Embark on an enlightening exploration of two prominent dietary approaches – vegan and keto, for managing diabetes and enhancing blood sugar control.
This article meticulously analyses the pros and cons of each diet based on scientific evidence and real-world testimonials. As diabetes continues to be a global health concern, the quest for an optimal diet remains a significant discussion.
Delve into an engaging comparison, learn from mastering diabetes reviews, and understand the impact of keto and plant-based diets on insulin resistance.
Your pathway towards a well-informed dietary choice for diabetes management unfolds here.
- Background
- What’s actually wrong with the keto diet for diabetes?
- High-fat diet nutrient deficiencies
- What is the actual relationship between insulin and the food we eat?
- How to improve your insulin sensitivity
- Tight blood sugar control isn’t that important after all?
- Understanding physiological insulin resistance
- Does eating fat makes you fat?
- Complications on a ketogenic diet
- Is a low-carb diet good for diabetes?
- What should you eat if you are a vegan with diabetes?
- So which approach is optimal?
- Summary
- How Can I Calculate My Nutrient Intake?
- More
Background
I recently watched the Mastering Diabetes teleseminar on ketogenic diets with high hopes of picking up some gems of wisdom from the rising stars of the plant-based diabetes community.
Unfortunately, I was underwhelmed by what I heard.
I shared my frustration on Facebook.
Robb Wolf suggested I put together a response to some of the misinformation in the teleseminar. Hence this post.
What’s actually wrong with the keto diet for diabetes?
Cyrus Khambatta (aka Mangoman) and Robby Barbaro (The Mindful Diabetic) should be uniquely qualified, both academically and experientially having themselves lived with type 1 diabetes for decades.
If I were was going to attack keto for diabetes management, then there would have been a couple of ‘free kicks’ I think they could have taken. So, in fairness to both sides, I’ll touch on a few of what I see as legitimate issues with ‘popular keto’ before I dissect the Mastering Diabetes presentation.
Giving fat a free pass
Humans like things to be straightforward and binary.
Yes or No.
Black or white.
High fat or low fat.
Low carb or high fat.
High protein or low protein.
Plants only or animals only.
For the last four decades, we have been told that fat, particularly saturated fat, is bad because it causes heart diseases and should be avoided.
The tide is now turning. However, there will always be people who take things to the extreme.
Now fat is healthy. But is more is better?
Ketones are good. So more is better?
For many people, a higher fat diet will be more satiating, particularly compared to processed grains and sugars. However, not everyone can ‘eat fat to satiety’ without some level of restraint and self-discipline. We can’t all trust our appetite to kick in to effortlessly provide the lean and chiselled body that they dream of.
My personal experience is that you can overdo the fat and drive insulin resistance by pushing fat too hard. If you exceed your ‘personal fat threshold‘[1], your adipose tissues will become insulin resistant, and the body will start pushing excess energy to the vital organs.
While there is no need to fear fat, there is no reason to go hog wild to compensate for the butter and bacon deficiencies that we all developed over the past four decades.
When it comes to nutrition, you need to get your big rocks in place first (i.e. the nutrient-dense foods). You can then fill up with fuel such as fattier foods if you do not want to burn any body fat. You could even add some starchy carbs if your blood sugars allow it.
Having some level of ketones indicates that your insulin levels aren’t too high and your metabolism is working. However, if you are not yet metabolically healthy, chasing ‘fauxtosis‘ by loading up on butter, coconut oil, cream and exogenous ketones to achieve high blood ketone levels can be a recipe for hypercaloric metabolic disaster that will drive insulin resistance.
People with type 1 diabetes (such as the Mastering Diabetes guys and my wife Monica) have a unique insight into the various factors that affect their insulin sensitivity. They can monitor their daily insulin dose.
I know some people with type 1 diabetes who have made an effort to chase higher ketones with more refined fat and less protein but found that they ended up needing more insulin. Retreating to a moderate to high protein approach with less added fat (as per Dr Bernstein’s recommended approach for Type 1 diabetes) enabled them to improve their insulin sensitivity (e.g. check out Allison’s Nutrient Optimiser analysis here).
This phenomenon is not unique to people with type 1 diabetes. There seem to be more and more people start out believing calories don’t count, only hormones. They then put their faith in the ‘magic ketone fairy’ and end up driving insulin resistance and obesity chasing ‘optimal ketone levels’ with more and more added fat.[2]
I have a dream
Before we get into the nutritional analysis, permit me this indulgence to share my vision (with a hat tip to Martin Luther King) from Martin Laurence Kendall.
I have a dream that one-day nutrition will be defined by the nutrients that a food contains and the health benefits that it confers rather than religious and ethical beliefs or commercial interests.
I have a dream that all people, mothers and children, fathers and brothers, would be able to clearly understand the foods that are truly optimal for them.
I have a dream that one day all people afflicted with diabetes will be able to choose foods that will enable them to achieve normal blood sugars and restore the health and vitality that they deserve.
Further, that they will be able to choose optimal foods, with engineering precision, without being affiliated with the needless ridicule that they will needlessly die of a heart attack due to unnecessary fears about ‘artery-clogging saturated fat’ or ‘harmful animal proteins’.
I have a dream that one day people will have, freely in their grasp, quality nutritional information that enables them to make informed choices that will, in turn, bring about a new day in the commercial food environment.
I dream that one day all people, obese, diabetic, children and athletes alike, will be free from the corruption of Big Food and Big Pharma working through diabetes educators, diabetes associations, heart associations, medical institutions and animal welfare advocates.
Free at least. Free at last.
I hope that one day we will be free at last.
Indulgence over. On with the data.
On with the data.
High-fat diet nutrient deficiencies
Another fact that I thought Cyrus and Robby would mention was that very high-fat foods tend to have a weak nutrient profile, especially compared to non-starchy vegetables.
The chart below shows the nutrients provided by the 800 highest fat foods out of the 8000 foods in the USDA database. If we prioritise fat, we will likely be lacking in around half of the essential nutrients.

A summary of some of the highest fat foods is shown below.
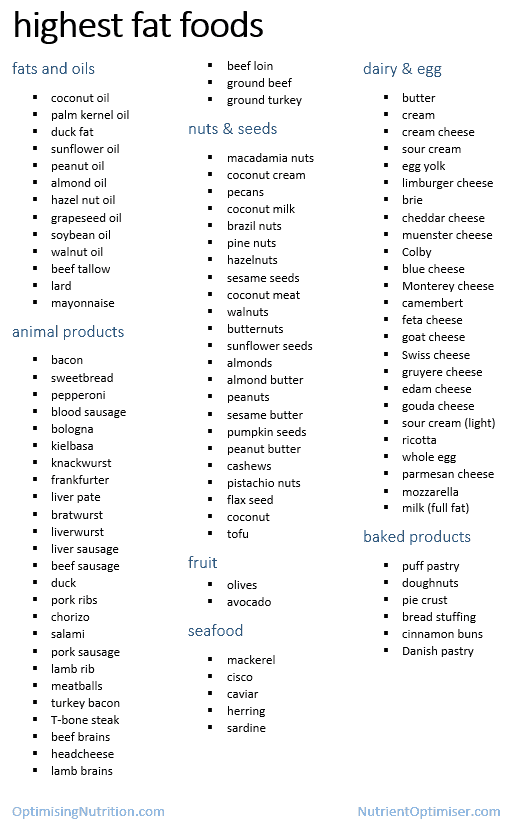

[For some real-life examples of the poor nutrient profiles achieved by people chasing high ketone levels in the misguided pursuit of weight loss check out the Nutrient Optimiser reports here, here, here here and here.]
Vitamins and minerals, in particularly electrolytes such as potassium, magnesium and calcium are critical to support our mitochondria, enabling them to produce energy and maximise insulin sensitivity.
People in the keto community are conscious that electrolytes are essential and go out of their way to supplement with magnesium, calcium, sodium and potassium as well as taking bone broth.
The kidneys let go of water and electrolytes when insulin levels drop. A ketogenic diet without attention to green leafy veggies is at risk of being very low in electrolytes. This will cause the pancreas to secrete more insulin to hold onto the scarce electrolytes. This increase in insulin levels may[3] ironically drive insulin resistance.
Whether you call them electrolytes or alkaline foods[5], our bodies need enough substrate to allow our kidneys to maintain a good acid/base balance without having to work too hard. Focusing on minerals can helps us maximise insulin sensitivity and ensure oxygen is efficiently be carried around our bloodstream.
There are plenty of foods available to provide the micronutrients that you need if you actually require therapeutic ketosis as an adjunct to cancer, epilepsy or dementia. We can achieve the Daily Recommended Intake (DRI) for most of the nutrients while still maintaining a low dietary insulin load.
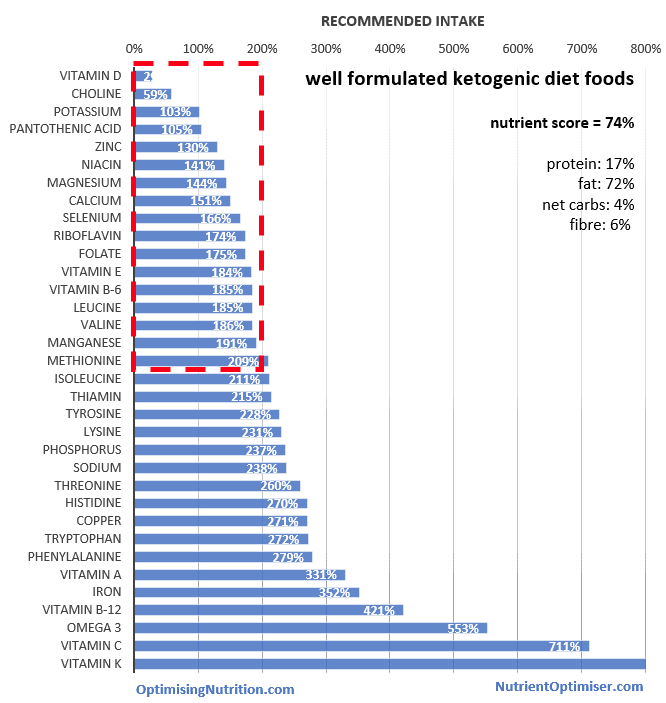
However, if you just need to manage diabetes with a low-carb diet (rather than therapeutic ketosis), you can achieve even higher levels of nutrition while maintaining stable blood sugars.
