focused on the wrong thing. Their doctors are ecstatic, I’m sure, as are the shareholders of the GLP-1 companies, but it really amounts to better living through man-made chemistry. What happens when the chemicals stop coming? Then one needs to switch to manual backup…that’s where Marty and his Nutrient Optimizer come in, if one cares enough about their health to clear the calendar for some cooking time.
These drugs, to me, are like Dirty Keto–a “quick and dirty” way to sort of accomplish the same thing–it may be quick, but the true emphasis should be on dirty.
Well written, Marty.
I think you’ve presented a thought-out, balanced perspective.
Nutrition for the long term win.
Cheers!
Bob Farrell
Nutrition coach, Pn1
thanks Bob! this is a tough topic to navigate!
So well researched and written Marty. I love it when you educate me – thanks teach!
Thank you!
Great article, Marty; thanks!
I think it’s worth mentioning the potential side-effects of semaglutide (it carries a black box warning, which is the FDA’s most serious warning), such as: thyroid c-cell tumors, acute pancreatitis, acute gallbladder disease, hypoglycemia, acute kidney injury, hypersensitivity, diabetic retinopathy complications, heart rate increase, suicidal ideation and behaviors. That’s in addition to its common side effects which include nausea, diarrhea, vomiting, constipation, stomach pain, headache, fatigue, upset stomach, dizziness, feeling bloated, belching, gas, stomach flu, and heartburn.
Separately, amid the hype around GLP-1 agonist weight loss medicines, no one is talking about the fact that much of the “weight loss” resulting from GLP-1 agonists is the loss of muscle, bone mass, and other lean tissue rather than body fat. For more on this, read this excellent article: https://www.psychologytoday.com/us/blog/the-healthy-journey/202208/how-get-the-most-weight-loss-medications. Could this explain (at least in part) the rapid weight regain upon stopping Ozempic?
I’m a nutritionist and have several clients who have been prescribed Ozempic by their doctors; they are so tired from their low calorie & nutrient intakes that they struggle to get through the day, let alone engage in the sort of resistance training that wd be necessary to retain and gain lean tissue.
I agree with you: Ozempic & Co may be helpful for many, but in order to achieve sustainable results, these drugs should be accompanied by changes in nutrition, exercise, sleep & stress management habits. In the age of the magic bullet, good luck with that…
Thanks for your awesome work, Marty. (Do you ever sleep?)
Warmly,
Conner
Thanks Connor
In the first version of this article, I mentioned the long list of adverse symptoms but removed it to make it more digestable and stay in my lane. I also had a blurb about all the MANY weight loss drugs from the last few decades that were initially EXTREMELY popular and then withdrawn due to safety issues and adverse effects when rolled out at scale.
It makes sense that if people are eating less of the same stuff that made them overeat they will lose lean mass and bone mass unless they radically change their diet using GLP-1 receptor antagonists as a bridge.
Cheers
Marty
These are the deleted sections RE side effects and the history of weight loss drugs.
The Risks and Side Effects of Injectable Weight Loss Drugs?
There is a wide range of commonly known side effects of these new GLP-1 receptor antagonists, including:
• nausea,
• vomiting,
• diarrhea,
• acid reflux,
• heartburn,
• burping,
• flatulence,
• vomiting,
• dizziness or light-headedness, and
• headaches.
The Ozempic website also notes complications, including:
• thyroid tumours,
• pancreatitis,
• hypoglycaemia,
• kidney failure,
• allergic reactions, and
• gallbladder problems.
Additionally, a recent study showed that GLP-1 accelerates breast cancer progression (Quin et al., 2022).
The use of these drugs during pregnancy has not been tested, so it is recommended that women come off the medications five weeks before trying to fall pregnant.
Many clinical trials have been done on the safety and efficacy of these drugs before their release. However, we will surely learn more about how they affect people over the long term in the coming months and years.
The History of Drugs for Weight Loss
It’s worth noting that there is a long list of failed anti-obesity medications in the past. Most of these medications were extremely popular and then withdrawn due to safety concerns or have fallen out of popularity due to side effects. A few examples include:
• 2,4-Dinitrophenol (DNP), which works by opposing oxidative phosphorylation in the mitochondria. This causes you to produce heat rather than usable energy in your body (ATP). The US Food and Drug Administration (FDA) withdrew DNP from the market in 1938 after adverse side effects like overeating and fatal hyperthermia started to appear.
• Amphetamines became popular in the 1930s due to their appetite-suppressing effect and increased alertness. However, they were banned in the 1960s because of the many deaths caused by overuse.
• After banning DNP, the FDA approved phentermine and fenfluramine. Later, in 1992 it was found that the two produced an average of 10% weight loss when combined. Fen-phen was then created—a combination drug of the two compounds—which quickly became the most prescribed diet medication until it was found to cause valvular heart disease in almost 30% of the people who took it. Thus, Fen-phen was withdrawn from the market in 1997.
• Orlistat (or Xenical) inhibits fat absorption. While it is still used today, it has decreased in popularity due to the side effect of ‘anal leakage’ that occurs when undigested fat passes straight through you.
Overall, 25 anti-obesity medications have been withdrawn from the market since 1964 due to safety concerns.
As much as we all want to be ‘biohackers’ and use everything available to us to be ‘superhuman’, there is usually no ‘free lunch’ in biology. Because of your body’s innate feedback mechanisms, there is unfortunately often a catch to anything that appears too good to be true.
Only time will tell if the new GLP-1 receptor antagonists stand the test of time based on their side effects when used at scale.
Thanks Marty. This is sad but true that we are now medicalizing satiety even in regards to children vs root cause solutions. I have used these meds frequently in severe diabetes and for many they have been helpful. But what is happening now is unacceptable at so many levels. GLP1 is not proprietary to the drug companies. We need to re-educate the population that our intestines make these peptides and always have. Mark Cucuzzella MD
Thanks Mark!
I hope we can educate people to increase satiety/GLP-1 with food.
Can’t wait to meet you in Denver. Maybe I can be your warmup act!
Cheers
Marty
Excellent article Marty, and very timely – it was announced here in the UK 3 days ago that the NHS is going to make Wegovy available on prescription for just £73 per month! I sense a forthcoming acceleration of the current chronic health crisis: my take is that GLP-1/ GIP agonists are only of benefit for up to 1 year for those people using them as a bridge, ie at the same time they are incorporating nutrition & lifestyle change, with a clear plan to drop the meds after 12 months. That’s certainly the way I’d approach it with my clients if they were dead set on using them. In reality though, what % of people will do that? Less than 1% I’d wager. It seems human beings are just wired to take the ‘easy’ solution… Which leaves 99% worse off after 1 year, facing the triple whammy of potential weight-regain, increased cravings and the consequences of chronic under-nutrition really beginning to kick in….
Agree. Everyone wants the quick and ‘easy’ solution, no matter the cost.
I worry about the long term cravings after a year or two of under-nutrition.
I believe there is a genetic component to obesity and that the rich foods we have mass produced and made available have led to the massive increase in obesity. My grandmother, born in rural America in the early 1900s, was actually obese from an early age. One of her children was also. In each of their families. one child was obese. Now in the great grandchildren and gg grandchildren, more are obese. My observation is that my brother and the overweight cousins always seemed hungry and ate more. We ate the same meals which were not always great nutrionally but better than a fast food meal. All that to say I think the pharmaceuticals could be very helpful for those people who may not be getting proper satiety signaling. I agree the best chance of long term success will be to re-program your brain and body to eat for health and nutrients while on these drugs, and then they would probably do better when they come off. When I first heard of these drugs being used by celebrities, the first thing I looked up was what can increase it in foods. Surprise, healthy foods. We can each change our food preferences by eating the good foods, but if we don’t fix our food supply and habits, there is no hope of solving this problem long- term for society.
Agree. It’s the food system that has changed the most over the past 80 years or so.
Not sure how we’re going to fix the food system, but I hope we can help some people increase their GLP-1 for free.
I’ve been on semaglutide for 47 weeks. It has been the best decision I have ever made. In that time I have dropped 28% of my body weight. I’m the thinnest (and healthiest) I have ever been. I’ve gotten DEXA scans along the way and can say that my lean body mass has only declined slightly. I am currently around 26% body fat. I went through all 3 of your programs (DDF, Macros, Micros) several months before starting on Semaglutide, and have stuck with the programs. I also exercise and focus on strength building. In addition to losing fat, my cholesterol is now normal, my A1c is normal, and my inflammation markers are normal. So while the cost may be high, there is great value, for me personally and society at large, in no longer being at risk for heart disease, diabetes, and various forms of cancer.
I don’t know what the endgame will be. I’m still trying to get down to below 25% body fat, but my weight loss has dramatically slowed in the last 8 weeks. As you point out in this article, I have noticed that by the end of each week the drug has worn off and I definitely eat more. I had hoped that by following your programs while using semaglutide that I would be able to achieve satiety consistently enough to be able to maintain my weight without the aid of the drug, but that hasn’t happened yet.