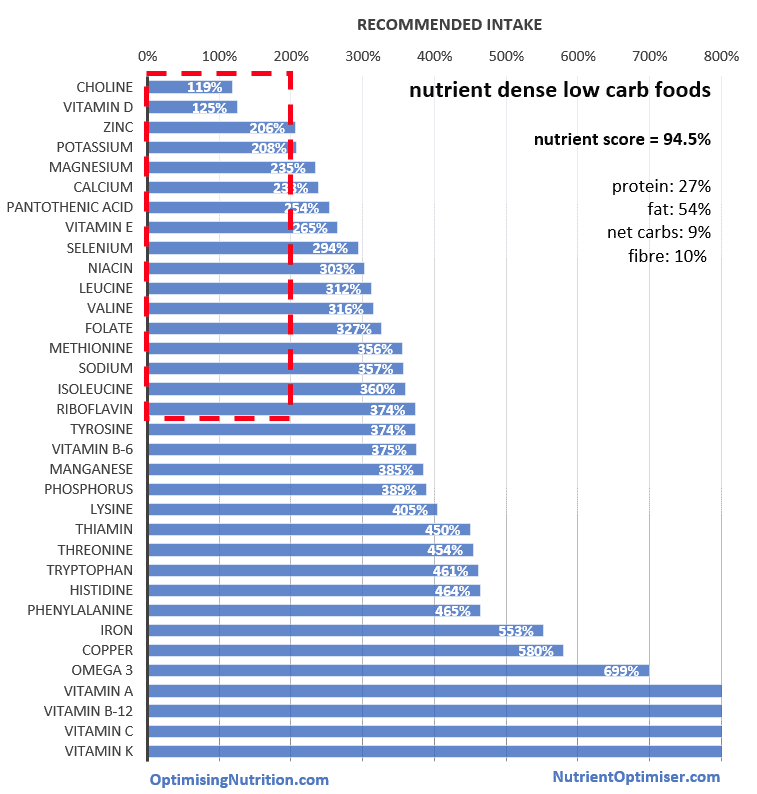
Given my family history of Type 2 and my wife Monica’s Type 1 diabetes, we generally focus on the foods listed below. Lots of people have found these lists useful. You can pin them to the fridge as a reminder of what you should focus on or print it out to take shopping next time when you need some inspiration. (There is a complete list of nutrient dense foods to suit different goals at the end of this article.)
Now my blood glucose levels are more stable, I’ve been trying to back off on the higher fat foods and focus on more nutrient-dense foods to build muscle and lose fat.
The ‘problem’ with the most nutrient-dense foods is that they typically have a very low energy density so it will be nearly impossible to get enough energy to prevent rapid weight loss.
Prioritising nutrient-dense foods is the secret to obtaining the nutrients you need with the lowest energy intake. If you don’t want to keep losing weight or want to run a marathon then adding some higher energy density foods will be useful.
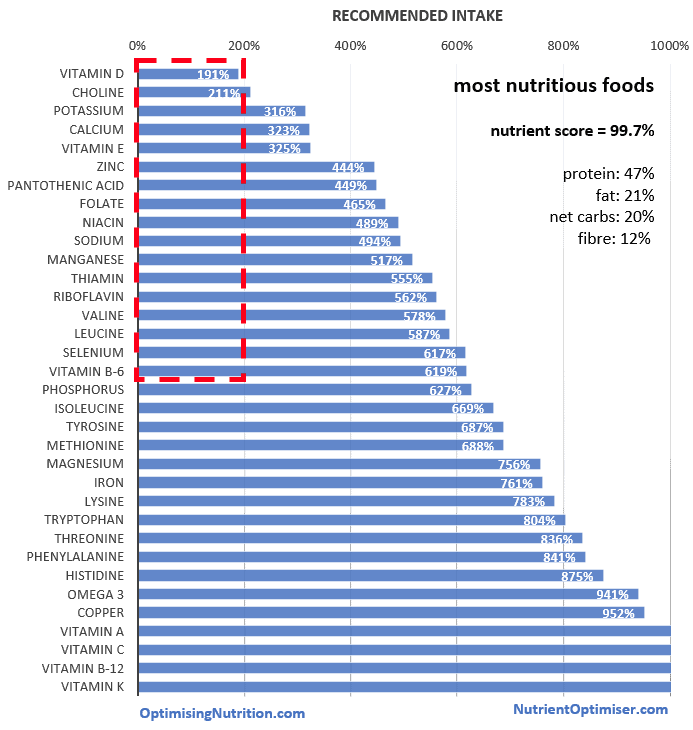
High carbohydrate foods are not nutritious
After watching the Mastering Diabetes teleseminar, you will get the feeling that the Mastering Diabetes guys believe carbohydrate can do no wrong and we should only fear fat.
The reality, however, is that the foods with the least fat are generally even more nutritionally corrupt than the highest fat foods.
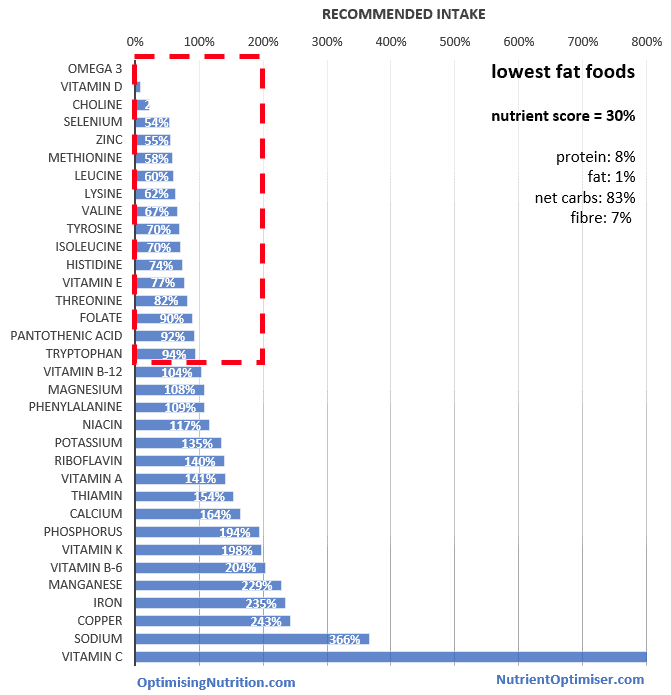
Not all of the low-fat foods are going to be beneficial.
Defining your nutritional approach as ‘high carbohydrate’ is not wise, especially if you are trying to manage diabetes. The foods with the most carbohydrates in our food system are typically very nutritionally deficient as well as highly insulinogenic.

If a ‘low carb diet’ leads you to avoid processed foods you may be better off. However, I don’t think defining nutrition in terms of macronutrient extremes is particularly useful. [6]
Plant-based versus animal-based foods
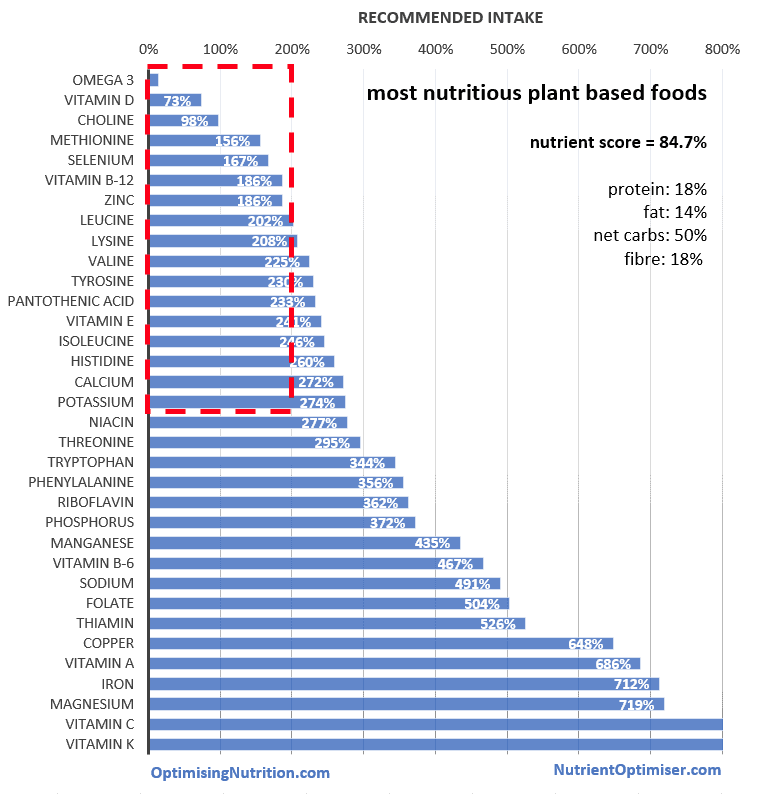
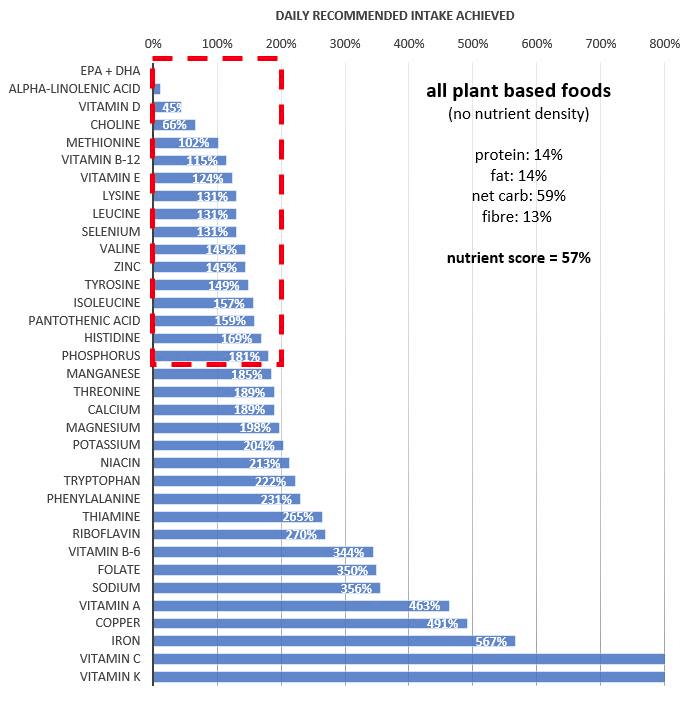
One area where vegans potentially have it over carnivores is vitamins and minerals. As shown in the chart below, a zero carb diet does not provide really high levels of many nutrients.
![2017-06-26-5[1]](https://optimisingnutrition.com/wp-content/uploads/2017/07/2017-06-26-51.png)
At the same time, there are plenty of people who appear to be thriving on a zero carb dietary approach. Many people with severe autoimmune related digestive issues succeed when they switch to a zero carb approach. Zero carb advocates will also tell you that they don’t need the recommended daily intake levels of the various micronutrients that are based on limited data or deficiency studies in people eating a standard high carb western diet.
A plant-based diet can provide a reasonably nutrient dense outcome. However, it will be hard to get adequate levels of omega 3, vitamin D and vitamin B-12. People following a strictly plant-based approach may need to supplement with these nutrients.
Achieving the minimum protein intake levels is possible. However, many people have concerns about the reduced bioavailability of plant based proteins and whether or not the minimum protein intake levels are actually optimal, particularly if you are active or older.
It’s also worth noting that other nutrients such as iron, vitamin A and omega 3 will be more bioavailable from animal-based sources. So it’s not as simple as comparing the nutrients in the food, what gets into your body is what really matters.
If you are going to follow a plant-based diet then prioritising the food listed below will give you the best chance of success. Most people are going to do best somewhere on the spectrum between exclusively plant-based and solely animal-based foods.
The real problem comes when we start to heavily process our food. Rather than prioritising the most nutrient dense and minimally processed vegetables, fruits and legumes, many vegans end up living on processed grains, cereal, sugar and soy products that have been treated with a host of fertilisers and pesticides. Meanwhile, many zero carbers or keto peeps end up living on nothing but bacon or processed meats from animals that were fed nutrient poor corn and grains with added antibiotics to make them grow quicker.
The vegan echo chamber
I have spent a good chunk of time hanging out in many vegan or plant-based groups trying to understand their position and gain insights about nutrient density. I have learned a lot from people like Professor Christopher Gardner, Ray Cronise and Dr Joel Fuhrman. Much of the analysis in this is based on the integration of my learnings their work with Dr Richard Bernstein and Dr Matt Lalonde.
Unfortunately, it seems that the vast majority of vegan/plant-based education comes from Dr Michael Greger through his sanitised, highly processed and hyper-palatable “Nutrition Facts” videos.
While Greger covers a lot of relevant research and raises some valid points, a lot of the time he seems to twist the science to ensure that the moral of the story is always ‘eat plants, not animals’. Plant-based is better. Eating animals will be bad for your health.
Without evolutionary context, we are asked again and again to believe that fat (particularly saturated fat) and ‘animal protein’ (whatever the hell that is!) is the primary cause of heart disease, the complications of diabetes and practically every other modern health ill.
There is no demonstrated biochemical mechanism provided as to how we suddenly became allergic to animal products. Meanwhile, vegans advocates generally give a free pass to sugar and processed grains.
With more than six million views and an estimated earnings of more than $100k per year from YouTube[7] (not to mention donations[8]), there appear to be a LOT of people eager to lap up the nutritional and medical justification of their ethical position.
Greger’s unique ‘interpretation’ of the scientific data all starts to make sense once you understand that he is the Director for Public Health and Human Agriculture for the Humane Society International.[9]
The mission of the Humane Society is to celebrate animals, confront cruelty and shape public opinion.
I wonder if Greger does his researching, writing, filming and editing the Nutrition Facts videos as a hobby after he gets home after working 50 hours a week and commuting? Or perhaps he creates these videos as an employee of the Humane Society as part of their stated goal to shape public opinion on animal cruelty?
It seems Mangoman and Robby are pretty tight with Greger.[10] Makes me wonder if Mastering Diabetes is a coordinated and strategic assault by the Humane Society on the low carb/keto/diabetes community who have become immune to Dr Greger.
I am by no means advocating animal cruelty. However, as a human, if you are looking for the best advice on human nutrition, is it wise to put your blind faith and unswerving trust in someone whose explicitly stated primary goal is animal welfare?
Do you really want to save the planet?
Worrying about whether we eat plants or animals exclusively is a modern luxury, an intellectual indulgence of sorts.
For the majority of human history, we have been opportunistic omnivores. When plants were the only thing that was available, we would eat them. When we could, we would chase down an animal to get the protein we need to thrive. We never had to worry about nutrient density because the foods we ate grew in fertile soil without pesticides. The animals we ate were eating their natural foods which were also nutritious for them.
Humans thrived and were able to populate the world because we learned to hunt, store, cook and process food. We became very good at getting the nutrients we needed with the minimum amount of effort.[11][12] [13]
Unfortunately, we have now become too good at processing food.
Many of us are now fantasising nostalgically about Paleo times.
It’s one thing to worry about saving animals, but ultimately we need to save the planet and our human race from accelerated extinction.
Our newfound ability to harvest fossil fuels enables us to move around in cars and grow a massive amount of food with chemical fertilisers. These foods grow quickly and give us plenty of energy, but few nutrients that we then process and feed to animals or humans.[14]
Take a moment to think about how your life would be different if we had never discovered fossil fuels (e.g. coal or oil). For as long as it lasts we are gorging ourselves on stored energy that is making us lazy and obese and driving not just us, but life as we know it to an early grave. If you want to care about something it should be the sustainability of the global environment (including animals and humans).
If you want to care about something it should be the sustainability of the global environment (including animals and humans).
While humans are probably the biggest threat to the long-term sustainability of earth as we know it, most of us aren’t willing to volunteer ourselves or our family as the first ones to check out to save the planet.
[If you want some challenging thoughts on this topic you should check out Daniel Vitalis’ Why I Hunt podcast.]
The plural of anecdote is not data
So, finally, onto the Mastering Diabetes video.
Cyrus and Robbie look like genuinely nice guys.
They are both living with type 1 diabetes.
They look like they’re happy and thriving on a plant-based diet full of fruits and vegetables.
To be honest, they look a lot healthier than many recovering diabetics in the low-carb scene.
But at the same time, the zero carbers will hold up anecdotes of people who have not eaten a plant for decades and look as great as the Johnson Family.
Or Dr Shawn Baker who is setting world records as a masters athlete since cutting plants out of his diet.
Then the keto folks will point to Dr Dominic D’Agostino who thrives on high fat and exogenous ketones and is exceptionally smart and can lift very heavy stuff at the same time.
While it’s useful to look at populations of people following a particular diet to look for trends, anecdote does not equal data.
It is more useful to look at underlying metrics (such as nutrient density and insulin load) that we can use to identify the optimal diet for humans.
I thought they would know better
Cyrus Khambatta is a smart guy. He was studying mechanical engineering at Stanford before he got type 1 and changed course to study nutritional biochemistry.
However, for all his ability in nutrition, engineering and mathematics (I took those classes, and I know how hard they are!), I thought he would have more to offer than what was presented!
People with diabetes get screwed around by the mainstream medical system and ‘diabetes education’ system. The system doesn’t really understand how it works, so they give them bad advice (e.g. “just eat like we tell everyone else to and cover it with insulin”)!
I remember clearly the anxiety and confusion we experienced after going to an appointment with the hospital endocrinologist when my wife Monica was pregnant with our daughter.
At her visits, she would routinely be told that she needed to reduce her blood sugars to avoid the many serious risks and complications and risks for her and the baby. Monica asked what else she could do to get the blood sugars down, but they had no advice. They just wanted to see them lower.
We now have two healthy and wonderful kids, but I if I can I would love to see other people spared the anxiety as well as minimise the genuine health risks related to diabetes. Hence my quest to understand how we can make intelligent food choices to optimise blood sugar and insulin levels.
What is the actual relationship between insulin and the food we eat?
The food insulin index data is a highly valuable resource that helps us to understand what causes us to secrete insulin and our blood sugars to rise. The chart below shows the results of the food insulin index testing on more than 100 different foods (click to enlarge).

The food insulin index testing demonstrates clearly that we have the lowest insulin response to fats and oils while we have the highest insulin response to high carbohydrate foods like jelly beans and rice bubbles. However, when we plot this data, we see that carbohydrate does not fully explain our insulin response.
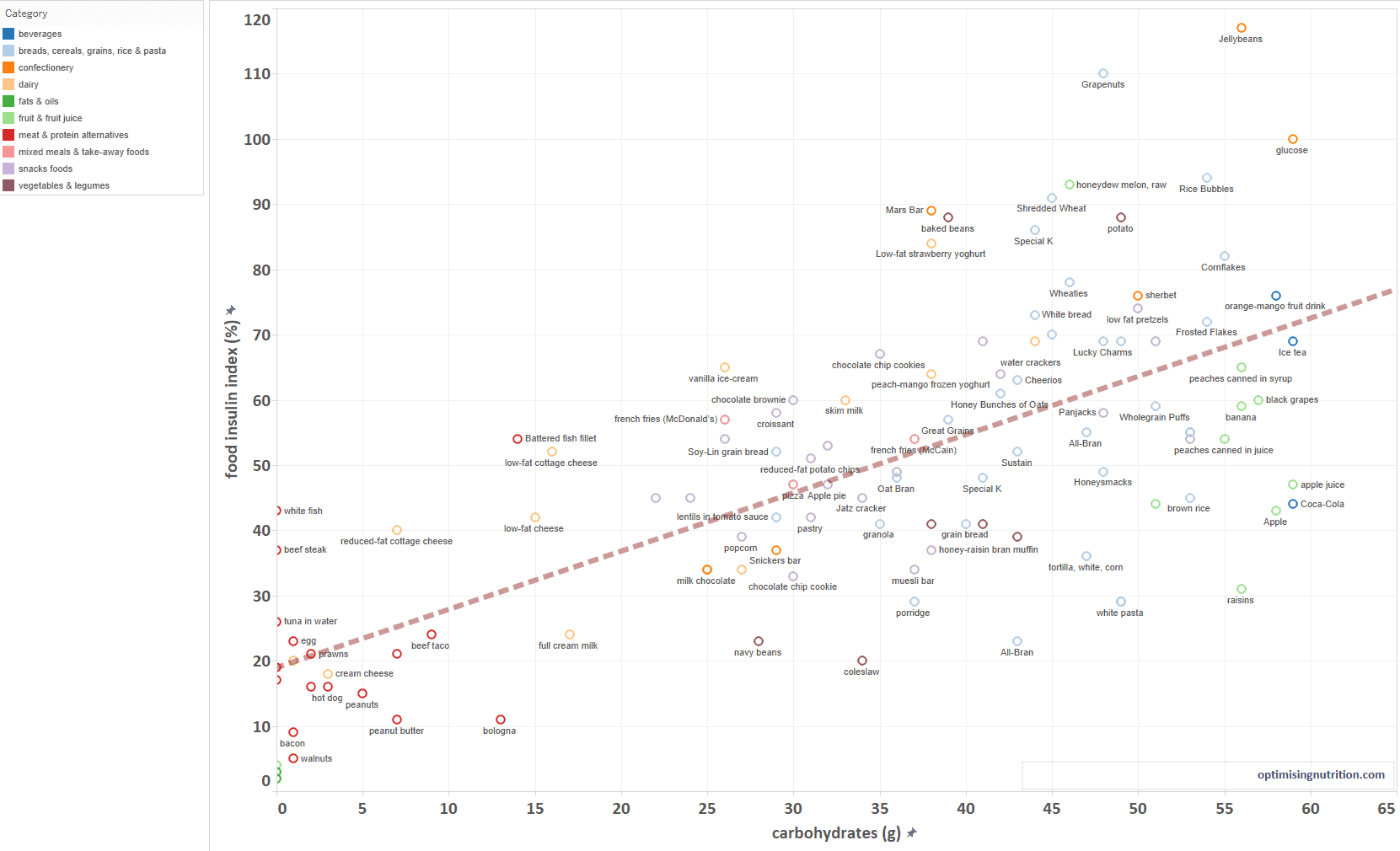
We get a much better prediction of our insulin response when we account for protein (which requires insulin to metabolise) and non-digestible fibre.