I tried Ozempic back in September of 2022. I noticed that on the initial dose of 0.25 ml my Dawn Phenomenon was decreased by about 40 points (from 210-220 to 170 US measure). However, my afternoon lows INCREASED by 30 points (from 110 to 150). I developed extreme shortness of breath, as well as unrelenting twitches of my right eye, my diaphragm, and my glutes that no amount of electrolytes could relieve.
I discontinued Ozempic at three weeks. Of course, my Dawn Phenom came back – with a vengeance of around 250 for a month or two- but now back to the 220’s, but to my dismay, my afternoon lows HAVE NOT RETURNED to previous. I am still running in the 150’s despite eating very low carb. I wonder if there was some microbiome effect due to slowing of gut motility that could explain this change. I had a similar blood sugar experience with lactulose after doing a breath test for SIBO.
Thanks for sharing your experience. We have an article on Dawn Phenomenon here that may be of interest: https://optimisingnutrition.com/dawn-phenomenon/
Chlorophyll is a natural GLP-1 receptor agonist. Here is a paper that talks about the possible mechanisms involved.
https://www.thieme-connect.com/products/ejournals/pdf/10.1055/s-0042-108340.pdf
This what the concept of ‘glycemic index’ was originally based on.
Interesting. I wasn’t aware of that. It might be part of the reason that we see such a massive satiety response to foods that contain more potassium.
I just started this last month taking Mounjora and the effects have been profound. I have been low carb keto for 6+ years and tried to optimize my diet according to nutrition. Since my metabolism has derailed into my 40’s and 50’s it’s been extremely difficult to lose weight. I was able to lose 80+ lbs with 5 day fasting with a 2 or 3 day refeed keto diet. I thought I could slowly lose weight down to my goal with just keto and I gained it all back and then some eating nutritionally rich keto. My appetite would not stop! Fasting has become increasingly hard as it affects my mood and head quickly. I want to stay on Mounjaro until I hit my goal weight but I am very interested in a diet plan designed for use with this drug and after drug diet plan. Since I was not exercising regularly I kept that as a control during this first initial month. My doctor appointment and weigh in is tomorrow but I have lost like 40 lbs! I know most is always water at the start but it’s significant! Typically I have eaten 1 or 2 small eating windows after extending my IF as long as possible with black cold brew coffee that I am really enjoying. Thanks Marty for such a thought provoking article. If you can help with these diet plans sign me up! Of course I want to get back to strength training, swimming and cycling soon.
Marty – do people with Type 1 diabetes have an abnormal GLP-1 level, given they don’t have an insulin response? Basically are they lacking in this hormone endogenously?
No. People with T1D, as far as I know from my research and living with two of them, have normal glucagon and GLP-1 function. It’s the imbalance of glucagon and insulin that causes elevated BGs.
Before my son was diagnosed, he was eating a TON, but I understand this is because the glucose was passing right through him without getting into his cells, so he had MASSIVE carb cravings. Once he started insulin this rapidly settled down.
Great article! I’ve watched a friend enjoy huge weight loss on Ozempic but now is gaining back. During the weight loss period she didn’t change what she ate, just the quantities. It looks like full circle.
Satiety is the magic. I can’t contribute to the conversation with regard to taking meds because fortunately I don’t have medical issues to address. However, satiety….finding the balance is key and makes the difference for me. High-ish protein and almost matching carbs produces a satiety response almost immediately. Using your programs is a game changer. Thanks for your amazing work.
thanks Jenny! drugs, or no drugs, satiety and nutrient density are critical. it must be frustrating for people when they spend all the money and then start gaining back due to poor nutrition.
From everything I’ve read on the ketogenic diet and diabetes T2 the goal is to lower your endogenous insulin as much as possible (and to get taken off your exogenous insulin by your physician).
It sounds like Ozempic INCREASES your endogenous insulin to promote satiety—the opposite of the goal. How does that help your diabetes?
(I am type 2, and have lost 45 lbs on a ketogenic WOE in 8 months, but have recently stalled, with 45 more to go; I was taken off insulin last August and remain on metformin and Victoza. )
The fact that GLP-1 antagonists work by increasing your insulin response to food doesn’t gel well with the carb-insulin model.
The key is that they help reduce your appetite, which leads to a loss in body weight and basal insulin, so your overall insulin demand on your pancreas will be reduced.
However you do it, it’s critical to focus on what you’re eating to make sure you feed the muscle and burn the body fat.