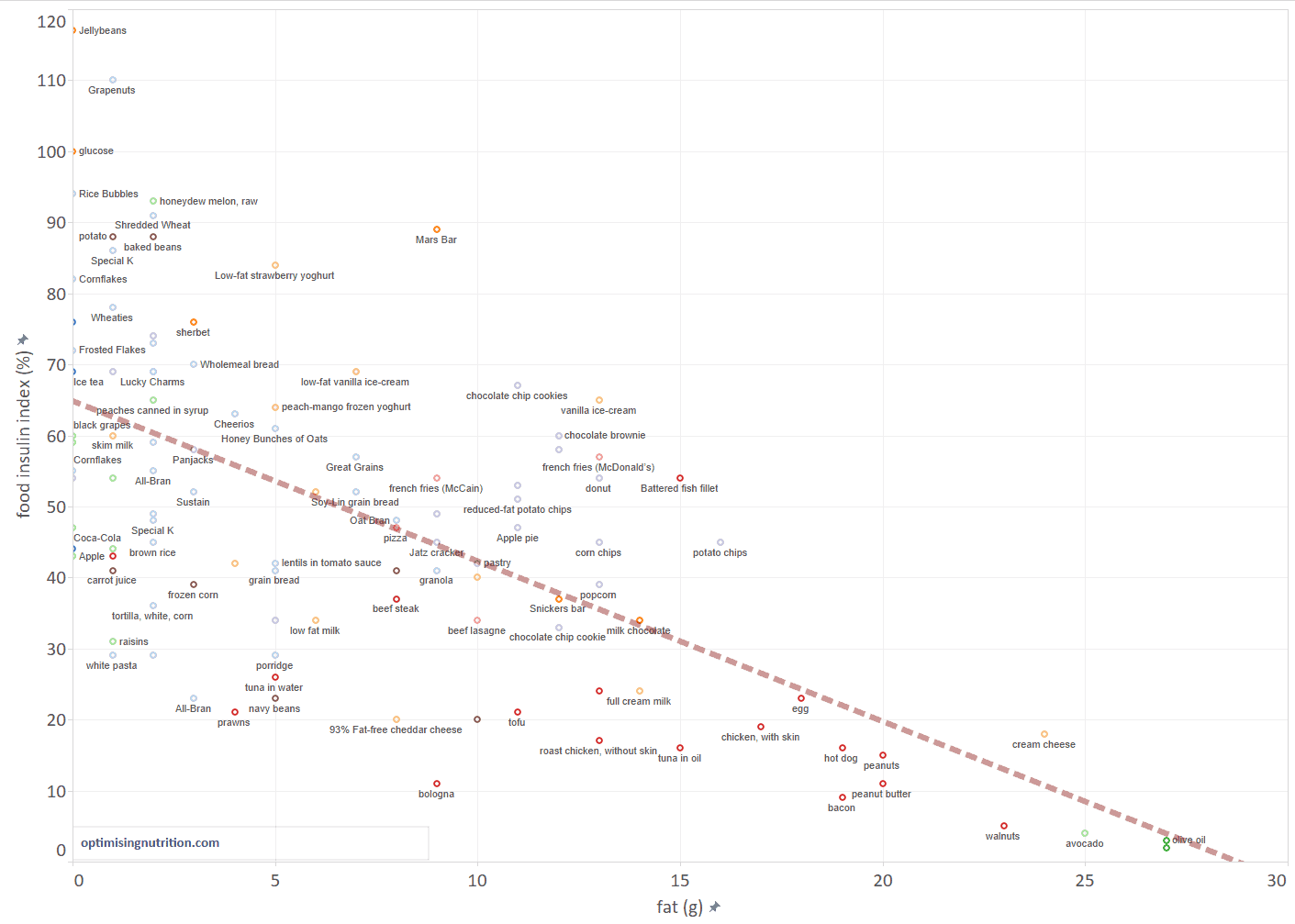
Eating more fat will decrease the amount of insulin required to keep our blood sugars stable.
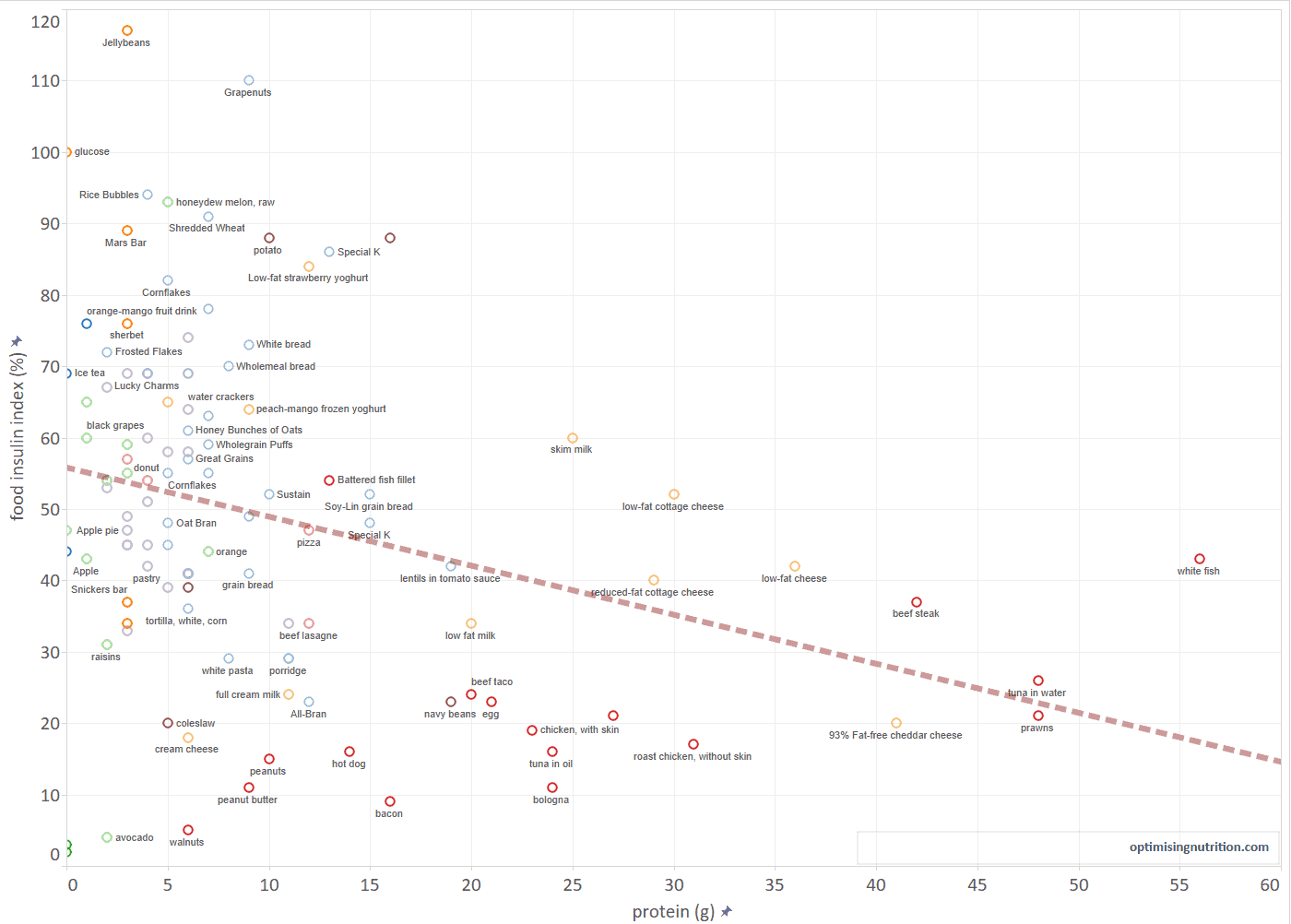
Eating more protein will reduce the amount of insulin your pancreas has to produce because it will push the more insulinogenic processed carbohydrates and sugar out of your diet.
How to improve your insulin sensitivity
If you reduce your intake of processed carbs and sugars, your insulin requirements will come down. Once your organs and muscles are no longer swimming in insulin, you will become more insulin sensitive (just like you become more sensitive to coffee or alcohol if you cut back your intake).
If you are injecting insulin, reducing the insulin load of your diet will enable you to significantly reduce your insulin dosage which will, in turn, allow you to more easily access your own body fat stores for fuel.[16]
This data is an inconvenient truth for both high carb vegans or the nutritional recommendations such Food Pyramid / My Plate generated by the US Dept of Agriculture. But I think it could be beneficial for people who want to effectively manage their diabetes.
Granted, if you switch your processed grains and sugar for fruits and vegetables, you will do better. But is it really optimal?
If you can’t win, move the goalposts!!!!
So what do you do if you can’t win with science?
You change the rules! You move the goalposts.
It was Cyrus and Robby’s unique definition of insulin resistance that really frustrated me.
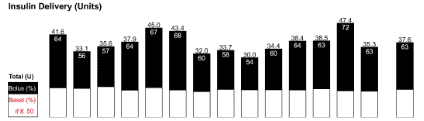
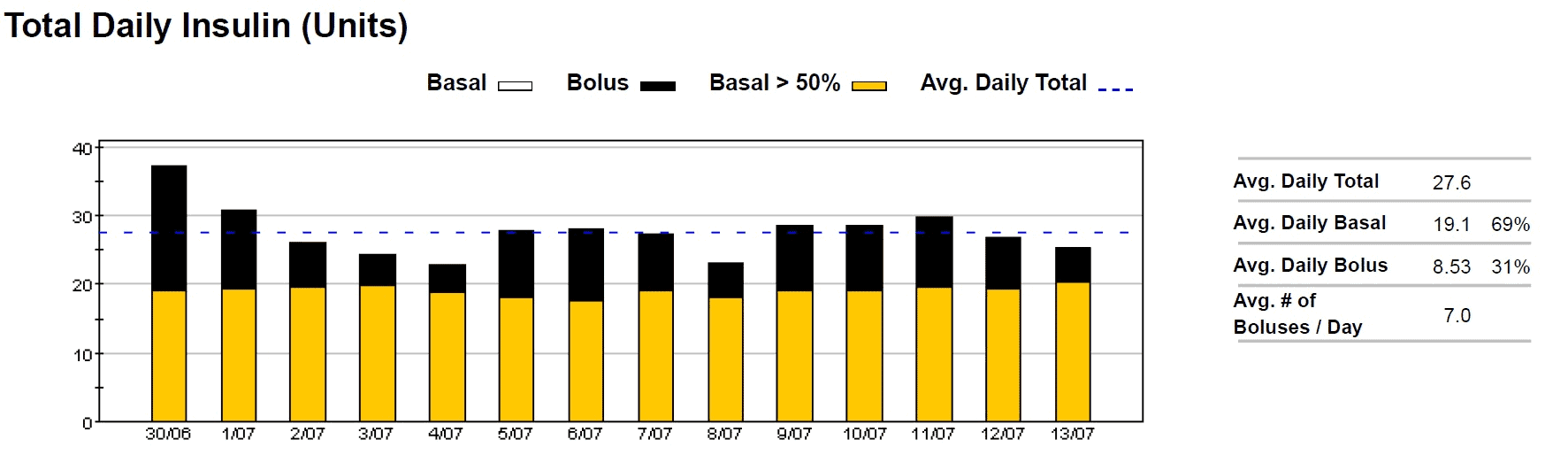
So you can understand my frustration, I need to explain the difference between basal and bolus insulin which is a daily reality for someone with type 1 diabetes.
- Bolus insulin is taken with food and is proportional to the insulin load of the food they eat (i.e. carbs – fibre + half protein)[17].
- Basal insulin is the insulin that your pancreas would produce through the day and night whether or not you eat anything. It’s the basal insulin that keeps your fat in storage and your muscles from being used for fuel.
You need both, but their function is different.
For someone eating a standard western diet about one-third to a half of their insulin will be basal insulin with the majority being bolus insulin for the food you eat.
When you switch to a low carb or keto diet this ratio flips and the majority of your insulin is basal insulin. You only need a little bit of bolus insulin to cover the small amount of carbohydrates and protein that you eat. With less glucose to deal with, you don’t need as much insulin, and your blood sugars stabilise.[18]
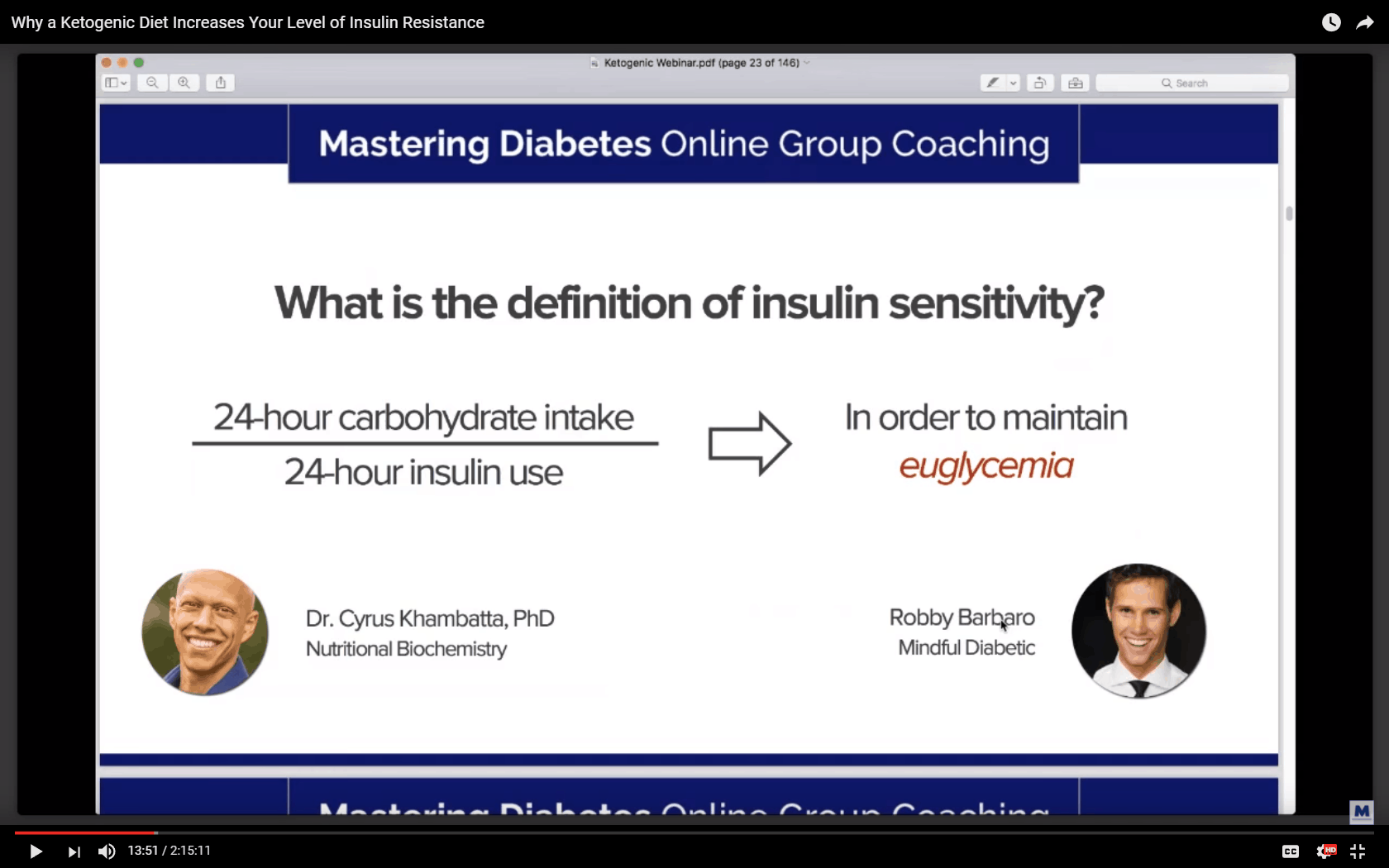
A significant portion of the Mastering Diabetes video was devoted to explaining their new creative definition of insulin sensitivity. The fundamental problem with this central piece of the Mastering Diabetes argument is that it conflates basal and bolus insulin. Your basal insulin is irrelevant if you are trying to do this sort of insulin sensitivity calculation!
It’s just the bolus insulin (i.e. for food) that matters when it comes to insulin sensitivity. The calculations in the table below demonstrate my point. If you take the denominator to your insulin sensitivity calculations to be the basal + bolus insulin, then the high carb approach has a better insulin sensitivity. If you only consider the bolus insulin (the only sensible approach in my view), then you declare the low-carb approach to be the winner.
| low carb | high carb | conclusion | |
| ISF (g carb/unit insulin) | 6 | 5 | |
| carbs (g) | 50 | 500 | |
| bolus insulin (units) | 8.3 | 100 | |
| basal insulin (units) | 20 | 20 | |
| total daily insulin (per day) | 28 | 120 | |
| 24 carb / 24-hour insulin (basal + bolus) | 1.8 | 4.2 | High carb is better |
| 24 carb / 24-hour insulin (bolus only) | 6.0 | 5.0 | Low carb is better |
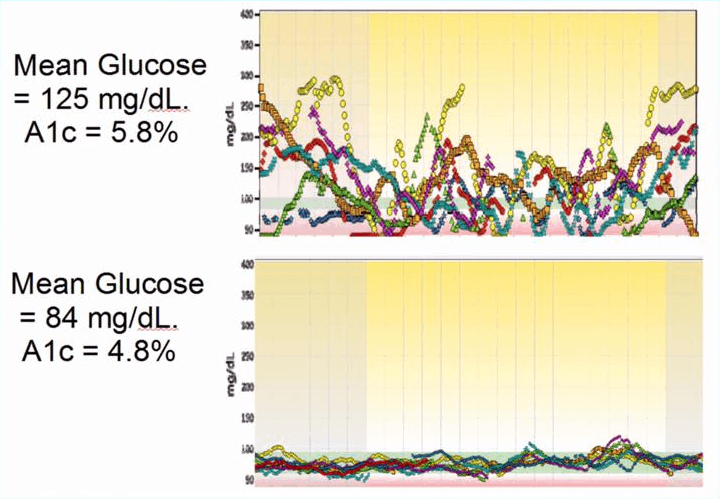
The chart below shows the difference in the daily blood sugar fluctuations of someone on a standard western diet and then after switching to a lower carb diet. The difference in the blood sugar levels is night and day! The difference in the quality of life between these two situations when it comes to energy levels, anxiety, depression, mood etc. is also immensely different.
I pinged Mastering Diabetes on their Facebook page to clarify if the cornerstone of their whole argument includes basal and bolus insulin. Unfortunately, my fears were confirmed (though they have since deleted their response and kicked me out of their Facebook Group).
Tight blood sugar control isn’t that important after all?
The next argument they try to run is that tight blood sugars really aren’t that necessary.
Cyrus (who is very active and practices intermittent fasting) has a Hba1c in the high 5s.
Robbie has a Hb1c in the low 6s.
Granted, this is good compared to the majority of the Type 1 population. They’ll have a better chance of thriving with good blood sugars if they are eating lots of vegetables and fruit compared to more processed grains and sugars that make up the typical diet. But it’s still a far cry from the blood sugar control of people following the type of low-carb approach advocated by Dr Richard Bernstein.
The problem I see with defining your diet as vegan or plant-based is that most people don’t have the self-discipline to stick with eating only vegetables and fruit and end up filling up on more processed (but still technically vegan) processed junk food.
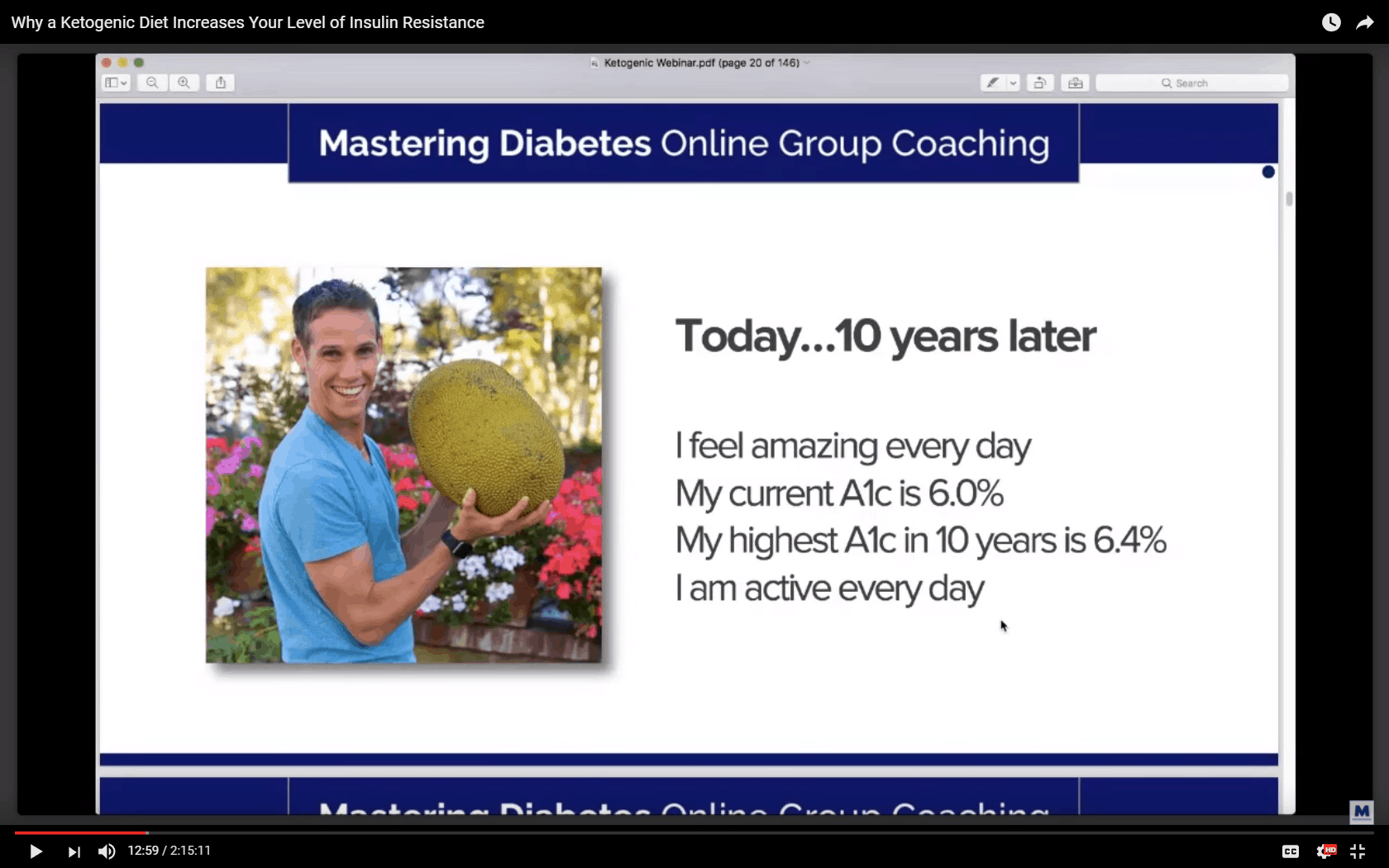
Cyrus and Robbie argue that normal blood glucose fluctuations are between 70mg/dL to 145 mg/dL or 3.8 to 8.0mmol/L.
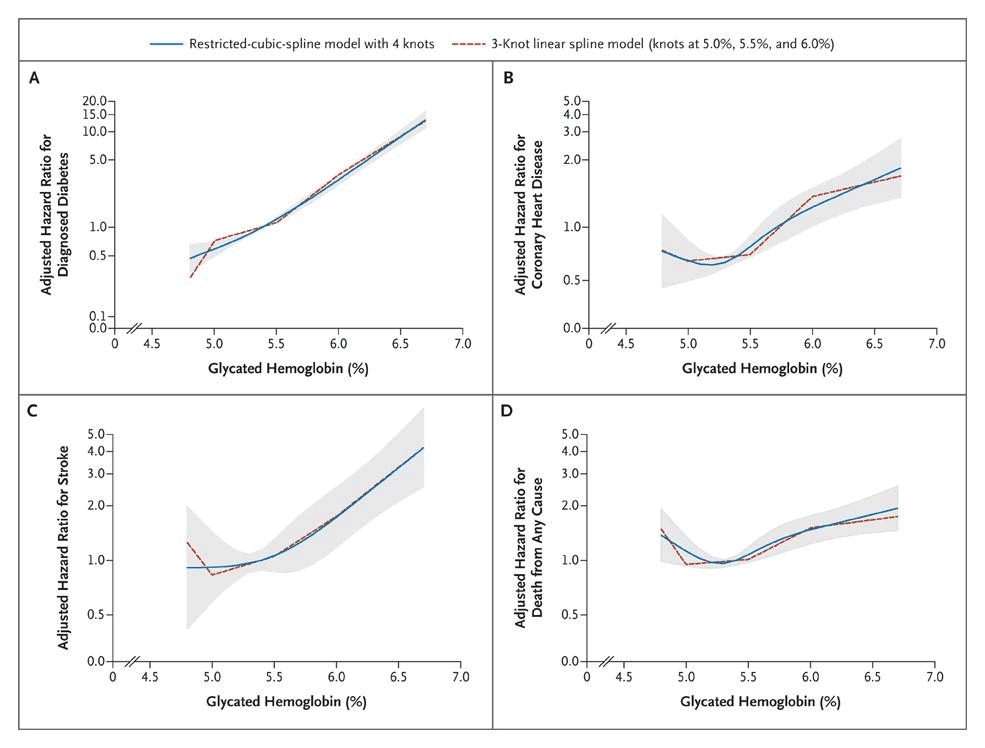
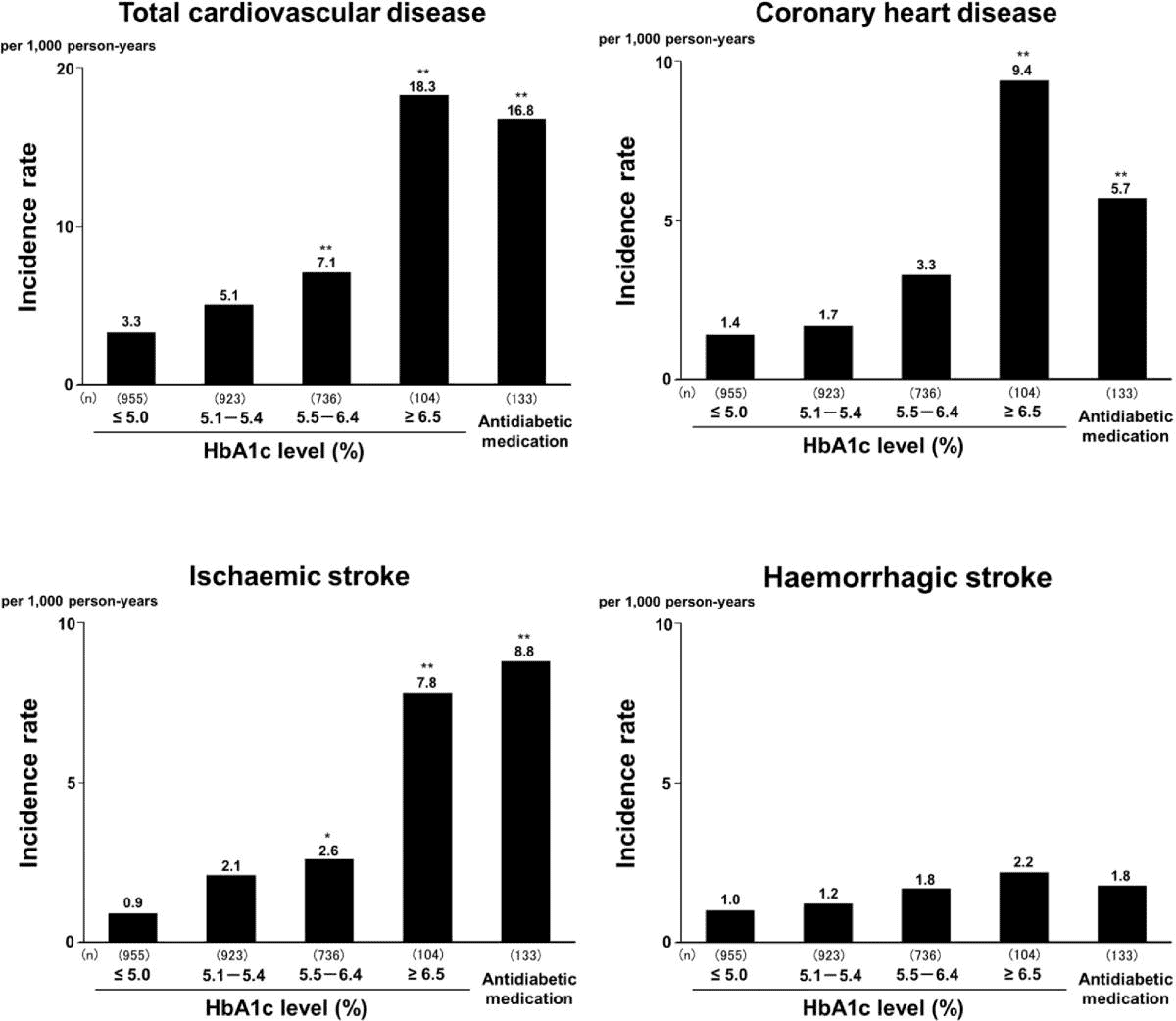
The problem with this argument is that what currently passes for ‘normal’ is far from optimal.[19] Complications from diabetes start to kick in well below what is widely considered “normal”.
Just because it’s normal for most people to do Facebook on their phone while they drive doesn’t mean it’s ideal or optimal. Just because it’s normal to have poor blood sugar and most people are dying of metabolic diseases doesn’t sound like a persuasive argument for a plant-based diet being optimal to me!
If you’re happy to settle for less than optimal blood sugar control because you have a strong ethical position, then that’s fine, but don’t construe it as optimal for everyone when it’s not.
The reality is that many people over at Type 1 Grit following Dr Bernstein’s approach are doing fabulously! Not everyone will achieve optimal, but it’s useful to know what to aim for and how to get there.
If you had a child or loved one with Type 1 diabetes would you want the opportunity to choose the approach that would yield the best results or would you prefer your advice to be tainted with ethical or commercial bias?
Check out the video the Type 1 Grit group put together for Dr B’s 83rd birthday to thank him for changing their lives.
Insulin resistance and metabolic syndrome are a big deal, so let’s not ruin more lives than we need to with bad advice that is based on bad math or putting ethical convictions or religious beliefs ahead of human health.
Understanding physiological insulin resistance
Cyrus and Robbie argue that someone on a low carb diet won’t deal with carbohydrate well when they are exposed to them. This phenomenon is real, but is typically due to what is termed ‘physiological insulin resistance‘.
Someone who eats a lot of carbohydrates will have high levels of insulin floating around in their bloodstream. Then when they eat a carb bolus, their pancreas is primed to shoot out some more insulin to mop up the glucose and stop more glucose being released into the bloodstream via the liver. By contrast, someone who doesn’t eat a lot of carbohydrates will have low levels of insulin in their bloodstream and need to wind up their pancreas to produce insulin to bring down the glucose.
This phenomenon is also referred to the first phase versus second insulin response. Someone who is not eating a lot of carbs will have a slower first phase insulin response.
It’s like comparing someone’s time over 100m when they are starting from a standstill versus someone using a rolling start. It’s not a relevant comparison. This phenomenon will go away after a few days on a high carb diet.
At the same time though, micronutrients such as potassium, magnesium and calcium are critical to maintaining healthy insulin sensitivity and glucose uptake. Metabolic acidosis (caused by a lack of dietary electrolytes) appears to cause an upregulation in insulin by the pancreas to hold onto precious electrolytes. Over the long term, this could be another driver of insulin resistance, metabolic syndrome and diabetes. [20]
Getting adequate dietary electrolytes from green leafy vegetables will make it easier for our body to maintain acid/base balance. However, I don’t think we need to feed all diabetics a high carbohydrate exclusively plant-based diet to achieve this.
Does eating fat makes you fat?
The vegan community seems to confuse eating fat and storing fat. The Ancel Keys / vegan story is that we store fat in our bodies because we overeat dietary fat. However, the reality is that we get fat because we eat more than we burn.
As shown in the graphic below from Ray Cronise’s Oxidative Priority paper, we will only burn fat (from our body or diet) once we’ve burned through the alcohol, ketones, protein and carbohydrate and fat that we eat (in that order).[21]
When we eat, our body prioritises refilling our glucose and glycogen stores in our bloodstream and liver (which can hold about 1200 to 2000 calories) before we start storing the excess energy in our adipose tissue. Our body fat stores can hold a lot more energy, but not an unlimited amount. Once our fat stores are full and can hold no more, they become insulin resistant. We then start to store the excess energy in our vital organs such as our liver, kidney, brain, eyes, heart, etc.
The trick to weight loss is to keep your blood sugar levels low enough so that your liver glycogen is being replenished from your body fat rather than always having overfull glycogen stores, so we need to offload excess energy to our fat stores.[22]
One of the many roles of insulin is to shut off the flow of stored energy from the liver into the bloodstream. If energy is coming in the pancreas will upregulate insulin to stop the flow of glucose from the liver back into the bloodstream (regardless of whether you’re eating carbs, fat or protein from animal or plant-based sources). The best way to reduce insulin is to stop eating and let your stored energy flow back into your bloodstream.
In a way, you can think of your liver as your fuel tank and you your blood glucose meter as the fuel gauge. If your blood sugars are high, you should think twice about whether you really need more fuel now.
If you are insulin sensitive, the bad news is that you can easily store excess energy as body fat very efficiently. Insulin is an anabolic hormone that will help you to grow. However, when you are insulin sensitive, you can lose fat relatively quickly when you reduce energy intake. If you are insulin sensitive your circulating insulin levels will be low, and fuel will more easily flow from storage. Hence you won’t be such a mindless slave to your uncontrollable appetite.
If you are insulin resistant and have high levels of circulating insulin, you may struggle to release your stored body fat. Your appetite will drive you to seek out food because you can’t efficiently access it from your body stores. You won’t be able to go very long between meals.
A low-carb diet can be helpful for someone who is insulin resistant because it can help lower insulin which in turn help them to normalise their appetite. Teaching that we get fat because we eat fat is just outdated science.
Even Dr Joel Fuhman will tell you that actively avoiding fat is stupid. He will also tell you that there is some value in eating fish on a regular basis to ensure you get adequate amounts of omega 3s and vitamin B-12.
Complications on a ketogenic diet
There are plenty of studies that show the shortcomings of a ketogenic diet. Sarah Ballantyne did a great job of summarising these on her Paleo Mom Blog here.
When you look in detail however you find that the adverse reactions the ketogenic diet are typically due to ‘keto in a can’ formula products.
While these food substitutes will help achieve therapeutic ketosis to help manage epilepsy or other chronic conditions, many of these keto formula products end up being very low in micronutrients.[23]
Obtaining a significant amount of your energy intake from processed food-like products that have been separated from nutrients is not a good idea (e.g. whether it be sugar, processed grains, refined oils or exogenous ketones).
Is a low-carb diet good for diabetes?
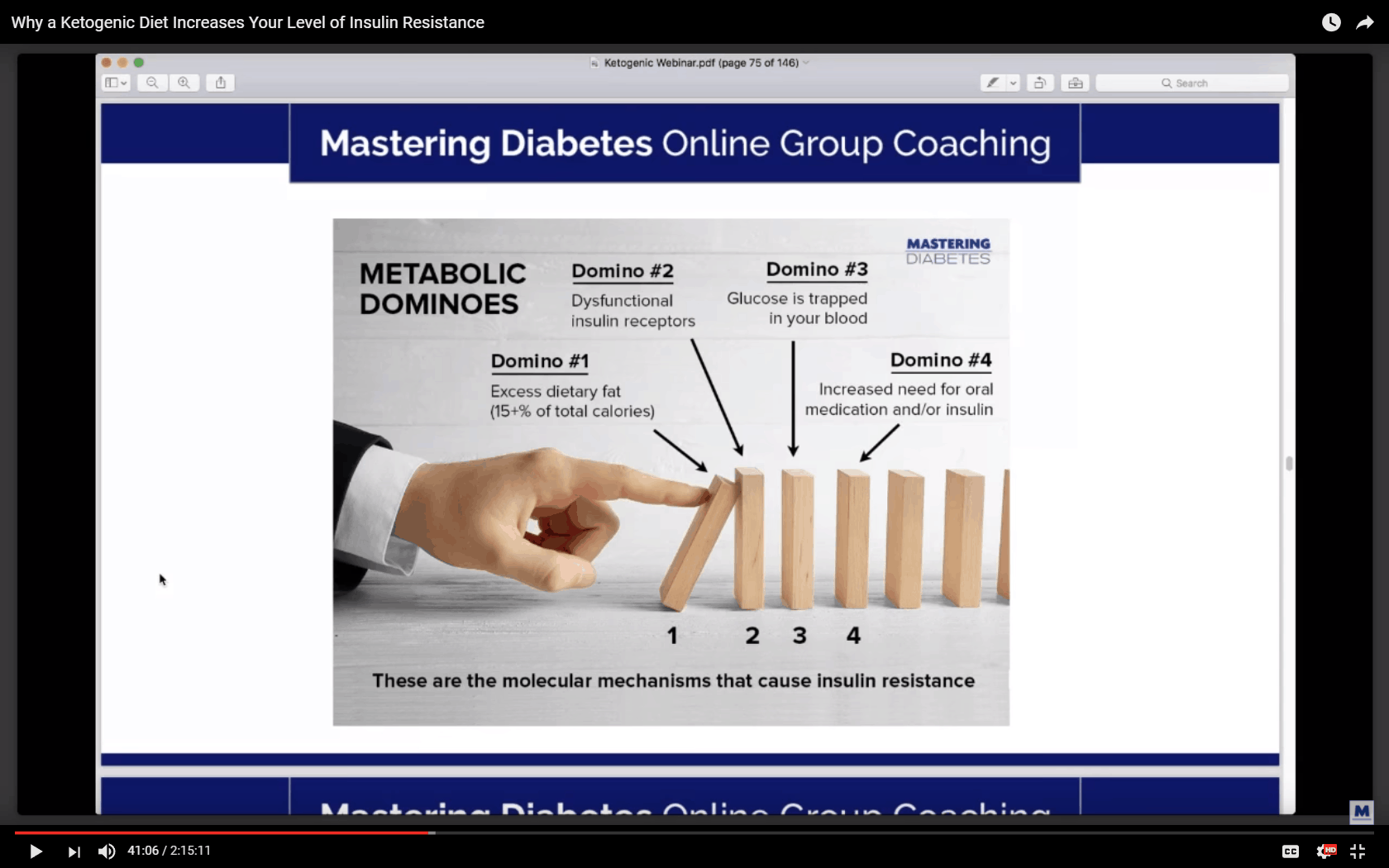
Unfortunately, Cyrus and Robby didn’t mention the benefits of a low-carb diet for people with diabetes which are fairly well documented. The seminal paper that summarises much of the latest work in this area is documented in Dietary carbohydrate restriction as the first approach in diabetes management: Critical review and evidence base.
Anyone who is on the fence about using a low-carb diet to manage diabetes should check out this paper which shows that a low-carb diet is better for weight, HbA1c, glucose, HDL and triglycerides compared to low GI or a grain-based diet.
Another well-known study is Christopher Gardener’s A to Z trial[24] where they found that the Atkins diet did much better than the low-fat, particularly if you were already insulin resistant.[25]
What should you eat if you are a vegan with diabetes?
So, after all this, what should we eat to maintain optimal blood sugar levels? Cyrus and Robby’s view is shown below. Unfortunately, it appears that their recommendations are driven more by their philosophical and ethical views rather than the nutrient content of the food or their ability to stabilise blood sugars.
- In the green column, most people with diabetes aren’t going to do too well with a lot of fruits, starchy veggies, and beans. Intact whole grains contain substantial nutrients but are very hard to find in our modern food system. Who eats wheat bran as a significant part of their diet? The vast majority of grains are processed with the nutrients discarded, so they are tasty and shelf-stable.
- In the red column, dairy eggs, meat, fish and poultry can be nutrient dense and keep your blood sugars stable (as long as you’re not afraid of fat in whole foods or ‘animal protein’).
- In the orange column, higher fat foods like nuts, seeds, avocados, coconut and olives can be useful to help stabilise your blood sugars, but it is possible to overconsume them if your goal is to lose weight.
We want to maximise nutrient density as much as possible while keeping the insulin load of our diet down to the point that we keep blood sugars stable.
This does not end up being super high fat or super low fat. Fat just comes along with nutritious whole foods.
If you have diabetes, then a little more dietary fat initially may help to stabilise blood sugars. Once your blood glucose levels have stabilised, you can start to decrease the dietary fat and increase nutrient density as much as you can while still maintaining excellent blood sugar levels.
A low insulin load, and diabetes-friendly plant-based nutritional approach will lack omega 3 and vitamin B-12.
I hope this is helpful for people who want to choose a plant-based approach to maximise nutrient density and maintain excellent blood sugar control.
So which approach is optimal?
It depends.
The optimal approach for you will depend on your situation and goals.
Going plant-based may be an improvement if your diet is currently full of sugar and processed grains, but it is not the singular solution to every ill. (For an excellent example of a very nutrient-dense plant-based dietary approach check out David’s Nutrient Optimiser analysis here.)
To help you make more informed food choices, I have devised two different ways of measuring food quality:
- Proportion of insulinogenic calories, and
- Nutrient density.
The proportion of insulinogenic calories is the percentage of the food you eat that will require insulin to metabolise. The table below lists a range of nutritional approaches ranked by the percentage of insulinogenic calories (right-hand column).
If you’re interested in any of these approaches, you can download the list and save it to your phone or print it out to take shopping for some inspiration.
| approach | foods | nutrient profile | % insulinogenic | |
| well-formulated ketogenic diet | foods | profile | 21 | |
| low carb | foods | profile | 34 | |
| plant-based (diabetes-friendly) | foods | profile | 56 | |
| weight loss and insulin resistance | foods | profile | 59 | |
| low carb pescitarian | foods | profile | 61 | |
| the most nutrient-dense foods | foods | profile | 67 | |
| plant-based | foods | profile | 68 | |
| plant-based (without ND) | profile | 73 |
Simply switching to a plant-based nutritional approach will leave you with 73% of your diet requiring insulin to metabolise. The diabetes-friendly plant-based approach will be an improvement, but a low-carb or ketogenic diet may be better if your goal is stable blood glucose levels.
Another way to look at things is nutrient density. You may have noticed the nutrient profiles shown above have a red dotted box. If a particular nutritional approach provides two times the Daily Recommended Intake for all essential nutrients, then you would get a perfect score of 100%. You can see below that the most nutritious foods below are pretty close to 100%.

By contrast, if we only focus on ‘plant-based foods’ nutritional outcome is not so flash. Thinking only in terms of plant-based is not automatically nutrient-dense.
I have sorted the various food lists in the table below based on their nutrient score. My suggestion is to start at the top with the most nutrient-dense foods and work your way down until you find an approach that suits your ethical framework or religious beliefs that will also enable you to stabilise your blood glucose levels (i.e. lower % insulinogenic calories).
| approach | score | foods | nutrient profile | % insulinogenic | |
| the most nutrient-dense foods | 99.7% | foods | profile | 67 | |
| weight loss and insulin resistance | 99.3% | foods | profile | 59 | |
| low carb pescitarian | 94.5% | foods | profile | 61 | |
| low carbohydrate | 81.0% | foods | profile | 34 | |
| plant-based | 78.0% | foods | profile | 68 | |
| plant-based (diabetes-friendly) | 76.0% | foods | profile | 56 | |
| well-formulated ketogenic diet | 74.0% | foods | profile | 21 | |
| plant-based (without ND) | 57.0% | profile | 73 |
Summary
- While many people choose plant-based foods exclusively, they are not necessarily a better dietary choice compared to a more varied diet.
- Someone following an exclusively plant-based approach will require supplementation with vitamin B-12, vitamin D and omega 3s.
- Fat is not necessarily good or bad. Swinging to macronutrient extremes will not lead to an optimal outcome.
- Reducing your diet’s insulin load will help normalise your blood sugar and insulin levels.
- Ideally, you should aim to achieve the blood sugars of a metabolically healthy person while maximising nutrient density at the same time.
How Can I Calculate My Nutrient Intake?
If you’re interested in checking if you’re getting just enough dietary phosphorus, you can check your nutrient profile using our Free 7-Day Nutrient Clarity Challenge. After a week of tracking your current diet in Cronometer, Nutrient Optimiser will give you a prioritised list of foods and NutriBooster recipes that will help you plug your current nutritional gaps.
More
References
[1]https://www.ncbi.nlm.nih.gov/pubmed/25515001
[2]https://optimisingnutrition.com/2015/07/20/the-glucose-ketone-relationship/
[3]https://www.ncbi.nlm.nih.gov/pmc/articles/PMC301822/
[4]https://www.quackwatch.org/01QuackeryRelatedTopics/DSH/coral2.html
[5]https://authoritynutrition.com/the-alkaline-diet-myth/
[6]https://optimisingnutrition.com/2017/03/19/micronutrients-at-macronutrient-extremes/
[7]https://socialblade.com/youtube/user/nutritionfactsorg
[8]https://nutritionfacts.org/donate/
[9]http://www.hsi.org/about/who_we_are/leadership/subject_experts/michael_greger.html
[10]https://www.facebook.com/mangomannutrition/videos/656469947843978/
[11]https://optimisingnutrition.com/2016/10/23/energy-density-food-hyper-palatability-and-reverse-engineering-optimal-foraging-theory/
[12]https://en.wikipedia.org/wiki/Optimal_foraging_theory
[13]http://www.hoajonline.com/obesity/2052-5966/2/2
[14]https://www.amazon.com/Dorito-Effect-Surprising-Truth-Flavor/dp/1476724237
[15]https://fineartamerica.com/featured/8-muscleart-marius-poser-classic-jake-hartz.html
[16]https://www.ncbi.nlm.nih.gov/pubmed/21241239
[17]https://optimisingnutrition.com/2015/08/10/insulin-dosing-options-for-type-1-diabetes/
[18]https://www.facebook.com/Type1Grit/
[19]https://optimisingnutrition.com/2015/07/20/the-glucose-ketone-relationship/
[20]https://www.ncbi.nlm.nih.gov/pmc/articles/PMC301822/
[21]http://online.liebertpub.com/doi/full/10.1089/met.2016.0108
[22]https://optimisingnutrition.com/2016/02/15/how-to-use-your-glucose-meter-as-a-fuel-gauge/
[23]http://ketotalk.com/2016/06/23-responding-to-the-paleo-mom-dr-sarah-ballantynes-claims-against-the-ketogenic-diet/
[24]http://jamanetwork.com/journals/jama/fullarticle/205916
[25]http://onlinelibrary.wiley.com/doi/10.1002/oby.21331/full





















Excellent work Marty as usual. You have hammered down the issue from an “either or” to “it depends”. My experience of some vegan doctors and followers are that they are almost tyrannical in seeking to impose that way of eat on everyone.
Totally tyrannical for someone to suggest a diet that is better for the planet and the 60 billion animals killed every year due to “personal” choice. Damn vegans and their compassion, why can’t they just understand that brutal slaughter is normal?
Reblogged this on Talmidimblogging.
Wow, outstanding post. Thank you!
Hi Marty Great message – I particularly liked your take on the speech by the other Martin. But, right at the end you state that the liver can hold 1200 to 2000 calories of glycogen. I believe it is much more like 400 calories and 1600 calories in the muscles. What is more, it’s only the liver glycogen that is available for maintaining basal blood glucose levels. Someone with a BMR of about 1600 calories in 24 hours ie 70 calories an hour, might expect to switch to fat burning after about 5-6 hours. This how the intermittent fasters lose up to 200g of fat every fasting day (as I did). I hope to see you at LCDU Gold Coast in October Cheers John Beaney
On Wed, Jul 26, 2017 at 2:52 AM, optimising nutrition wrote:
> Marty Kendall posted: “recently watched the Mastering Diabetes teleseminar > on ketogenic diets with high hopes of picking up some gems of wisdom from > the rising stars of the plant-based diabetes community. Unfortunately, I > was underwhelmed with what I heard. I shared my frus” >
Go to YouTube and watch “Simply Raw: reversing diabetes in 30 days”. Plant based diets have reversed diabetes, no omni diet can claim that.
Type 2 diabetes only. You cannot reverse type 1 diabetes. Check out Dr Jason Fung’s videos on YouTube. Intermittent fasting + low carb/nutritional ketogenic diets have shown to be effective at reversing type 2 diabetes as well.
“…no omni diet can claim that.”
How would you know? It isn’t possible to prove a negative. Anyway, depending on which type of diabetes we’re talking about, it’s absolutely true that Paleo or similar diets have eliminated the illness for many people. One of the most amusing conversation threads I’ve seen in the last several years about food nutrition and health is this one, where the American Diabetes Association posted to FB asking viewers to post their blood glucose numbers. The people doing worst were following the ADA recommendations for diet, while lots of people with improvement or no longer needing insulin products at all mentioned they are eating HPHF or LCHF diets.
https://www.facebook.com/AmericanDiabetesAssociation/posts/10153140618374033
I am not diabetic, but having tried both keto and vegan, I felt terrible on keto and feel wonderful on vegan. The fact that no animals are slaughtered is just a big bonus. I have much more energy less brain fog on vegan diet which includes much fat in the form of healthy vegetable oils. Dr. Gregor is not pro sugar and advocates for low glycemic fruit. I do a low carb vegan diet and am keeping weight off. My digestive system works much better on vegan diet.
That’s great. I’ve got no issue with people choosing an exclusively plant based approach if it works for them. However, I think a better understand of how things work will help people better manage their chosen approach.
Great article. It will take a while to understand it all.
Let me know if you have any questions.
Monica asked what else she could do to get the blood sugars down, but they had no advice. They just wanted to see them lower.
More fiber? That’s about the only thing I can think of. Of course, now there’s a whole slew of drugs designed just for that purpose–high A1C? Januvia to the rescue. Insulin alone not doing the job? Add Victoza! And on and on…
It’s getting to where a diabetic (of any stripe) is directed to take at least 3 injectable drugs along with insulin—cha-CHING for Big Pharma. “We’ve got a shot for that!”
Just a few days ago, Dr. Jason Fung posted an article that’s pretty much a step-by-step instruction to eliminating T2 diabetes by limiting the amount of food you eat so as to match the liver’s speed of processing: https://intensivedietarymanagement.com/medications-actually-work-type-2-diabetes-t2d-40/
In the 6th edition of the book “The ketogenic and modified Atkins diets: treatments for epilepsy and other disorders” on page 111, the writers define two ratios for ketogenic diets in children with epilepsy: 80-15-5 and 90-8-2 (F-P-C %). Have you tried micronutrient optimise those ratios? Obviously, when children are changing from SAD to ketogenic, rarely they are eating offal and mostly get their fat calories from heavy cream or MCT to gut tolerance.
Most people with diabetes will benefit with more nutrients from protein and non-starchy vegetables without needing to go to those extremes.
Thank you Marty for this informative and thorough post. I have to read ti again and try to absorb all the material.
Even after reading your post, I am still confused about Keto vs. Vegan philosophy. I am pre-diabetic with A1c that started at 5.8, went up to 6.4 and over the past 6-8 months is down to 5.6 again. Fasting glucose is in the 95-120 range.
I followed a low carb, almost Keto diet for about 4-5 months and lost about 20lbs. Then my weight leveled off and I could not lose anymore weight. I suppose it is the insulin that is holding on to my fat reserves.
Then I came across Dr. McDugall’s work and also learned about Cyrus. Their argument made sense to me. More so for health and not so much for animal rights part of it. So I started a vegan diet about four weeks ago. I have lost some more weight. However, I am not feeling any better. My neuropathy is still there and now I have chest pains at night and my sleep has been not so good for the past 3-4 months. I stopped taking metformin about 6 weeks ago because it did not do anything for me.
I am totally confused about this whole deal. I know advocates on both sides are well meaning but it is hard for me to decipher which path is the better one to take. In the meantime, I started a long overdue lone-term fast two days ago. I am hoping that this will clear the deck so to speak. Fasting seems to be universally accepted in both camps.
I would love to hear your and other people’s thoughts on this.
Oh goodness…that photo of Dom D’Agostino! Is it hot in here? Now I can’t concentrate. I think you were saying something about diabetes?
Thanks Marty! I hate propaganda and vegans are very skilled at it.
Great article. Just what I was looking for. Doing some research on the vegan diet as it is getting increasingly popular. The claim that high fat diet is creating insulin resistance is a recurring theme. I think that you explain well that this is a physiological response. One question: in your experience, when is insulin too low? And related to that I have often seen people on a low carb diet having their fasted glucose increase as well as having very low fasted (basal) insulin. Cause for concerns? Thanks!
A very low dietary insulin load will likely be super high fat. Physiological IR can be related to less minerals, but maybe the body just likes to run glucose a little higher. Maybe cause for concern if HbA1c is also elevated.
That’s right, That will happen mostly in patients with low insulin response especially patients with diabetes. Insulin sometimes will be lower than what required to manage good glucose state. This story will be recurring thing in patients with more than 10 years of uncontrolled diabetes who started low carb diet.
Best dietary strategy for managing Type 1 or Type 2 is the one that patient can implement with ease and balance between results and not feeling deprived. Non-diabetic is A1c is below 5.0, any other number is bull shit. Damage begins at 100mg/dl.
One caution to Cyrus and Robby’s methods is the extreme amount of fructose.
Look at the faces of both and you can see the aging skin while generally healthy looking due to high antioxidant status looks weathered/leathery/crumpled around the eyes wondering about other systemic effects due to abnormal collagen production caused by high fructose.
They could mitigate this with taurine/carnosine or similar supplements to lessen fructose negative effects and still maintain current diet.
High protein and high fat can increases dietary glycation and lipid peroxidation products which is not ideal.
High protein will also age due to impact on MTOR and IGF-1 levels. Can likely be mitigated through fasting and cycling protein content.
Switching things up and keeping body guessing and burning through reserves on occasion probably best bet.
This article was very helpful. I’m pre-diabetic, age 52, overweight by 30-40 lbs, post-menopausal and I want to stop this process now before it gets worse. I have done massive research, read numerous books/blogs/articles and with each one thought I found the answer only to get more confused by reading the next one. I too feel the vegan approach as taught by Cyrus and Robbie( along with other vegan doctors) just seemed too high carb with all that fruit. Keto is just too high fat (for my digestive liking and lack of gallbladder) to seem healthy for me. I am all for a healthier planet and limiting animal cruelty but my thought is that if total plant based is lacking in basic nutritional needs such as B12 and omega 3’s, then it surely can’t be the absolute solution. So your article put things in a better perspective for me in terms of better explaining the 2 camps. I’m hoping I can tackle this issue by choosing bits of both. Thanks again!